Long-term teeth whitening treatments can permanently damage your enamel, increase tooth sensitivity, and harm your gum tissue. Repeated peroxide applications strip protective minerals, thin your enamel, and expose the underlying dentin, making your teeth more vulnerable to fractures and nerve irritation. Without adequate recovery time between sessions, your saliva can’t remineralize your enamel effectively. Understanding exactly how these compounding effects unfold can help you make safer, more informed decisions about your whitening choices.
Key Takeaways
- Repeated peroxide applications strip protective minerals from enamel, leaving teeth thinner, weaker, and increasingly vulnerable to fractures over time.
- Peroxide penetrates enamel and irritates dental nerves, causing heightened sensitivity to hot, cold, and pressure with prolonged use.
- Prolonged bleaching thins enamel, exposing yellow dentin underneath and creating cosmetic damage that is difficult to reverse.
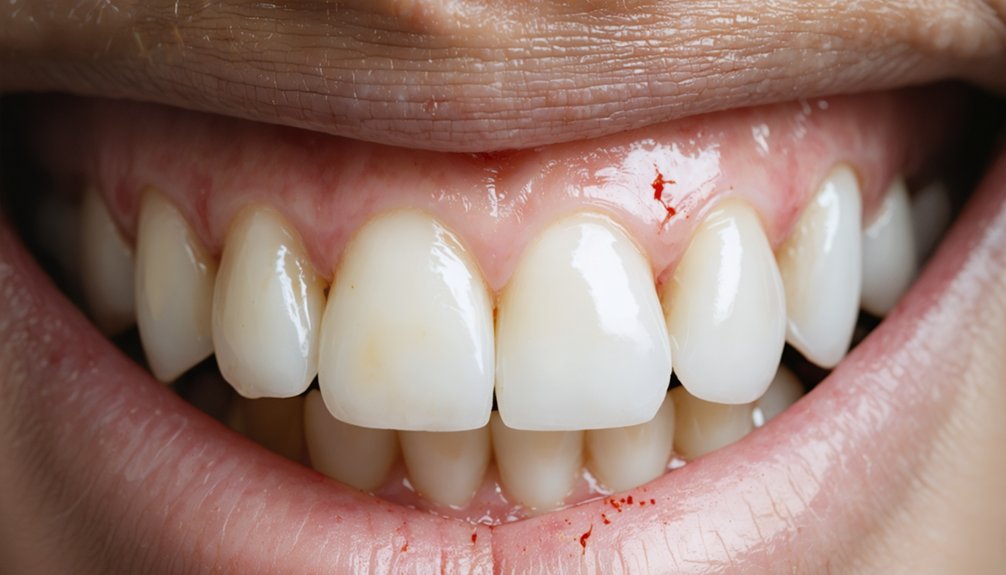
- Frequent contact with whitening agents can chemically burn gum tissue, causing recession, swelling, and chronic irritation.
- High-concentration DIY treatments without professional oversight significantly increase risks of pulp damage, enamel erosion, and nerve injury.
How Repeated Whitening Treatments Destroy Your Enamel Over Time
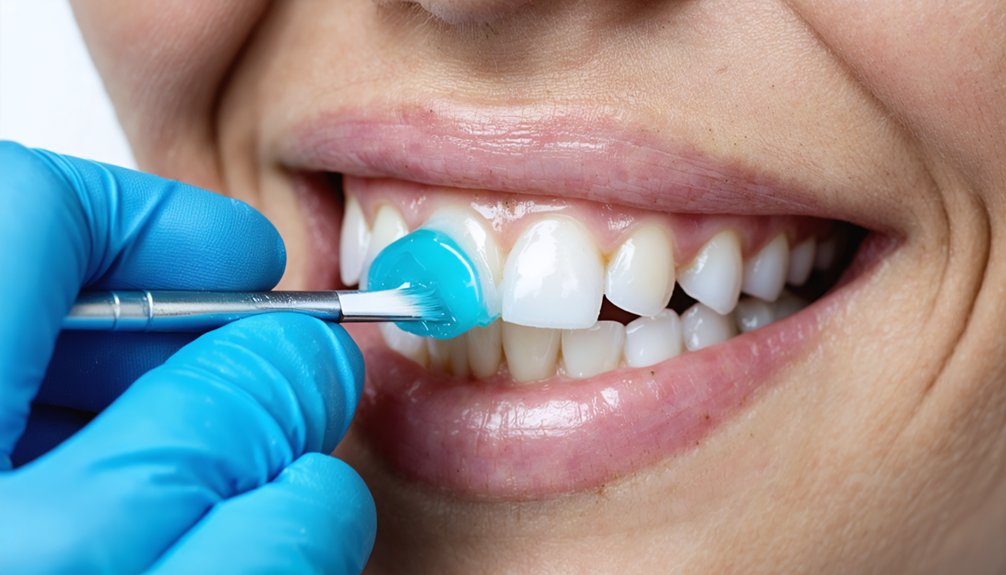
While teeth whitening products promise a brighter smile, repeated use gradually destroys the very structure that protects your teeth. Each peroxide application strips protective minerals, compromising enamel health and exposing the sensitive dentin beneath.
