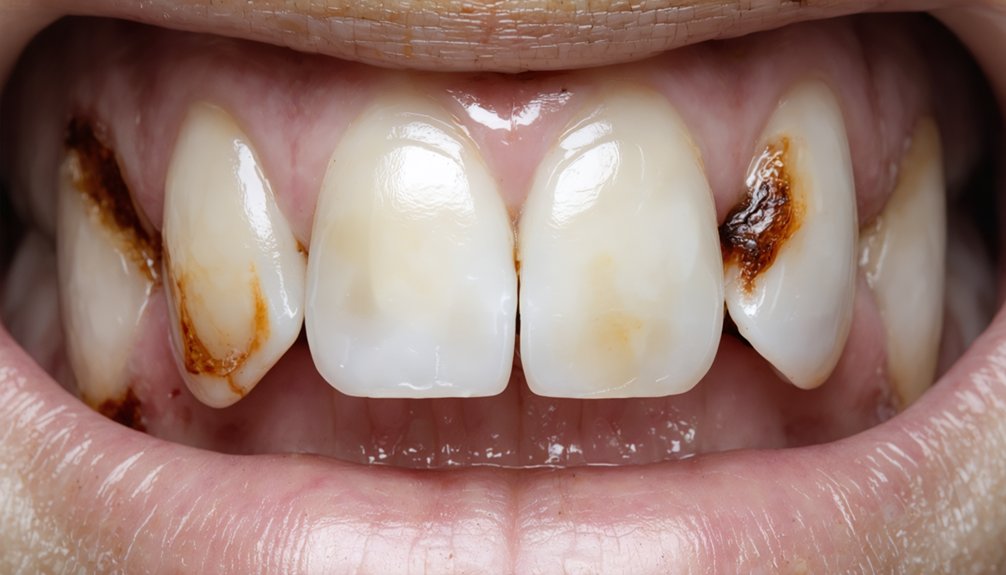
When you skip brushing and flossing, bacterial plaque colonizes your tooth surfaces and triggers a cascade of chemical and structural changes that stain your teeth from the inside out. Acidic plaque erodes enamel, exposing the darker dentin beneath. Hardened plaque calcifies into porous tartar, trapping chromogenic pigments that resist removal. Neglected gum tissue breaks down, exposing unprotected root surfaces that absorb stains rapidly. The full mechanisms behind each stage reveal just how preventable this damage truly is.
Key Takeaways
- Bacterial plaque produces acids that erode enamel, exposing darker dentin underneath and causing a yellowed appearance that worsens over time.
- Plaque acts as a stain reservoir, trapping pigments from food and beverages directly onto unbrushed tooth surfaces.
- Hardened plaque calcifies into porous tartar, which deeply absorbs chromogenic compounds and resists removal through regular brushing.
- Enamel erosion creates porous surfaces that trap deeper stains, leading to intrinsic discoloration that surface treatments cannot reverse.
- Gum inflammation exposes enamel-free tooth roots, which absorb pigments faster and accelerate overall teeth discoloration.
How Neglected Oral Hygiene Stains Teeth From the Inside Out
When oral hygiene is neglected, the damage doesn’t stop at the surface — it progresses inward, altering tooth structure at a cellular level. Acidic plaque erodes your enamel over time, exposing the darker dentin beneath.
Once that protective layer thins, you’re not dealing with surface staining anymore — you’re dealing with intrinsic discoloration that no whitening toothpaste can reverse.
Your stain prevention strategy must address this internal vulnerability. Without consistent oral hygiene, bacteria metabolize sugars into acids that systematically break down enamel, accelerating dentin exposure.
The yellowing you see isn’t just cosmetic — it’s structural evidence of ongoing tissue degradation. You can’t correct internal discoloration with surface-level solutions.
Only disciplined daily care stops the progression before irreversible structural changes compromise your teeth permanently.
Plaque Buildup: The First Step Toward Discolored Teeth
Plaque buildup is the foundational trigger for teeth discoloration, making consistent oral hygiene your first line of defense. When you neglect brushing and flossing, bacterial plaque accumulates on enamel surfaces, producing acids that erode protective layers and expose yellower dentin beneath.
