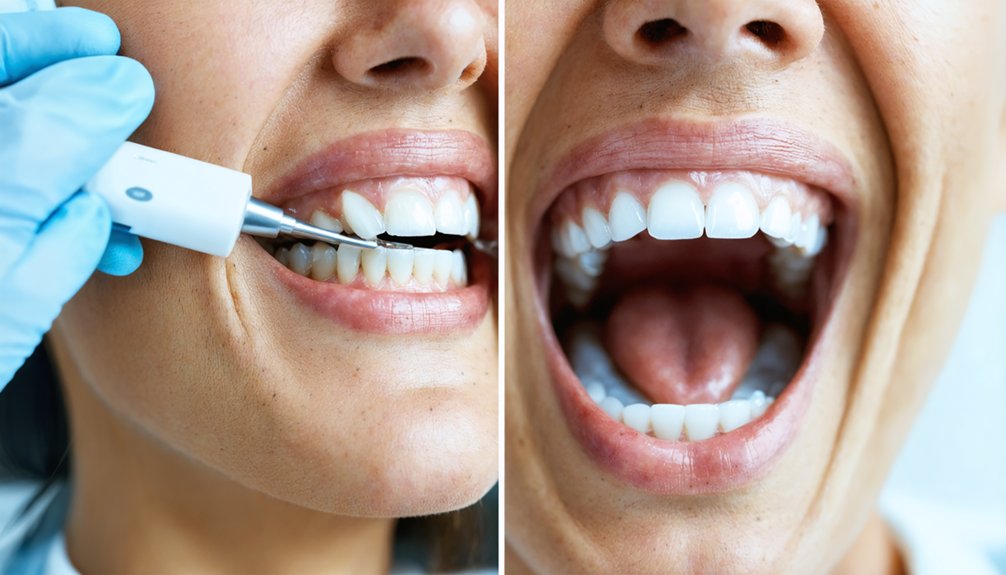
If you have sensitive teeth, you can still whiten at home safely by choosing the right products and approach. Use lower-concentration peroxide formulas, look for desensitizing ingredients like potassium nitrate and fluoride, and shorten your whitening sessions to reduce nerve irritation. Always prep with sensitivity toothpaste before treatment and avoid acidic foods throughout the process. The tips and product guidance ahead will help you build a whitening routine that actually works for your teeth.
Key Takeaways
- Choose whitening products with lower peroxide concentrations and desensitizing ingredients like potassium nitrate and fluoride to minimize irritation.
- Start with whitening toothpaste as a gentle introduction, delivering gradual results while protecting sensitive enamel daily.
- Apply sensitivity toothpaste before and after whitening sessions to calm nerve activity and reduce post-treatment discomfort.
- Space out whitening sessions by skipping alternating days, starting with half the recommended wear time to build tolerance.
- Avoid acidic foods, abrasive products, and use a soft-bristled toothbrush to protect enamel throughout the whitening process.
Why Do Sensitive Teeth React Badly to Whitening?
Whitening products work by using peroxide-based agents to penetrate enamel and break down stain molecules — but if your teeth are already sensitive, that same penetration can trigger sharp discomfort.
Thin or compromised enamel exposes the underlying dentin, where microscopic tubules connect directly to nerve endings. When peroxide reaches those tubules, it can activate pain signals almost immediately.
Peroxide doesn’t just whiten — it penetrates, and compromised enamel gives it a direct path straight to your nerves.
Tooth sensitivity during whitening isn’t random — it’s a physiological response you can anticipate and manage.
One of the most persistent whitening myths is that stronger formulas produce better results faster. In reality, higher concentrations often worsen sensitivity without delivering proportional benefits.
Understanding the mechanism behind your discomfort puts you in a stronger position to choose the right product, concentration, and application strategy.
Which Whitening Ingredients Are Safest for Sensitive Teeth?
When choosing a whitening product for sensitive teeth, you’ll want to focus on two key factors: the type of active whitening ingredient and the supportive agents included in the formula.