The American Dental Association confirms that aggressive bleaching causes microstructural erosion that your saliva can’t reverse without adequate recovery periods.
You’re accelerating permanent damage when whitening frequency exceeds safe thresholds. Without sufficient breaks between sessions, remineralization can’t occur, leaving your enamel progressively thinner and your teeth vulnerable to fractures and cavities.
Taking control means seeking professional guidance before continuing any whitening regimen. Dentists can assess your enamel’s current condition, establish safe treatment intervals, and recommend evidence-based treatment alternatives that achieve your desired results without systematically dismantling your teeth’s natural defense.
Why Each Whitening Session Makes Tooth Sensitivity Worse
Each whitening session compounds sensitivity because peroxide penetrates enamel and irritates the nerves within your teeth.
Without adequate enamel recovery time between treatments, you’re continuously exposing dentin and pulp to chemical stress. This cumulative exposure intensifies sensitivity triggers, making hot, cold, and pressure stimuli increasingly painful.
Laboratory studies confirm that aggressive or frequent bleaching prevents salivary remineralization, the natural process your teeth rely on to rebuild protective mineral layers.
Once dentin becomes exposed, nerve responses sharpen markedly. If you have existing cracks, cavities, or worn enamel, peroxide penetrates deeper, accelerating nerve irritation.
You control the outcome by spacing treatments appropriately and allowing full enamel recovery between sessions.
Ignoring these intervals doesn’t accelerate results—it permanently worsens sensitivity and compromises your long-term dental health.
The Gum Damage Whitening Brands Hide From You
Whitening brands rarely disclose that their products can burn, inflame, and chemically damage your gum tissue with repeated use.
Prioritizing consumer awareness means understanding what labels omit about chemical safety.
Three documented gum risks include:
- Chemical burns and recession from prolonged bleaching agent contact
- Swelling and redness caused by ill-fitting trays that leak gel onto tissue
- Chronic irritation from DIY treatments applied without professional guidance
Protecting your gum health requires informed choices, not marketing trust.
Brands prioritize sales over product transparency, leaving you vulnerable to preventable damage.
Whitening alternatives like professional-supervised treatments offer enamel protection while minimizing tissue exposure.
Seek professional guidance before continuing any whitening regimen—your gums don’t regenerate tissue lost to chemical overexposure, making prevention your only reliable strategy.
Warning Signs Your Teeth Are Being Permanently Damaged by Whitening
Recognizing early warning signs of whitening-induced damage can prevent irreversible structural harm to your teeth. Monitor these sensitivity signs closely: sharp pain from hot or cold stimuli indicates exposed dentin, while persistent aching between sessions suggests nerve irritation.
Translucent edges or a bluish tint at tooth tips are critical enamel warnings signaling severe mineral loss. If your gums appear recessed, swollen, or discolored after treatments, chemical burns may have already occurred.
Uneven coloration across natural teeth and restorations confirms structural compromise. Increased sensitivity that doesn’t resolve within 48 hours post-treatment requires immediate professional evaluation.
Continuing whitening while experiencing these symptoms accelerates permanent damage, including pulp inflammation and enamel fractures. Stop treatment and consult a dentist before proceeding further.
How Whitening Chemicals Reach Your Nerves and What Happens Next
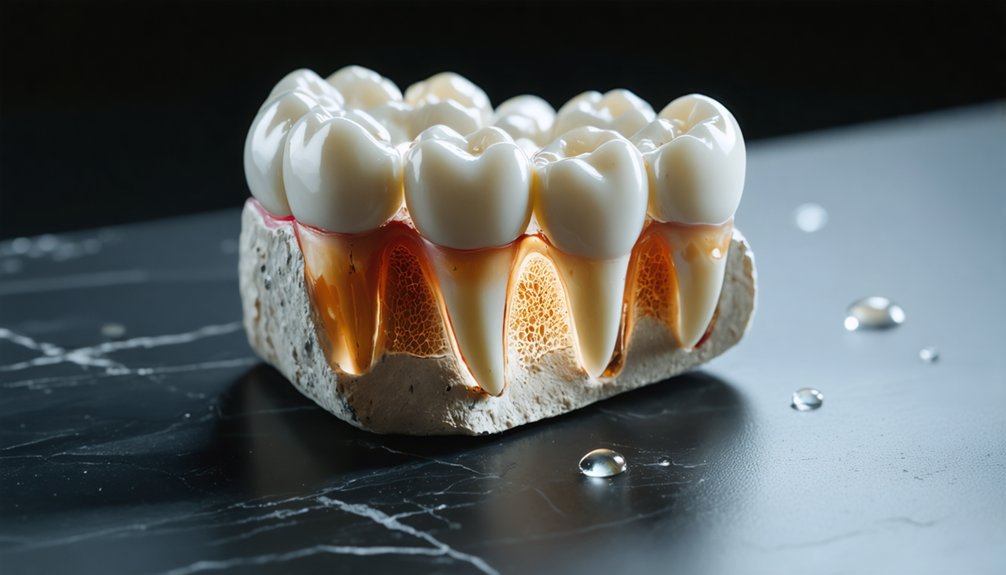
When you apply peroxide-based whitening agents, the chemicals penetrate your enamel and reach the dentin tubules, creating a direct pathway to the pulp where your nerves reside.