Plaque effects extend further — stains from coffee, tobacco, and dark foods embed readily into unbrushed surfaces, accelerating discoloration. Hardened plaque calcifies into tartar, which resists home removal and permanently traps pigments.
Understanding these plaque effects clarifies why whitening methods alone won’t resolve discoloration rooted in poor hygiene — whitening methods target surface stains, not active plaque or tartar. You must eliminate plaque through twice-daily brushing, daily flossing, and professional cleanings before any whitening intervention produces lasting, clinically meaningful results.
Tartar Escalates Staining in Ways Plaque Never Could
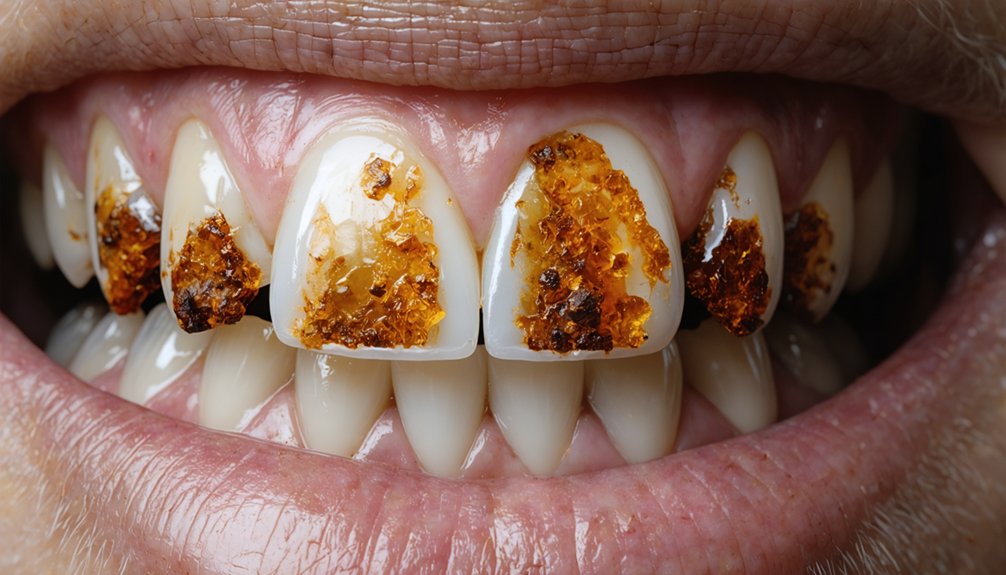
Once tartar forms on your teeth, it acts as a highly porous surface that actively traps pigments from coffee, tea, tobacco, and dark foods, embedding stains far deeper than soft plaque ever could.
Unlike plaque, which you can remove through consistent brushing and flossing, hardened tartar resists all home-care interventions due to its calcified, mineralized structure.
You’ll require professional scaling and debridement from a dental clinician to effectively break down tartar deposits and address the discoloration it has caused.
Tartar Traps Persistent Stains
Tartar’s capacity to trap and retain stains far exceeds that of soft plaque, making it a markedly more damaging contributor to tooth discoloration. Its porous, calcified structure actively absorbs pigments from food, beverages, and tobacco, embedding them beyond your reach.
Without professional tartar removal, these stains become chemically bonded to enamel surfaces, resisting all home-based stain prevention efforts. You’re left with discoloration that compounds over time.
Key mechanisms driving tartar-related staining include:
- Porous absorption: Tartar’s calcified matrix draws in chromogenic compounds from coffee, tea, and tobacco.
- Pigment retention: Embedded stains resist brushing, whitening toothpastes, and rinses.
- Progressive darkening: Each staining episode intensifies discoloration as tartar accumulates additional deposits.
Reclaiming control requires scheduled professional cleanings before staining becomes entrenched.
Professional Removal Becomes Necessary
When tartar calcifies onto enamel, it crosses a threshold that no toothbrush or over-the-counter product can reverse. At that point, you’ve lost the ability to manage discoloration independently.
