When treating severe fluoride stains, you can’t rely on standard whitening treatments to deliver meaningful results. Professional bleaching targets surface discoloration, but fluorosis involves deep structural enamel defects that peroxide simply can’t reach. Mild-to-moderate cases respond well to microabrasion combined with bleaching, achieving up to 90% stain reduction. Severe fluorosis typically requires porcelain veneers for complete correction. Understanding which treatment matches your severity level is the key to setting realistic expectations and choosing the right solution.
Key Takeaways
- Professional whitening treatments like Zoom are ineffective for severe fluorosis, as they address surface issues rather than deep structural defects.
- Porcelain veneers are the recommended solution for severe fluorosis, lasting 10–20 years and concealing deep stains permanently.
- Microabrasion combined with bleaching achieves 80–90% stain removal for mild fluorosis and 50–70% improvement for moderate cases.
- Sodium hypochlorite (5%) targets organic chromogens unreachable by peroxide, converting brown stains into a more manageable white mottled appearance.
- Severe fluorosis shows minimal response to bleaching, making veneers the only reliable option for complete aesthetic correction.
Why Whitening Alone Fails Severe Fluorosis Cases
Although professional whitening remains a cornerstone of cosmetic dentistry, it consistently falls short for severe fluorosis cases. When you undergo treatment, the dehydration process actually accentuates your stains rather than concealing them, leaving discoloration more prominent post-procedure.
Your treatment expectations must account for this limitation — even Zoom whitening, which uses 40% hydrogen peroxide with light activation, delivers insufficient results for complete stain removal.
Even Zoom whitening — 40% hydrogen peroxide, light activation and all — still falls short against severe fluorosis stains.
Understanding your stain perceptions requires recognizing that severe fluorosis responds at only limited improvement rates without adjunct therapies. Bleaching alone oxidizes surface chromogens but can’t penetrate the deeply mineralized, intrinsic discoloration characteristic of severe cases.
You’re fundamentally targeting a structural enamel defect with a surface-level solution. Whitening works — just not completely here, and knowing that distinction helps you pursue more effective alternatives confidently.
Why Microabrasion Plus Bleaching Works Best for Mild Fluorosis
When you combine microabrasion with professional bleaching, you target mild fluorosis at two levels — the procedure removes the outer enamel layer where superficial stains reside, while bleaching enhances the final color outcome, achieving 80–90% stain removal in favorable cases.
You’ll find that mild-to-moderate cases typically reach 50–70% improvement following this dual approach, making it clinically superior to either treatment alone.
Using carbamide peroxide for the bleaching phase minimizes sensitivity, which matters greatly when treating enamel that’s already structurally compromised by fluorosis.
Microabrasion Removes Surface Stains
Microabrasion strips away the outer layer of enamel where superficial fluorosis stains reside, making it one of the most targeted mechanical interventions available for mild-to-moderate cases.
The procedure uses an acidic abrasive compound to selectively remove discolored enamel without compromising deeper structural integrity. You’ll notice improved surface texture almost immediately, as the treated enamel reflects light more uniformly.
Significantly, the process preserves enamel integrity by targeting only the lesion depth—typically limited to stains that haven’t penetrated beyond superficial layers. For deep staining, success rates drop to 20-40%, making case selection essential.
When you combine microabrasion with professional bleaching afterward, you’re addressing both mechanical discoloration and residual chromogens simultaneously, producing dramatically superior outcomes compared to either treatment applied in isolation.
Bleaching Enhances Final Results
Combining microabrasion with professional bleaching produces 80–90% stain removal in superficial fluorosis cases—a result neither treatment achieves independently.
Microabrasion removes compromised enamel; bleaching addresses residual discoloration beneath. Together, these whitening techniques deliver measurable ΔE >5 improvements for mild-to-moderate stain management.
Why this protocol works:
- Microabrasion eliminates the outer stained layer, allowing bleaching agents deeper enamel penetration.
- Home bleaching with 10% carbamide peroxide worn 2–4 hours daily minimizes sensitivity in enamel-defective teeth.
- Mild-moderate fluorosis achieves 50–70% improvement following combined treatment versus isolated bleaching alone.
- Carbamide peroxide’s gentler oxidation reduces post-treatment sensitivity, supporting patient compliance over 2–6 weeks.
You’re controlling the outcome by selecting a sequenced, evidence-supported approach rather than relying on single-modality treatment.
Minimizing Sensitivity During Treatment
Enamel already compromised by fluorosis responds poorly to aggressive whitening agents, so sequencing microabrasion before bleaching reduces both treatment risk and post-procedural sensitivity.
By removing superficial stained enamel first, you’re allowing lower-concentration bleaching agents to penetrate more efficiently, eliminating the need for harsher peroxide formulations.
Carbamide peroxide—gentler than hydrogen peroxide—delivers measurable sensitivity reduction while maintaining clinical efficacy in enamel-defective teeth.
