The best hydrogen peroxide percentage depends on your goals and sensitivity tolerance. Low concentrations (3%–6%) deliver gradual, sustainable results with minimal risk, while professional-grade concentrations (16%–35%) whiten faster but carry higher sensitivity risks. Research shows 6% achieves longer-lasting results at six months than 35%, despite 35% performing better immediately post-treatment. There’s no single “best” percentage — only the right one for your specific situation, and the details ahead will help you find it.
Key Takeaways
- Low concentrations (3%-6%) suit surface stains and sensitive teeth, while high concentrations (16%-35%) are better for deep or intrinsic staining.
- 35% hydrogen peroxide achieves faster results, with a 3.68-unit shade improvement immediately post-treatment versus 2.37 units for 6%.
- At six months, 6% hydrogen peroxide outperforms 35%, retaining a 1.95-unit improvement compared to 1.70 units.
- Higher concentrations increase risks of tooth sensitivity, gingival burns, and enamel microstructure disruption, requiring professional supervision.
- The best concentration depends on stain severity, sensitivity levels, desired speed of results, and professional oversight availability.
How Hydrogen Peroxide Whitens Teeth and Why Percentage Matters
Hydrogen peroxide whitens teeth through a straightforward oxidation process: once applied, it breaks down into water and oxygen radicals, which penetrate the enamel and dentin to disrupt the chemical bonds in chromogenic compounds—the molecules responsible for tooth discoloration.
Understanding these whitening mechanisms helps you make smarter product decisions.
Concentration effects are direct: higher percentages accelerate the oxidation reaction, producing faster and more dramatic shade changes, while lower percentages work more gradually with less tissue exposure.
However, speed doesn’t automatically mean better outcomes. Research shows that 6% hydrogen peroxide, used over a longer duration, can match or eventually surpass the long-term results of 35% treatments.
Selecting the right percentage means weighing your stain severity, sensitivity threshold, and whether you’re operating under professional supervision.
How Low and High Concentrations Whiten Teeth Differently
When you use a low-concentration product, such as a 6% hydrogen peroxide strip, you release oxidizing agents gradually, which produces slower shade changes but typically causes less sensitivity and tissue irritation.
Higher concentrations, such as the 35% gels used in dental offices, penetrate enamel more aggressively and deliver faster, more pronounced results—one study found that 35% hydrogen peroxide produced a 3.68-unit shade improvement immediately after treatment, compared to 2.37 units for 6%.
Understanding this tradeoff helps you match the concentration to your specific whitening goal, sensitivity threshold, and level of professional supervision.
Low Concentration Whitening Effects
Although both low and high hydrogen peroxide concentrations whiten teeth through the same oxidative mechanism, they differ considerably in speed and intensity of results.
Low concentrations, typically ranging from 3% to 10%, deliver gradual whitening by penetrating enamel slowly over multiple applications. This controlled pace is one of the primary low concentration benefits, as it minimizes tooth sensitivity and soft-tissue irritation during treatment.
Research supports their effectiveness. A comparative study found that 6% hydrogen peroxide produced a 2.17 shade improvement at three months, closely approaching the 2.60 improvement achieved with 35%.
Over six months, the 6% group actually retained stronger results. If you prioritize safety, tolerability, and sustained outcomes, gradual whitening with lower concentrations offers a clinically sound, self-directed approach.
High Concentration Whitening Effects
High concentrations, typically ranging from 16% to 35% in professional settings, penetrate enamel more aggressively and produce faster shade changes than their lower-concentration counterparts.
Research confirms this advantage is most pronounced immediately after treatment, where 35% hydrogen peroxide delivered a 3.68 shade-unit improvement compared to 2.37 units at 6%.
However, one of the most persistent whitening myths is that stronger always means better long-term results. By six months, the 35% group actually showed slightly less retention at 1.70 shade units versus 1.95 units.
If you’re weighing peroxide alternatives or considering professional treatment, understand that high concentrations demand supervision to manage sensitivity and soft-tissue risk.
Faster initial results come with trade-offs, and long-term outcome data should factor heavily into your decision.
What Percentage Is in Over-the-Counter Whitening Products?
Most over-the-counter whitening products contain hydrogen peroxide concentrations ranging from about 3% to 10%, with many popular whitening strips formulated at around 6%.
When evaluating over-the-counter effectiveness, you should recognize that product formulation directly influences how a product performs, including contact time, gel viscosity, and delivery method.