Tartar’s mineralized matrix bonds to enamel at a structural level, locking in pigments from food, beverages, and bacteria. Standard dental hygiene practices can’t fracture that bond.
Only professional cleanings using ultrasonic scalers or hand instruments can mechanically debride calcified deposits without damaging underlying enamel.
Delaying treatment doesn’t pause the process — it accelerates it. Each additional layer of tartar compounds the staining, driving pigmentation deeper into the tooth’s surface architecture.
You retain control only by acting before calcification occurs. Once it does, professional intervention isn’t optional — it’s the sole clinically validated path to restoration.
Enamel Erosion and the Tooth Discoloration It Reveals
Enamel erosion, driven by acidic plaque accumulation from poor oral hygiene, progressively wears down the tooth’s protective outer layer, exposing the darker dentin beneath.
This intrinsic discoloration can’t be reversed with surface-level treatments alone. Maintaining enamel strength requires consistent, evidence-based hygiene practices before erosion advances.
Neglecting brushing and flossing accelerates enamel breakdown through these mechanisms:
- Acidic bacterial byproducts in plaque demineralize enamel, reducing its structural integrity.
- Thinning enamel increases dentin visibility, producing a permanent yellow undertone.
- Eroded surfaces become increasingly porous, trapping stains deeper within the tooth structure.
Once dentin exposure occurs, you’re dealing with a structural problem, not merely a cosmetic one.
Early intervention through disciplined oral hygiene directly controls erosion progression and preserves your enamel’s protective capacity.
How Tooth Decay Creates Dark Spots and Stains
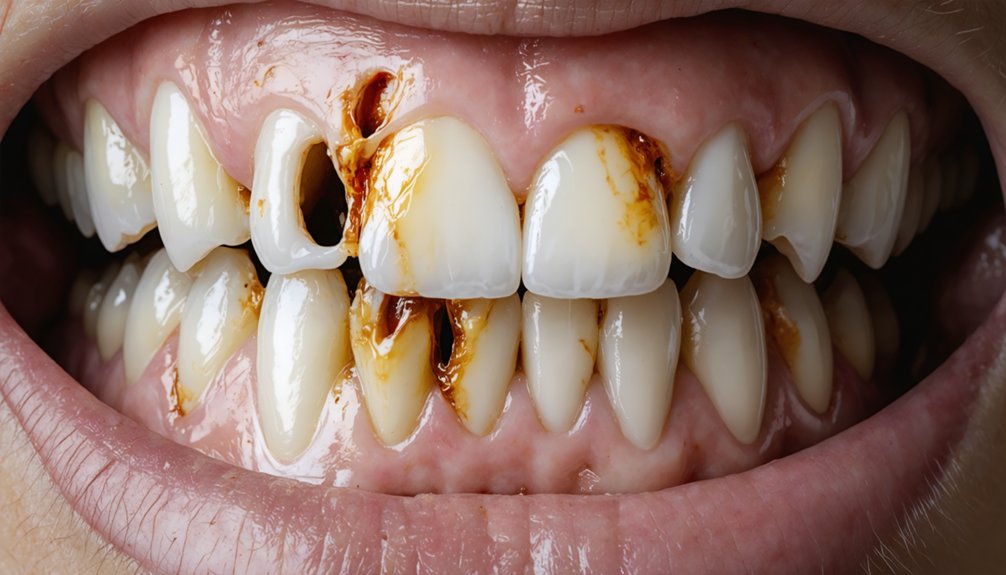
Beyond enamel erosion, poor oral hygiene sets the stage for a more destructive process: tooth decay. When you neglect brushing and flossing, bacteria effects intensify—plaque acids penetrate weakened enamel, initiating cavity formation.
These cavities manifest as dark spots, ranging from brown to black, signaling irreversible structural damage.
Hygiene neglect accelerates enamel impact by allowing bacterial colonies to metabolize sugars, producing acids that destroy tooth structure progressively. Untreated cavities deepen, exposing dentin and pulp, creating visible discoloration that no whitening treatment reverses.