Hydrogen peroxide and carbamide peroxide are the primary effective actives in OTC whitening products, and lower concentrations generally reduce the risk of irritation without sacrificing results.
Alongside these actives, look for soothing ingredients like potassium nitrate, fluoride, and xylitol, which help calm nerve sensitivity, reinforce enamel, and support overall oral health during the whitening process.
Low-Irritation Whitening Actives
For sensitive teeth, the choice of whitening active matters as much as the method itself. Hydrogen peroxide and carbamide peroxide are the primary OTC whitening agents, but concentration determines your tolerance.
Lower concentrations function as low irritation alternatives that still deliver effective concentrations for visible results without overwhelming nerve endings.
Potassium nitrate is frequently added to calm tooth nerves, making it a clinically recognized support ingredient during whitening. Fluoride reinforces enamel integrity, reducing vulnerability to post-whitening sensitivity.
Some formulas also incorporate xylitol for broader oral-care support.
If you’re managing sensitivity, prioritize products that pair a peroxide-based active with potassium nitrate or fluoride. This combination lets you pursue meaningful whitening results while keeping discomfort within a manageable range.
Soothing Supportive Ingredients
Beyond the active whitening agents, the supporting ingredients in your formula play a direct role in how well your teeth tolerate the process. Soothing agents like potassium nitrate work by calming the nerve activity inside the tooth, reducing the sharp sensitivity that whitening can trigger.
Fluoride reinforces enamel integrity, helping offset mineral loss that occurs during treatment. Xylitol, found in select gentle formulations, supports oral health without adding irritation.
When you choose a product, check that it combines these supportive ingredients alongside the active whitening compound. Potassium nitrate is most effective when used consistently—twice daily before and during your whitening routine.
Fluoride rinses can provide additional enamel protection post-treatment. These ingredients don’t whiten on their own, but they make effective whitening considerably more tolerable.
Use Sensitivity Toothpaste Before and After Every Treatment
Using a sensitivity toothpaste before each whitening session helps build a protective baseline by calming nerve activity in your teeth ahead of chemical exposure.
After treatment, apply the toothpaste directly to your teeth and leave it on for several minutes rather than rinsing immediately, allowing the active ingredients to penetrate and reduce post-whitening discomfort.
Potassium nitrate, the key desensitizing compound in most sensitivity formulas, works by blocking dentinal tubules and quieting nerve signals, making it one of the most clinically supported options for managing whitening-related sensitivity.
Pre-Treatment Toothpaste Benefits
Before you apply any whitening product, brushing with a sensitivity toothpaste can help calm nerve activity and reduce the likelihood of post-treatment discomfort.
The pre-treatment benefits of this step are rooted in how active ingredients like potassium nitrate work — they penetrate the dentinal tubules and progressively block pain signals before whitening agents ever contact your enamel.
Using a potassium nitrate-based toothpaste twice daily in the days leading up to treatment allows the desensitizing compound to accumulate, which helps blunt the sensitivity effects that hydrogen peroxide or carbamide peroxide can trigger.
This isn’t optional preparation — it’s a clinically informed strategy. You’re fundamentally building a buffer against nerve stimulation before introducing an active oxidizing agent into your routine.
Post-Whitening Application Tips
The pre-treatment window isn’t the only time sensitivity toothpaste earns its place in your whitening routine. Post whitening care matters just as much.
After each session, apply a potassium nitrate-based sensitivity toothpaste directly to your teeth and leave it on for several minutes before rinsing. This step helps calm irritated nerves and supports enamel protection when your teeth are most vulnerable.
You can also use a fluoride rinse after whitening to reinforce enamel and reduce residual discomfort.
Twice-daily use of sensitivity toothpaste throughout your whitening cycle—not just on treatment days—builds a more consistent protective effect. Skipping this step leaves a gap in your protocol that can amplify sensitivity and undermine results.
Make post-treatment application a non-negotiable part of your routine.