A strip designed for 30-minute daily application at 6% hydrogen peroxide can produce meaningful shade improvements over several weeks.
Lower concentrations, such as 3%, work more gradually and suit those with heightened sensitivity.
Concentrations approaching 10% accelerate results but may increase irritation risk.
Understanding these variables lets you select a product aligned with your stain severity, tolerance, and timeline rather than defaulting to the highest available concentration.
Why Professional Whitening Uses Much Higher Hydrogen Peroxide Percentages
Over-the-counter products cap their concentrations largely because unsupervised use demands a wider safety margin.
But when you move into a dental office, the clinical environment changes that equation entirely.
Professional techniques typically employ 16% to 40% hydrogen peroxide because supervised applications allow clinicians to monitor concentration effects in real time.
Professional whitening gels reach 16% to 40% hydrogen peroxide—concentrations made safe through real-time clinical supervision.
Your gingival tissue gets protected, exposure duration gets controlled, and treatment protocols get adjusted based on your response.
That level of oversight makes higher concentrations clinically appropriate.
When stain removal is your priority and time efficiency matters, professionally administered gels produce measurable shade changes faster than home products can.
Patient comfort remains manageable because the dentist controls every variable.
Higher concentration isn’t reckless here—it’s deliberate, matched precisely to your whitening goals under qualified supervision.
6% vs. 35% Hydrogen Peroxide: What the Research Actually Shows

A randomized controlled study comparing 6% and 35% hydrogen peroxide reveals a clear trade-off between immediate impact and long-term retention.
Immediately after treatment, the 35% group achieved a 3.68 shade-unit improvement versus 2.37 shade units in the 6% group, suggesting the higher concentration delivers faster initial results.
However, by the six-month mark, the gap reversed—the 6% group retained a 1.95 shade improvement while the 35% group had declined to 1.70, indicating that lower-concentration whitening can match or outlast higher-concentration results over time.
Immediate Results Compared
When researchers directly compared 6% and 35% hydrogen peroxide in a randomized controlled study, the higher concentration came out ahead—but not by as much as you might expect.
Immediately after treatment, the 35% group gained 3.68 shade units, while the 6% group gained 2.37 shade units. That’s a measurable difference, but it challenges common whitening myths that frame stronger formulas as categorically superior.
The gap is 1.31 shade units—not the dramatic divide that concentration confusion often implies. If you’re evaluating your options based on immediate outcomes alone, the higher concentration does deliver faster initial results.
However, that single data point doesn’t tell the complete story, and immediate post-treatment shade change is only one factor worth weighing before you choose a protocol.
Long-Term Effectiveness Fades
The immediate advantage of 35% hydrogen peroxide shrinks considerably when you look past the first treatment. At six months, the gap nearly reverses—6% delivers 1.95 shade units retained versus 1.70 for 35%.
Gradual results, it turns out, hold longer. Consider what the data actually shows:
- Week 1: 35% produces a sharper initial change you can see immediately.
- Month 3: The difference narrows to just 0.43 shade units.
- Month 6: 6% hydrogen peroxide outperforms 35% in retention.
- Long-term maintenance: Lower concentrations allow consistent reapplication without compounding sensitivity risks.
You’re not just choosing a percentage—you’re choosing a trajectory. If sustained whiteness matters more than a dramatic first impression, the lower concentration gives you more durable control.
The Best Hydrogen Peroxide Percentage for At-Home Whitening
For at-home whitening, 6% hydrogen peroxide is generally the most practical and evidence-supported choice. It aligns with established Concentration Guidelines and delivers meaningful shade improvement without requiring professional supervision.
Research confirms that 6% can produce results comparable to higher concentrations over time, making it a reliable option for DIY Whitening.
Studies show 6% hydrogen peroxide delivers results comparable to stronger concentrations, proving it a dependable DIY whitening solution.
If you have sensitive teeth, dropping to 3% reduces irritation risk while still providing gradual brightening.
Avoid exceeding 10% without dental oversight, as higher concentrations increase the likelihood of enamel damage and soft-tissue irritation.
Your choice should reflect stain severity, sensitivity history, and how frequently you plan to whiten.
Stronger isn’t always better—matching the concentration to your specific needs gives you both control and consistent, measurable results.