Your treatment options at this stage include fillings, crowns, or extractions—all invasive and costly.
Preventive measures remain your strongest defense: twice-daily brushing, daily flossing, and routine professional cleanings disrupt bacterial activity before decay establishes, preserving both tooth structure and natural color.
Why Stains Stick Harder to Unbrushed Teeth
Unbrushed teeth accumulate plaque—a sticky, bacteria-laden biofilm that acts as a primary adhesion site for dietary and environmental stains.
When you neglect cleaning frequency, plaque’s porous structure absorbs chromogens from coffee, tobacco, and dark foods, dramatically increasing stain adhesion at the molecular level.
Key mechanisms driving this process include:
- Plaque porosity: Unremoved biofilm creates microscopic channels that trap pigmented compounds deeper into enamel surfaces.
- Surface roughness: Plaque-covered enamel becomes texturally irregular, giving staining agents more surface area to bond.
- Tartar conversion: Hardened plaque locks stains permanently, making professional intervention necessary for removal.
You control this outcome entirely through consistent brushing and flossing.
Disrupting plaque before mineralization eliminates the primary adhesion matrix, preventing chromogen penetration and maintaining enamel’s natural, stain-resistant surface integrity.
How Gum Disease Makes Tooth Discoloration Even Worse

When gum disease develops from neglected oral hygiene, it compounds tooth discoloration through mechanisms that extend well beyond surface staining. Gum inflammation triggers bacterial proliferation beneath the gumline, accelerating tissue breakdown and exposing tooth roots that lack protective enamel coverage.
These exposed root surfaces stain considerably faster than enamel, absorbing pigments from food, beverages, and tobacco with minimal resistance.
As periodontal disease advances, receding gums reveal darker dentin structures, creating an inherently discolored appearance independent of external staining agents.
Bacteria proliferation within infected pockets produces metabolic byproducts that further compromise surrounding tooth structures. You can’t reverse exposed root discoloration through brushing alone—professional intervention becomes mandatory.
Controlling gum disease early gives you the only reliable pathway to preventing this accelerated, multi-layered discoloration process.
Why Coffee and Dark Foods Stain Plaque-Covered Teeth Faster
When you neglect brushing, plaque accumulates on your enamel and acts as a porous matrix that actively traps chromogens—the dark pigment compounds found in coffee, tea, and foods like berries.
These chromogens bind to the sticky biofilm far more readily than they’d to clean enamel, accelerating stain absorption and penetration.
Without consistent mechanical removal, you’re effectively allowing plaque to function as a permanent stain reservoir on your tooth surfaces.
Plaque Traps Dark Pigments
Plaque acts as a sponge for chromogenic compounds, binding dark pigments from coffee, tea, and deeply colored foods far more readily than clean enamel. Its porous, bacterial matrix locks in plaque pigments, accelerating dark discoloration that routine rinsing won’t reverse.
Understanding this mechanism gives you actionable control:
- Chromogen adhesion: Plaque’s sticky biofilm chemically bonds dark pigments, embedding stains beneath the surface layer.
- Accelerated penetration: Uncleaned enamel surfaces allow beverages like coffee to saturate plaque within minutes of exposure.
- Compounding effect: Each exposure without brushing deepens existing discoloration, making subsequent stain removal progressively harder.
Consistent mechanical removal through brushing and flossing disrupts this biofilm before pigments embed permanently, preserving enamel clarity and preventing irreversible dark discoloration from compounding over time.
Coffee Penetrates Unbrushed Surfaces
Coffee’s chromogenic compounds—primarily chlorogenic acids and melanoidins—penetrate enamel surfaces with measurably greater speed and depth when plaque is present.
Plaque absorption accelerates coffee staining by creating a porous, adhesive biofilm that chemically bonds pigments to your tooth surface. Without consistent brushing, you’re fundamentally leaving a stain-trapping layer intact after every cup.
The biofilm’s bacterial proteins interact with coffee’s polyphenols, producing stubborn brown complexes that resist rinsing. Dark foods operate through identical mechanisms—anthocyanins and tannins embed into unbrushed surfaces with comparable efficiency.