Potassium Nitrate’s Soothing Role
Potassium nitrate works by penetrating the dentinal tubules and calming the nerve signals responsible for whitening-induced sensitivity. Its potassium nitrate benefits extend beyond comfort—consistent use builds cumulative sensitivity relief over time.
To maximize its protective effect:
- Before whitening: Apply a potassium nitrate toothpaste twice daily for at least two weeks prior to starting treatment.
- Immediately after whitening: Brush with a potassium nitrate formula to intercept nerve activation before discomfort sets in.
- Between sessions: Continue twice-daily use to sustain the desensitizing effect throughout your whitening cycle.
You’re reinforcing a physiological barrier with each application. Skipping this step removes a critical layer of protection. Treat it as non-negotiable within your whitening protocol—not an optional add-on.
Start With Whitening Toothpaste for the Gentlest Results

If you’re just starting out with whitening and have sensitive teeth, whitening toothpaste is often the safest entry point. It delivers gradual results while minimizing the irritation risk associated with higher-concentration peroxide products.
Sensitivity-focused formulas typically combine mild abrasives for stain removal with desensitizing agents like potassium nitrate and fluoride, giving you both whitening and protective benefits in one step.
Incorporating whitening toothpaste into your daily whitening routine requires no additional tools or timing adjustments—you simply replace your regular toothpaste. Options like Sensodyne Extra Whitening, Sensodyne Clinical White, and Sensodyne Pronamel Gentle Whitening are formulated specifically for this balance.
Progress is slower than strips or gels, but if sensitivity has limited you before, this approach gives you a controlled, sustainable starting point.
Which Whitening Strips Work Best for Sensitive Teeth?
When whitening toothpaste isn’t delivering results fast enough, strips designed for sensitive teeth offer a meaningful step up without the harshness of standard formulas.
Among whitening strip types, look for these clinically relevant features that support sensitivity reduction:
- Lower hydrogen peroxide concentration — Crest Whitestrips Sensitive uses approximately 5.25% hydrogen peroxide, reducing irritation while still producing visible results.
- Shorter wear intervals — Choose strips with 9- to 30-minute application windows, and start at the lower end to assess your tolerance before extending sessions.
- Desensitizing additives — Some formulas include potassium nitrate or fluoride to calm nerve response during treatment.
You control the pace. Skipping days between applications lets your enamel recover without sacrificing your overall whitening progress.
Apply Whitening Gels Without Triggering Sensitivity
Whitening gels give you more control over concentration and application than strips do, but that flexibility also means you can inadvertently overexpose your enamel if you’re not careful.
Start with formulas containing 10% to 15% hydrogen peroxide and apply thin, even layers using precise gel application techniques to avoid gum contact.
Wear time matters greatly — don’t exceed the labeled duration, and consider starting with shorter sessions before gradually increasing exposure.
For effective sensitivity management strategies, apply potassium nitrate toothpaste twice daily before beginning your whitening cycle, and use a fluoride rinse immediately after each session.
Skip application days when discomfort persists rather than pushing through.
Address any existing cavities or enamel damage beforehand, since compromised teeth will react more intensely to peroxide-based formulas.
Shorten Whitening Sessions to Protect Sensitive Teeth
Shorter whitening sessions are one of the most effective ways to reduce peroxide-related sensitivity without abandoning your results. Rather than following maximum wear times, start conservatively and adjust based on your tolerance.
Shorter whitening sessions reduce sensitivity without sacrificing results — start conservatively and adjust based on your tolerance.
Reducing whitening frequency also gives your enamel recovery time between applications.
Use these session-management strategies for better sensitivity management:
- Start at half the labeled wear time — increase gradually only if you’re tolerating it well.
- Skip alternating days — spacing applications reduces cumulative peroxide exposure without sacrificing meaningful progress.
- Don’t exceed the recommended time — overextending strips or gels increases discomfort and enamel stress without improving results.
You control the pace. A slower, consistent approach typically delivers better long-term outcomes than aggressive whitening sessions.