Sensitivity and Safety Risks at Higher Hydrogen Peroxide Percentages
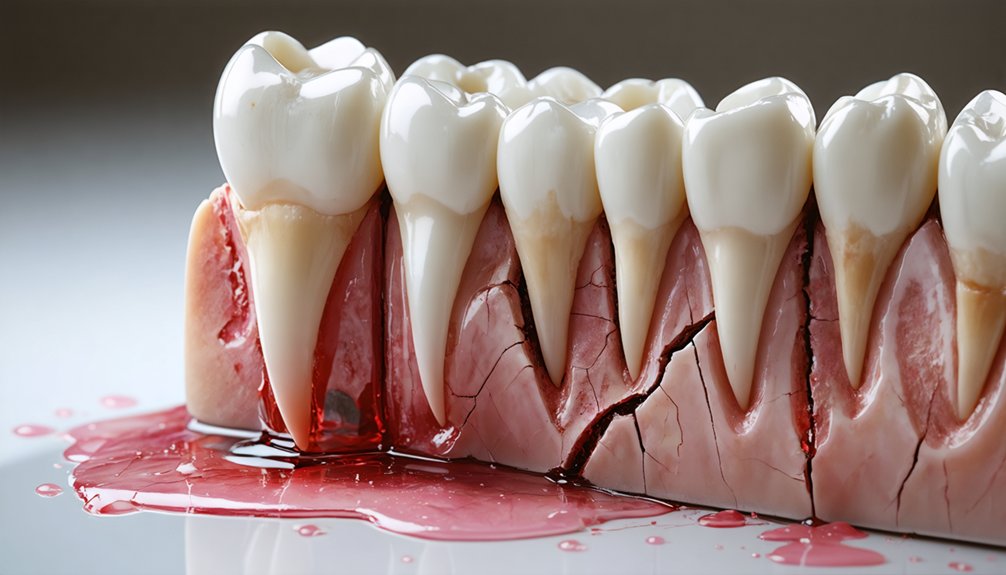
Higher hydrogen peroxide concentrations increase your risk of tooth sensitivity and soft-tissue irritation in direct proportion to their strength. Understanding these sensitivity risks lets you make informed, controlled decisions before starting treatment.
Higher concentrations introduce four specific hazards:
- Nerve irritation — peroxide penetrates enamel, triggering sharp, transient tooth sensitivity.
- Gingival chemical burns — concentrated gel contacting soft tissue causes visible blanching and discomfort.
- Enamel microstructure disruption — prolonged high-concentration exposure may compromise enamel integrity.
- Compounding sensitivity — repeated applications accelerate cumulative damage without adequate recovery time.
Applying safety measures reduces these risks considerably. Keep contact time within manufacturer guidelines, avoid concentrations above 6% without professional supervision, and discontinue use if sensitivity persists beyond 48 hours.
Control over your whitening outcome begins with respecting concentration limits.
Does a Higher Percentage Always Mean Better Results?
When you choose a higher hydrogen peroxide concentration, you may see faster initial shade improvement, but that short-term gain doesn’t always hold over time.
Research comparing 6% and 35% hydrogen peroxide found that while the 35% group achieved greater whitening immediately after treatment, the 6% group produced comparable results by six months.
You’re fundamentally trading speed and heightened sensitivity risk against a slower, gentler process that can still deliver meaningful, lasting whitening.
Short-Term Versus Long-Term
Although higher hydrogen peroxide concentrations produce faster initial shade changes, the long-term results don’t always reflect that early advantage.
Research comparing 6% and 35% hydrogen peroxide reveals how short term effects and long term effects can diverge considerably:
- Immediately post-treatment: 35% produced a 3.68-unit shade improvement versus 2.37 units for 6%.
- At 3 months: The gap narrowed — 35% yielded 2.60 units, while 6% held at 2.17 units.
- At 6 months: Results inverted — 6% maintained 1.95 units compared to 35% at 1.70 units.
- Takeaway: Lower concentrations with extended application can match or outlast aggressive short-term treatments.
You’re not sacrificing long-term outcomes by choosing a lower concentration — you’re often preserving them.
Sensitivity Versus Speed Tradeoff
Faster whitening comes at a cost. Higher concentrations accelerate speed optimization but increase your risk of tooth sensitivity and soft-tissue irritation.
A 35% formula delivers faster initial shade change than a 6% formula, but that advantage narrows considerably over time. Research shows that at six months, the lower-concentration group actually maintained better results.
If you’re prioritizing sensitivity management, lower concentrations reduce adverse effects without sacrificing long-term outcome. Higher percentages don’t automatically mean better whitening—they mean faster whitening, which isn’t always the same thing.