You control this outcome directly. Brushing twice daily disrupts the biofilm before pigment bonding becomes permanent. Skipping even one session extends plaque’s exposure window, compounding discoloration progressively.
Mechanical removal remains your most effective intervention against accelerated coffee staining on susceptible enamel.
Can You Actually Reverse Staining From Poor Hygiene?
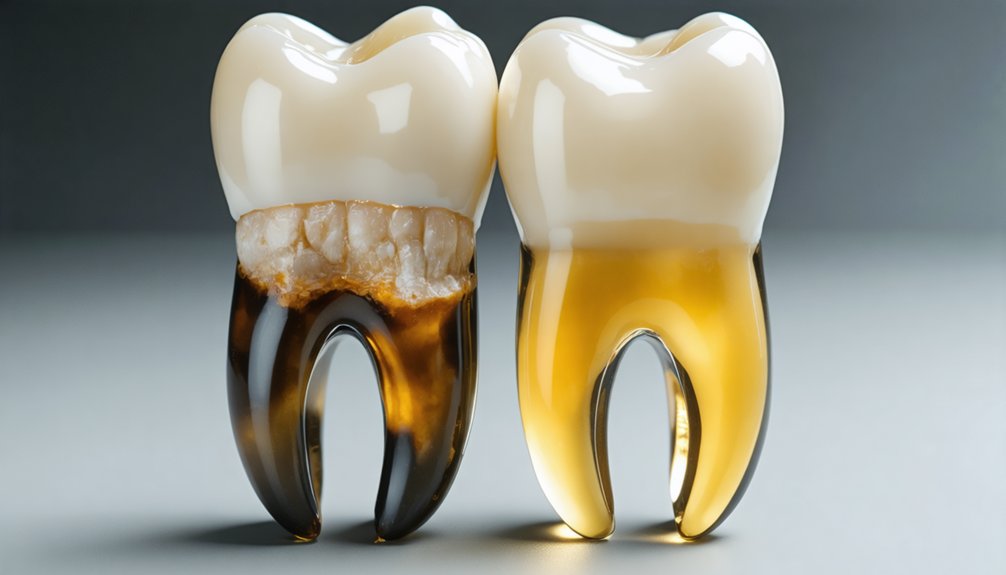
Whether poor hygiene-related staining is reversible depends largely on its type and severity. Extrinsic stains from plaque and food retention respond well to stain reversal through professional cleaning and whitening treatments.
However, intrinsic discoloration from enamel erosion or advanced decay presents a harder clinical challenge.
You can address reversible staining by taking these targeted steps:
- Remove tartar professionally — home care won’t dissolve hardened deposits causing surface discoloration
- Apply whitening treatments — peroxide-based systems effectively lift extrinsic stains post-cleaning
- Restore compromised enamel — fluoride protocols or bonding address erosion-driven yellowing
Decay-induced brown or black discoloration requires restorative intervention, not cosmetic treatment. Your window for reversal narrows as neglect progresses, making early clinical assessment critical to preserving treatment options.
What to Do Every Day to Keep Your Teeth From Staining
Brushing twice daily with fluoride toothpaste and flossing once removes plaque before it hardens into stain-retaining tartar.
You should limit coffee, tea, and other chromogenic beverages, or use a straw to minimize contact with enamel surfaces.
Rinsing with water after meals dislodges food particles and dilutes acids, reducing the likelihood of stain adhesion and enamel erosion.
Brush And Floss Daily
Establishing a consistent oral hygiene routine is the most effective daily defense against tooth discoloration. Mastering proper brushing techniques and understanding flossing importance gives you direct control over plaque accumulation, tartar formation, and stain retention.
Follow these evidence-based daily practices:
- Brush twice daily using fluoride toothpaste and a 45-degree angle technique, targeting the gumline where plaque concentrates most heavily.
- Floss once daily to eliminate interdental plaque that brushing can’t reach, preventing decay-related dark spots and staining between teeth.