If you have pre-existing cracks, cavities, or worn enamel, this penetration accelerates, irritating nerve tissue and triggering sharp sensitivity or persistent pain.
Repeated exposure without adequate recovery periods prevents your nerves from stabilizing, increasing your risk of long-term pulp damage that may require clinical intervention.
Chemical Penetration Into Enamel
Here’s what actually happens during penetration:
- Peroxide molecules pass through enamel’s crystalline structure, reducing enamel integrity and accelerating nerve exposure at the pulp boundary.
- Product formulation concentration determines penetration speed—higher percentages breach deeper layers faster.
- Without following established safety guidelines, you eliminate any opportunity for enamel restoration through natural remineralization.
Sensitivity management becomes critical because chemical exposure isn’t reversible once dentin tubules open.
You’re not just whitening—you’re chemically altering living tooth architecture with every unsupervised application.
Nerve Irritation Explained
Once peroxide breaches your enamel, it doesn’t stop—it continues migrating inward through dentin tubules until it reaches the pulp chamber, where your tooth’s nerve supply lives.
When this happens, inflammation follows, compromising nerve health and triggering sharp sensitivity responses.
Whitening frequency directly determines your risk level. Frequent sessions prevent enamel restoration between treatments, leaving tubules persistently open and nerves chronically exposed.
Without adequate recovery time, nerve exposure escalates from temporary irritation to lasting pulpal damage.
Maintaining treatment balance is essential for whitening safety. Sensitivity management strategies—including fluoride application and extended intervals between sessions—help protect nerve integrity.
Dental monitoring allows professionals to assess pulpal responses before damage becomes irreversible.
Skipping professional oversight removes your most reliable safeguard against progressive, compounding nerve injury.
Long-Term Nerve Consequences
Acute nerve irritation from whitening chemicals is troubling enough, but the more serious concern is what happens when that irritation isn’t given time to resolve.
Repeated chemical exposure compromises nerve regeneration, leaving pulp tissue increasingly vulnerable with each session.
Long-term consequences you risk include:
- Persistent hypersensitivity — nerves remain in a heightened state, responding painfully to temperature and pressure long after treatment stops.
- Pulp inflammation — chronic irritation progresses toward irreversible pulpitis, potentially requiring root canal intervention.
- Nerve death — prolonged chemical assault can permanently destroy pulp tissue, ending nerve regeneration entirely.
Your dental health depends on recognizing these outcomes before they become irreversible.
Frequency, concentration, and recovery time aren’t optional variables — they’re the factors that determine whether damage stays temporary or becomes permanent.
Why Long-Term Whitening Leaves Teeth Patchy and Translucent
When you whiten your teeth repeatedly over time, you risk developing uneven results because fillings, crowns, and veneers don’t respond to bleaching agents the way natural enamel does.
Your teeth also vary in calcium content and structural density, causing them to absorb whitening chemicals at different rates and producing a patchy appearance.
Prolonged peroxide exposure eventually thins your enamel to the point of translucency, revealing the yellow dentin beneath and creating a cosmetic outcome that’s difficult to reverse.
Uneven Whitening Results
Many people assume that the longer they whiten, the more uniform their results will be—but long-term whitening frequently produces the opposite effect.
Over time, uneven shades and patchy results become increasingly visible due to several factors:
- Restorations don’t respond — Fillings, crowns, and veneers resist peroxide entirely, creating stark color mismatches against your natural teeth.
- Structural differences matter — Calcium content and enamel density vary across teeth, causing uneven absorption of whitening agents.
- Enamel thinning creates translucency — Excessive bleaching erodes enamel, making teeth appear bluish or transparent rather than white.
You can’t correct these outcomes simply by whitening more.
Without strategic breaks and professional oversight, you’re compounding inconsistency—not resolving it.