Your decision should account for your current sensitivity threshold, your timeline, and whether you have professional oversight. Choosing the wrong concentration doesn’t optimize results; it creates complications that slow your progress and compromise your comfort.
When to Go Higher and Let a Dentist Take Over
There are situations where over-the-counter concentrations simply won’t cut it, and pushing higher on your own isn’t the answer. A dentist consultation becomes necessary when:
- Your staining runs deep — tetracycline discoloration or fluorosis won’t respond adequately to 6% strips.
- You need rapid results — professional whitening methods using 16%–35% hydrogen peroxide can produce measurable shade changes in a single session.
- You’ve hit a plateau — if home whitening stops progressing, supervised higher-concentration gels can break through.
- Sensitivity is already present — a dentist can apply protective barriers and manage exposure time, reducing risk at stronger concentrations.
Controlled clinical data confirms that 35% hydrogen peroxide delivers faster initial shade changes.
Supervision doesn’t limit your options — it expands them safely.
Which Hydrogen Peroxide Percentage Fits Your Specific Situation?
Choosing the right hydrogen peroxide percentage comes down to three variables: stain severity, sensitivity level, and whether professional supervision is involved.
If you’re managing surface stains from coffee or tea with regular whitening frequency, 6% hydrogen peroxide delivers reliable results with minimal irritation risk.
For intrinsic stain types—those caused by aging, medications, or trauma—lower concentrations require extended treatment durations and may still fall short. In that case, professionally supervised concentrations between 16% and 35% produce faster, more significant shade changes.
Intrinsic stains from aging or trauma often demand professional-grade concentrations of 16–35% for meaningful results.
If sensitivity is your primary concern, 3% to 6% applied less frequently offers better tolerability.
Match the percentage to your specific clinical picture rather than defaulting to the highest available strength, since research confirms that higher concentration doesn’t always guarantee superior long-term outcomes.
Frequently Asked Questions
Can Hydrogen Peroxide Whitening Permanently Damage Tooth Enamel Over Time?
Like sandpaper on wood, overuse wears you down. Misusing hydrogen peroxide can cause long term effects on tooth enamel, but you’ll avoid permanent damage if you follow concentration guidelines and dentist-recommended protocols consistently.
Is Hydrogen Peroxide Whitening Safe to Use During Pregnancy?
You should avoid hydrogen peroxide whitening during pregnancy. Current evidence on hydrogen peroxide safety for pregnancy oral health remains limited, so dentists strongly recommend postponing whitening treatments until after delivery to eliminate any potential risk.
Can Hydrogen Peroxide Whiten Dental Crowns, Veneers, or Bonded Teeth?
Like painting a sealed canvas, hydrogen peroxide won’t whiten crowns or alter veneers safety profiles—it’s ineffective on restorations. You’ll find crowns whitening impossible since peroxide only affects natural enamel, leaving restorations unchanged.
How Does Hydrogen Peroxide Whitening Interact With Existing Dental Restorations?
Hydrogen peroxide won’t alter your restoration types—crowns, veneers, and bonding resist bleaching agents. You’ll notice color mismatches as natural teeth lighten. Watch for sensitivity issues around restoration margins, and consult your dentist before proceeding.
Does Drinking Water After Whitening Affect Hydrogen Peroxide Effectiveness?
Harmless as it seems, drinking water won’t undermine your whitening techniques or oral hygiene routine. You’re safe to hydrate freely, as water doesn’t neutralize hydrogen peroxide’s active whitening process once it’s already bonded to enamel.
References
- https://www.laserglowspa.com/blogs/news/teeth-whitening-gel-strength-guide
- https://www.youtube.com/watch?v=owavFFnn-pQ
- https://pubmed.ncbi.nlm.nih.gov/25799793/
- https://www.healthline.com/health/hydrogen-peroxide-teeth-whitening
- https://www.gentledental.com/resources/articles/hydrogen-peroxide-teeth-whitening
- https://www.urmc.rochester.edu/news/publications/health-matters/diy-teeth-whitening-too-good-to-be-true
- https://drgeorges.com/dental-white/teeth-whitening-system-comparisons/
- https://www.medicalnewstoday.com/articles/326148
- https://www.colgate.com/en-sa/oral-health/teeth-whitening/hydrogen-peroxide-toothpaste-four-common-questions
- https://www.ada.org/resources/ada-library/oral-health-topics/whitening