Cut Acidic Foods and Abrasive Products During Whitening

What you eat and how you brush during whitening can either protect your progress or undermine it. Acidic foods and beverages — including citrus, soda, coffee, and wine — weaken enamel temporarily, making teeth more vulnerable to sensitivity and staining.
Rinse with water after consuming them, or use a straw to minimize direct tooth contact.
Abrasive products like baking soda and activated charcoal may seem effective, but overuse accelerates enamel erosion and worsens sensitivity.
Stick with a soft-bristled toothbrush and apply light pressure.
Before starting any whitening regimen, address existing dental concerns — cavities, cracks, or gum disease — since these conditions amplify irritation.
Controlling your diet and product choices gives you a meaningful advantage in managing whitening discomfort effectively.
Should You See a Dentist Before Whitening at Home?
Before starting any at-home whitening regimen, seeing a dentist can help you avoid complications that no OTC product is designed to handle. A professional whitening assessment identifies issues that make whitening unsafe or ineffective without prior treatment.
Schedule a dentist consultation if you have any of the following:
- Active cavities or cracks – Whitening agents penetrate compromised enamel and cause sharp, lasting sensitivity.
- Gum recession or disease – Exposed root surfaces don’t respond to whitening and are highly vulnerable to irritation.
- Recent dental restorations – Crowns, veneers, and bonding won’t whiten, creating uneven color results.
Addressing these conditions first gives you a controlled baseline.
You’ll choose products more precisely and reduce the risk of setbacks that force you to stop treatment entirely.
Frequently Asked Questions
Can Whitening Products Damage Dental Crowns, Veneers, or Bonding Work?
Whitening product ingredients won’t alter dental restoration effects—your crowns, veneers, and bonding resist bleaching agents, yet your natural teeth lighten. This mismatch can create visible color inconsistencies, so consult your dentist before starting any whitening regimen.
How Long Do At-Home Whitening Results Typically Last for Sensitive Teeth?
Your at-home whitening results typically last three to six months before sensitivity triggers like acidic foods and dark beverages accelerate staining. You’ll extend whitening duration by maintaining a consistent desensitizing toothpaste routine and avoiding known enamel stressors between treatments.
Is Teeth Whitening Safe to Use During Pregnancy or Breastfeeding?
You should avoid teeth whitening during pregnancy or breastfeeding due to unresolved safety concerns around peroxide absorption. Instead, explore alternative methods like sensitivity toothpaste to maintain oral health until it’s clinically appropriate to resume whitening treatments.
Can Children or Teenagers Safely Use At-Home Whitening Products?
Most dentists don’t recommend at-home whitening for children, and age restrictions vary by product. You should follow each product’s product recommendations closely and consult your dentist before allowing teenagers to begin any whitening regimen.
Does Drinking More Water During Whitening Help Reduce Tooth Sensitivity?
Like a shield, water benefits your whitening routine. You can rinse after meals to reduce acid exposure, supporting sensitivity reduction. It won’t replace desensitizing products, but it’s a simple, protective habit worth maintaining.
References
- https://www.youtube.com/watch?v=E1ln0LeqNnU
- https://www.dentalgroupofamarillo.com/brightening-smiles-gently-how-to-whiten-sensitive-teeth-without-the-ouch/
- https://www.forbes.com/sites/forbes-personal-shopper/article/best-whitening-product-for-sensitive-teeth/
- https://deandentalsolutions.com/how-to-whiten-your-sensitive-teeth-safely/
- https://www.health.com/beauty/best-whitening-products-sensitive-teeth
- https://www.sensodyne.com/en-us/oral-health-tips/whitening-sensitive-teeth/what-to-know/
- http://www.goochlanddentistry.com/whats-the-best-teeth-whitener-for-sensitive-teeth/
- https://www.goodrx.com/conditions/dental-care/sensitive-teeth-after-whitening
- https://www.healthline.com/nutrition/whiten-teeth-naturally
- https://www.colgate.com/en-us/oral-health/tooth-sensitivity/managing-sensitive-teeth-after-whitening