Pairing microabrasion with 10% carbamide peroxide home bleaching worn 2-4 hours daily optimizes treatment comfort without sacrificing results.
Studies confirm mild-to-moderate fluorosis cases achieve 50-70% improvement through this combined protocol.
You’re controlling both the pace and intensity of treatment, reducing inflammatory responses while systematically improving stain appearance across multiple sessions rather than one aggressive appointment.
Which Whitening Method Matches Your Fluorosis Severity
Matching the right whitening method to your fluorosis severity can mean the difference between meaningful improvement and wasted effort.
Whitening misconceptions often lead patients toward ineffective treatments, so understanding fluorosis severity guides smarter decisions.
Fluorosis misconceptions waste time and money — knowing your severity level is the only path to real results.
- Mild fluorosis — Microabrasion combined with home bleaching (10–20% carbamide peroxide) achieves 60–70% improvement.
- Moderate fluorosis — In-office 40% hydrogen peroxide with microabrasion yields 30–50% stain reduction.
- Severe fluorosis — Bleaching alone won’t deliver results; porcelain veneers lasting 10–20 years provide complete coverage.
- Hypomineralized lesions — 5% sodium hypochlorite followed by resin perfusion oxidizes chromogens bleach can’t reach.
You’re not guessing anymore. Match your severity level to its corresponding protocol, and you’ll avoid wasted treatments and unnecessary disappointment.
Why Severe Fluorosis Needs Veneers, Not Bleaching
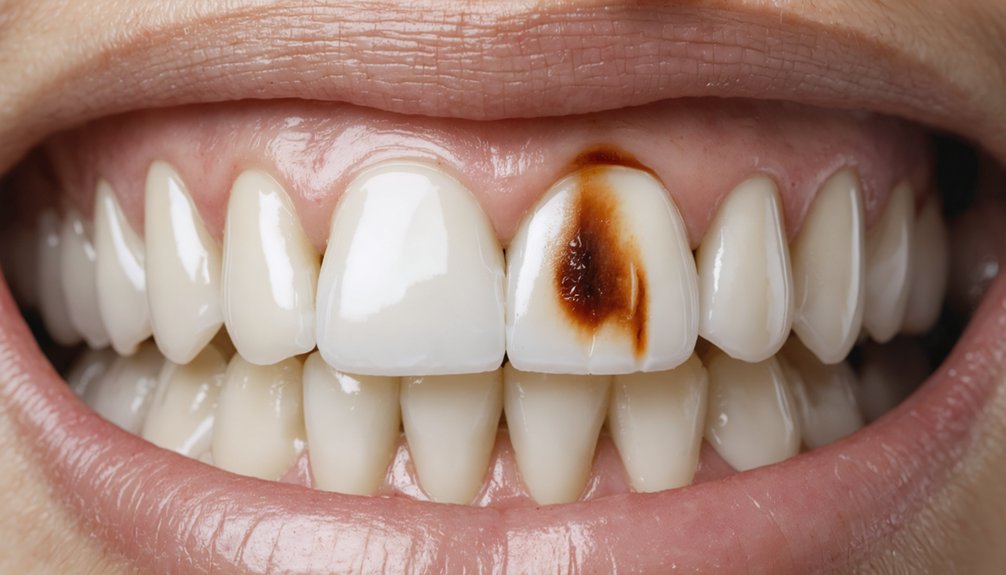
When your fluorosis is severe, bleaching won’t deliver meaningful results—dehydration from the process actually accentuates deep stains, leaving them more prominent than before.
Porcelain veneers, by contrast, physically cover the affected enamel, eliminating discoloration entirely rather than attempting to chemically alter it.
Lasting 10–20 years and resistant to future staining, veneers offer you a clinically reliable, aesthetically superior solution that bleaching simply can’t match at this severity level.
Bleaching Fails Severe Fluorosis
Here’s why bleaching consistently underperforms:
- Dehydration effect — Bleaching accentuates severe staining rather than masking it.
- Penetration limits — Peroxide can’t reverse deep hypomineralization within compromised enamel.
- Incomplete results — Severe cases achieve minimal improvement, even with light-activated Zoom protocols.
- Sensitivity risk — Defective enamel amplifies chemical irritation, limiting treatment duration.
You’re working against enamel that’s structurally altered—not simply discolored.
Bleaching isn’t your solution here.
Veneers Cover Deep Stains
Porcelain veneers resolve what bleaching cannot: deep structural staining embedded within hypomineralized enamel. When fluorosis penetrates beyond the enamel’s surface, whitening agents can’t reach the chromogens causing discoloration. Veneers eliminate that limitation entirely.
Your dentist bonds thin porcelain shells directly over affected teeth, concealing brown and white mottling beneath a uniform, natural-looking surface. This aesthetic transformation requires no repeated treatments or maintenance cycles that bleaching demands.
Veneers longevity spans 10–20 years with proper oral hygiene, making them a durable, cost-effective investment for severe cases.