- Rinse after staining beverages like coffee or tea, reducing surface contact time before your next brushing session.
Skipping either brushing or flossing allows bacterial plaque to harden into tartar, accelerate enamel erosion, and permanently embed stains into your tooth surfaces.
Limit Staining Beverages
Daily brushing and flossing build your primary defense against discoloration, but what you drink each day works against that effort just as consistently.
Coffee, tea, red wine, and dark sodas contain chromogens and tannins that bind directly to enamel and plaque, accelerating staining beyond what routine oral hygiene can fully reverse. You should limit these staining beverages or consume them through a straw, reducing direct enamel contact.
Rinsing with water immediately after drinking dilutes residual compounds before they adhere. Waiting 30 minutes before brushing post-consumption prevents acid-softened enamel from abrasion.
Frequency matters more than quantity; sipping continuously prolongs acid and pigment exposure. Controlling your beverage habits is a measurable, evidence-supported strategy that directly reduces cumulative staining risk.
Rinse After Eating
Rinsing with water after eating removes residual food particles and dilutes acidic compounds before they interact with enamel or adhere to plaque-covered surfaces.
Effective rinsing disrupts stain retention mechanisms, reducing chromogen adhesion to uncleared plaque. Implementing consistent rinse techniques gives you direct control over discoloration progression between brushing sessions.
Maximize rinsing effectiveness with these targeted practices:
- Swish vigorously for 30 seconds to mechanically dislodge food debris from interproximal spaces and occlusal surfaces.
- Rinse immediately after consuming dark beverages like coffee or tea to prevent chromogen penetration into enamel irregularities.
- Use fluoridated mouthwash periodically to simultaneously neutralize acid and reinforce enamel mineralization against erosion-related yellowing.
You’re not eliminating brushing’s necessity—you’re strategically reducing cumulative stain burden between sessions.
Frequently Asked Questions
Does Genetics Play a Role in How Quickly Teeth Discolor?
Yes, genetic factors influence discoloration speed. Your inherited enamel thickness determines stain resistance—thinner enamel exposes dentin faster. You’re not entirely off the hook, though; poor hygiene accelerates what genetics started.
Are Certain Toothpaste Brands More Effective at Preventing Discoloration?
Yes, certain toothpastes outperform others. You’ll find whitening effectiveness depends on toothpaste ingredients like hydrogen peroxide, fluoride, and silica abrasives, which actively combat plaque, tartar, and stain retention, giving you measurable control over discoloration prevention.
Can Teeth Whitening Treatments Work on Decay-Related Discoloration?
Teeth whitening treatments won’t effectively address decay-related discoloration. You must prioritize decay prevention first, as whitening effectiveness depends on healthy enamel. Treat cavities before pursuing whitening; otherwise, you’ll risk worsening damage and achieving inconsistent, unreliable results.
How Does Dry Mouth Contribute to Faster Teeth Staining?
Dry mouth causes faster staining because you’ve lost saliva’s role in neutralizing acids and washing away pigments. Without adequate saliva, plaque accumulates rapidly, stains adhere more aggressively to enamel, and tartar formation accelerates, intensifying discoloration considerably.
Do Children Experience Poor Hygiene Discoloration Differently Than Adults?
Like a young garden needing early tending, children’s habits shape enamel vulnerability differently—you’ll find early education prevents plaque-driven discoloration, as developing teeth absorb stains faster, making timely hygiene intervention clinically critical for lasting enamel protection.
References
- https://www.regencycourtdentistry.com/blog/causes-of-tooth-discoloration/
- https://my.clevelandclinic.org/health/symptoms/10958-tooth-discoloration
- https://www.maynardfamilydentists.com/what-causes-tooth-discoloration/
- https://www.webmd.com/oral-health/tooth-discoloration
- https://www.opnwide.com/causes-of-tooth-discoloration/
- https://wiltonmanorsdental.com/what-are-the-signs-of-poor-oral-hygiene/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC6937148/
- https://austinlakesdentistry.com/blog/are-discolored-teeth-a-health-concern/