When you whiten your teeth with dry mouth, you’ll face three serious risks. First, you’ll experience intensified tooth sensitivity as whitening agents penetrate deeper without saliva’s protective buffering. Second, your gums become vulnerable to chemical irritation and potential burns since saliva can’t neutralize the peroxide effectively. Third, your enamel’s remineralization process slows dramatically, leaving your teeth structurally weakened for extended periods. Understanding these mechanisms and implementing protective strategies can help you minimize damage while achieving your desired results.
Key Takeaways
- Whitening agents penetrate exposed dentin without saliva’s protection, causing increased tooth sensitivity and prolonged demineralization.
- Peroxide remains on gum tissue longer without saliva’s buffering, leading to inflammation, redness, and potential chemical burns.
- Enamel remineralization slows significantly when saliva cannot restore minerals, leaving teeth vulnerable to erosion and structural damage.
- Reduced saliva extends peroxide contact time on teeth, increasing penetration depth through enamel and exposed dentin tubules.
- Whitening effectiveness decreases without saliva’s chemical activation, potentially requiring stronger peroxide concentrations or longer treatment duration.
Increased Tooth Sensitivity From Reduced Saliva Protection
When you undergo teeth whitening with insufficient saliva production, your teeth lose their primary defense mechanism against chemical stress. Saliva maintains a neutral pH environment and delivers protective proteins that counteract whitening agent penetration into dental structures. Without adequate salivary flow, hydrogen peroxide and carbamide peroxide remain in prolonged contact with tooth surfaces, accelerating the enamel demineralization process and creating pathways to sensitive dentin layers.
Your compromised remineralization capacity prevents normal mineral restoration after bleaching exposure. This extended chemical contact increases demineralization depth and exposes dentin tubules, allowing direct peroxide access to nerve-rich areas. While approximately 50% of whitening patients experience sensitivity under normal conditions, dry mouth substantially elevates this risk. Higher peroxide concentrations further compound the problem, particularly when your natural salivary protection is absent during treatment sessions.
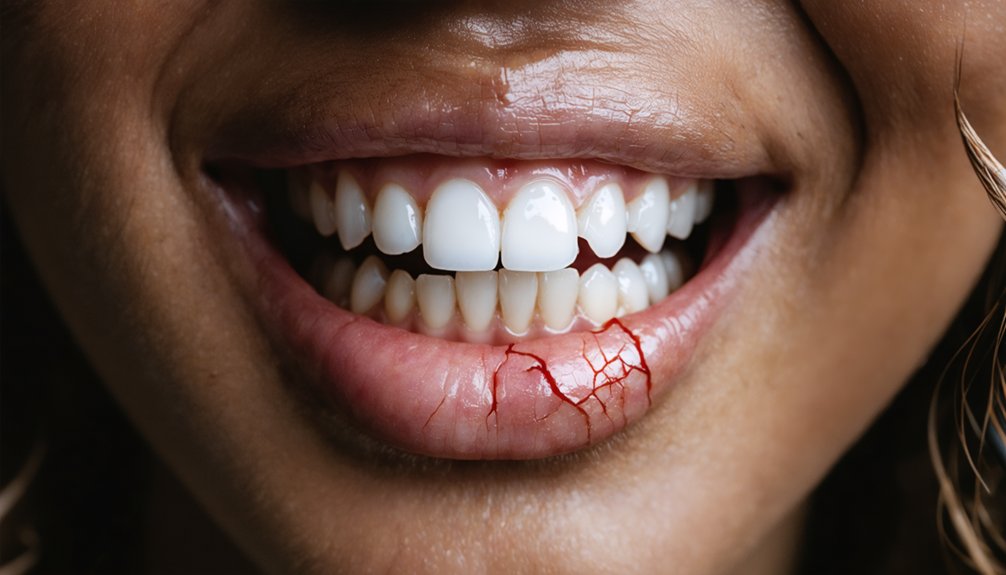
Heightened Gum Irritation Due To Inadequate Chemical Buffering
Because saliva acts as your gums’ primary chemical buffer, its absence during teeth whitening leaves soft tissues vulnerable to direct peroxide damage. Without adequate salivary flow, hydrogen peroxide and carbamide peroxide penetrate gingival tissues unchecked, creating oxidizing effects that trigger localized inflammation severity you can’t ignore. You’ll notice tissue damage patterns progressing from initial redness and swelling to white patches indicating chemical burns—symptoms that develop within 24 hours of treatment.
Poorly-fitted trays worsen this exposure, allowing gel seepage directly onto unprotected gums. The oxidative stress accumulates between applications since saliva can’t dilute or neutralize these compounds. You’re facing extended chemical contact duration, burning sensations, and potential bleeding that signals severe irritation requiring immediate treatment cessation and professional evaluation.
Delayed Enamel Remineralization Caused By Saliva Deficiency
Your teeth depend on saliva’s mineral-rich composition to rebuild enamel structure after whitening treatments temporarily weaken it. When you have dry mouth, you’re facing continued mineral depletion because deficient salivary flow reduces the calcium and phosphate ions necessary for restoration.
This creates a problematic cycle: whitening procedures make enamel porous for 24 to 48 hours, while your compromised saliva can’t deliver adequate minerals during this critical recovery window. The temporary enamel vulnerability becomes prolonged when your mouth lacks the buffering capacity to neutralize acid attacks and restore lost minerals.
Without sufficient saliva, remineralization operates slower than demineralization, allowing erosion to advance. You’ll need supplemental fluoride treatments, calcium phosphate pastes, or hydroxyapatite-based products to compensate for your saliva’s reduced protective function.
Frequently Asked Questions
Can Dry Mouth Cause Uneven Whitening Results During Teeth Bleaching Treatments?
Like a telegraph disrupting messages, dry mouth impairs saliva production impact, preventing even whitening agent distribution across your enamel. You’ll experience patchy results and heightened enamel sensitivity concerns. Hydrate strategically and maintain rigorous oral hygiene to control outcomes effectively.
Does Dry Mouth Increase the Risk of Chemical Burns From Whitening Gels?
Yes, dry mouth increases your risk of chemical burns from whitening gels. Reduced saliva can’t adequately buffer peroxide agents, leading to increased sensitivity and dental irritation. You’ll experience heightened vulnerability to tissue damage without proper moisture protection.
Are Over-The-Counter Whitening Products Safer for People With Dry Mouth Conditions?
Not necessarily—over-the-counter products still pose risks for your dry mouth condition. You’ll minimize sensitivity risks by choosing ideal whitening timing under professional supervision, where customized concentrations and application methods protect your compromised oral tissues more effectively.
Should I Hydrate Before Whitening Treatments if I Have Chronic Dry Mouth?
Yes, you should hydrate before whitening treatments. Pre-treatment hydration temporarily boosts increased saliva production, which dilutes bleaching agents and addresses dental irritation concerns. This protective step minimizes gel concentration on your gums and reduces sensitivity risks effectively.
Can Dry Mouth Worsen Bleachorexia or Obsessive Whitening Behaviors?
Yes, dry mouth can worsen bleachorexia. Studies show 40% of frequent whiteners report compulsive behaviors. Your reduced saliva fails to buffer agents, causing increased dental sensitivity and heightened gum irritation—prompting you to over-whiten despite worsening damage.