Translucency From Overuse
Uneven whitening results are only part of the problem—extended bleaching also alters the physical structure of enamel in ways that produce a distinctly different and harder-to-reverse cosmetic outcome: translucency.
When you repeatedly expose enamel to peroxide, you increase enamel permeability, stripping the mineral density that gives teeth their natural, opaque appearance.
The result is translucent teeth—edges that appear grayish, glassy, or nearly see-through, particularly at the incisal tips.
This occurs because thinned enamel allows the underlying dentin’s yellow tone to show inconsistently, while heavily bleached areas lose enough structure to transmit light rather than reflect it.
Unlike surface staining, this structural change doesn’t respond to further whitening.
It requires restorative intervention, making overuse a clinically significant and costly mistake you’ll want to avoid.
The Whitening Methods Most Likely to Cause Permanent Damage
Not all whitening methods carry equal risk, and some are far more likely to cause permanent damage than others. Understanding which whitening techniques compromise enamel protection and gum health helps you make informed decisions.
The three highest-risk methods include:
- High-concentration OTC gels — Ill-fitting trays increase contact time, undermining sensitivity management and accelerating enamel erosion.
- Unsupervised professional-strength treatments — Without dental monitoring, product ingredients penetrate vulnerable pulp tissue, risking nerve damage.
- Frequent DIY charcoal or acid-based products — Abrasive compounds strip enamel faster than restorative treatments can address.
Patient education and professional advice remain your strongest defenses.
Cosmetic dentistry offers supervised protocols that balance whitening outcomes against measurable biological risk.
Don’t let trend-driven choices override evidence-based judgment.
How to Reduce Long-Term Damage If You Choose to Whiten

Although whitening carries inherent risks, you can take deliberate steps to minimize long-term damage to your enamel, gums, and nerve tissue. Whitening moderation is your strongest protective strategy — limit treatments to dentist-recommended intervals and avoid consecutive sessions without recovery periods. This allows salivary remineralization to restore protective minerals before your next exposure.
Prioritize enamel care by using low-concentration peroxide formulas and fluoride-based toothpaste between treatments. Confirm trays fit properly to prevent gel contact with gum tissue. Avoid whitening over existing restorations, cracks, or cavities, as chemical penetration heightens nerve and pulp risk.
Schedule dental evaluations before and after whitening cycles. Professional oversight lets you identify early erosion or sensitivity patterns before they become permanent, keeping your whitening approach controlled and evidence-informed.
Frequently Asked Questions
Can Teeth Whitening Treatments Interact Negatively With Existing Dental Medications?
Yes, they absolutely can devastate your oral health! Whitening agents may intensify sensitivity issues and accelerate enamel erosion when combined with certain dental medications, so you’ll want to consult your dentist before proceeding.
Are Children and Teenagers at Higher Risk From Whitening Treatments Than Adults?
Yes, you face greater risks if you’re young—youth sensitivity and incomplete enamel development make teeth more vulnerable to chemical damage, increasing nerve irritation, erosion, and lasting structural harm compared to fully developed adult dentition.
Does Diet Affect How Quickly Whitening Damage Progresses Over Time?
Like acid rain eroding stone, acidic foods accelerate whitening damage considerably. Your dietary impact on enamel sensitivity compounds peroxide exposure — you’re weakening tooth structure faster when you consume citrus, soda, or coffee alongside frequent whitening treatments.
Can Teeth Ever Fully Recover After Years of Repeated Whitening Treatments?
Your teeth can’t fully recover after years of repeated whitening. Enamel erosion is permanent, as lost minerals don’t regenerate. You’ll likely experience lasting teeth sensitivity, since damaged enamel and exposed dentin don’t restore themselves without professional intervention.
Are Certain Blood or Health Conditions Worsened by Whitening Chemical Exposure?
Certain conditions can complicate chemical sensitivity during whitening. If you’ve got bleeding disorders, autoimmune issues, or compromised oral health, peroxide penetration potentially provokes pronounced systemic reactions—always consult your physician before proceeding with any whitening treatment.
References
- https://www.caryprosthodontics.com/teeth-whitening/teeth-whitening-risks-and-side-effects/
- https://www.blvddentistry.com/effect-of-teeth-whitening-too-often/
- https://www.cornerstonedentistryvan.com/the-hidden-dangers-of-teeth-whitening-treatments/
- https://adanews.ada.org/huddles/risks-of-frequent-teeth-whitening/
- https://www.dentistryofwestbend.com/teeth-whitening-risks-and-side-effects/
- https://www.giodentalsl.com/are-teeth-whitening-treatments-causing-long-term-side-effects/
- https://health.clevelandclinic.org/is-teeth-whitening-safe
- https://gratondentalgroupca.com/dangers-of-over-whitening-your-teeth-and-how-to-avoid-it/