Unlike composite bonding, porcelain resists future staining and mimics natural enamel translucency precisely. If bleaching has already failed you, veneers don’t compensate—they replace the problem surface completely, giving you permanent control over your smile‘s appearance.
Long-Lasting Veneer Benefits
Severe fluorosis damages enamel structurally, not just superficially—bleaching agents can’t reverse hypomineralization or reach chromogens embedded deep within compromised enamel tissue.
Porcelain veneers deliver complete aesthetic transformation where bleaching fails.
Veneer longevity and clinical performance give you measurable control over your outcome:
- Durability: Porcelain veneers last 10–20 years with proper maintenance.
- Stain resistance: Non-porous porcelain resists future discoloration that compromised enamel cannot.
- Complete coverage: Veneers mask deep brown and white mottling in a single treatment phase.
- Predictability: Unlike bleaching protocols yielding inconsistent ΔE values on severe fluorosis, veneers guarantee uniform color.
You’re not managing a condition—you’re eliminating its visibility permanently.
That’s the clinical and aesthetic distinction veneers provide.
When Sodium Hypochlorite Removes Stains That Peroxide Can’t
When peroxide-based whitening fails to budge fluorosis stains, sodium hypochlorite offers a chemically distinct mechanism that targets what bleaching agents can’t. As one of the most effective alternative whitening agents, 5% sodium hypochlorite applied for 25-30 minutes oxidizes organic chromogens embedded within porous, hypomineralized enamel — material peroxide simply can’t reach.
The sodium hypochlorite benefits extend beyond surface-level action. It extracts deeply embedded pigmentation from structurally compromised enamel, converting unsightly brown staining into a far more manageable white mottled appearance.
Clinicians typically follow this treatment with resin infiltration to reinforce enamel integrity.
If you’ve exhausted peroxide protocols without meaningful results, sodium hypochlorite gives you a targeted, evidence-backed alternative that addresses fluorosis at its chemical source.
What to Expect From Fluorosis Treatment at Each Severity Level
Matching your expectations to fluorosis severity keeps treatment decisions grounded and prevents frustration when results plateau.
Understanding what each fluorosis severity level realistically delivers helps you choose interventions with confidence.
- Mild fluorosis: Microabrasion combined with bleaching achieves 80–90% stain removal; bleaching alone yields 60–70% improvement.
- Moderate fluorosis: Expect 30–50% improvement from whitening; microabrasion plus bleaching raises results to 50–70%.
- Severe fluorosis: Bleaching produces limited outcomes; porcelain veneers lasting 10–20 years offer complete cosmetic correction.
- All severity levels: An initial worsening of appearance is possible before improvement occurs during treatment.
Aligning your treatment expectations with fluorosis severity means you’re selecting protocols based on evidence, not optimism, and you’ll recognize genuine progress when it happens.
Frequently Asked Questions
Can Fluorosis Stains Return After Successful Microabrasion and Bleaching Treatment?
Fluorosis stains won’t typically return after successful fluorosis treatment, but microabrasion effectiveness depends on stain depth. You’ll need to maintain good oral hygiene and avoid staining agents to preserve your 80-90% improvement long-term.
Are At-Home Whitening Kits Safe for Children With Fluorosis Stains?
At-home safety is absolutely everything here—you shouldn’t use whitening kits on children with fluorosis without consulting a dentist first, as fluoride exposure compounds enamel sensitivity, and carbamide peroxide formulas risk irreversible damage to developing dentition.
Does Dental Insurance Typically Cover Veneers for Severe Fluorosis Cases?
Most insurers don’t cover veneers cost since they’re deemed cosmetic, not medically necessary. You’ll need to explore financing or alternative treatment options, as porcelain veneers remain your most effective solution for severe fluorosis cases.
How Long Does Sodium Hypochlorite Treatment Take During a Dental Visit?
Like paint stripper dissolving layers, sodium hypochlorite effectiveness peaks when you allow it 25-30 minutes of contact time during your visit—that’s your treatment duration for oxidizing stubborn chromogens from porous enamel.
Can Fluorosis Staining Worsen With Age if Left Completely Untreated?
Yes, fluorosis progression can worsen as aging effects accumulate—you’ll notice stains darkening and enamel weakening over time. Without treatment, you’re allowing irreversible discoloration to deepen, making future aesthetic interventions increasingly complex and less effective.
References
- https://www.magnoliadentistry.com/blog/dental-fluorosis-treatment-from-stains-to-sparkle/
- https://drbvreddysdental.com/what-are-the-best-treatment-options-for-fluorosis-affected-teeth/
- https://www.ritchiedentalgroup.com/blog/expert-dentist-in-marble-falls/
- https://softouchdentalcare.com/blog/can-zoom-teeth-whitening-treat-fluorosis/
- https://teethwhiteninghochiminh.com/best-fluorosis-teeth-whitening/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC12170373/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC4606706/
- https://custmbite.com/pages/teeth-whitening-for-fluorosis
- https://www.ada.org/resources/ada-library/oral-health-topics/whitening