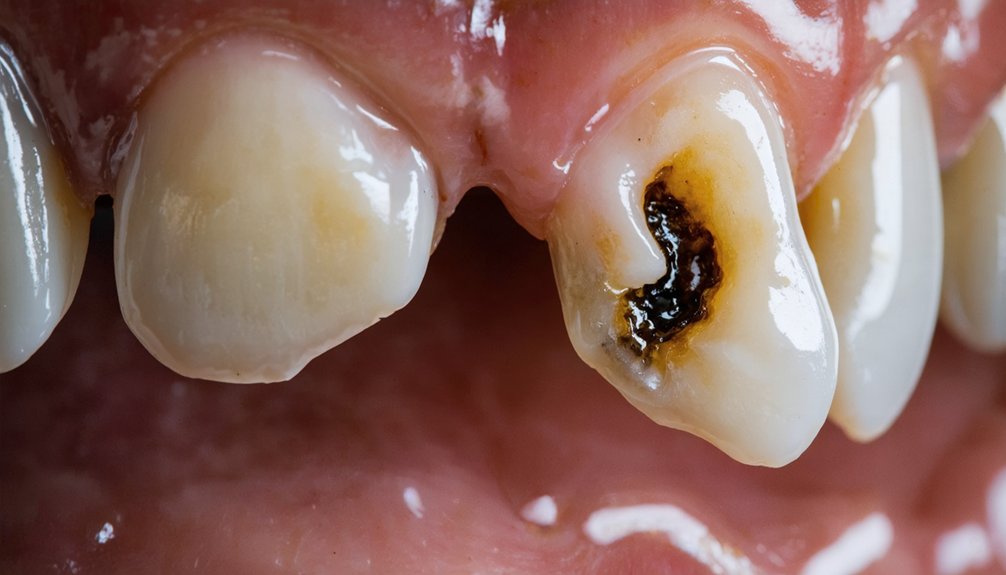
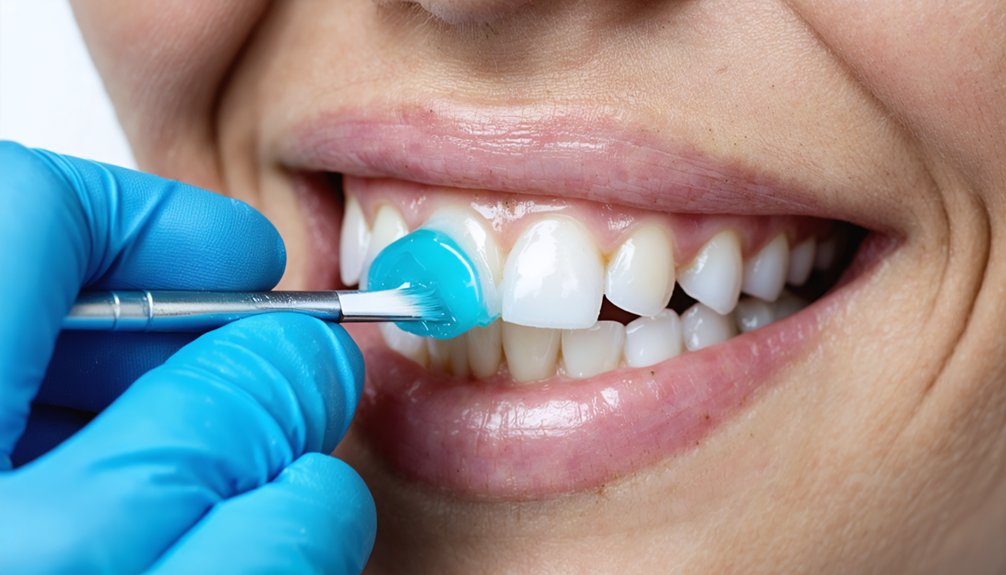
Whitening your teeth over untreated cavities puts your dental health at serious risk. Peroxide-based chemicals can penetrate compromised enamel, reach exposed dentin, and contact nerve tissue, causing acute pain and potential irreversible nerve damage. They can also accelerate existing decay and chemically irritate your gum tissue. You’ll likely experience heightened sensitivity that outlasts the treatment itself. Understanding each specific risk can help you make a safer, more informed decision before proceeding.
Key Takeaways
- Whitening agents penetrate compromised enamel, reaching the pulp chamber and potentially causing nerve damage in teeth with untreated cavities.
- Peroxide-based whitening products can worsen existing decay, deepen cavity openings, and mask progression, delaying necessary dental treatment.
- Cavities expose dentin tubules, amplifying sensitivity and triggering sharp, persistent pain during and after whitening treatment.
- Severe nerve damage from whitening over cavities may require emergency procedures, including root canal therapy or tooth extraction.
- Whitening agents can chemically burn gum tissue, with existing gum disease alongside cavities intensifying the inflammatory response.
What Happens to Your Teeth When You Whiten Over Cavities
When you whiten teeth that have untreated cavities, bleaching agents containing hydrogen peroxide penetrate the compromised enamel and seep directly into the pulp chamber, where nerve endings are located. This direct chemical contact triggers sharp pain and risks irreversible nerve damage.
Cavities extending beyond enamel into the dentin layer greatly increase this danger, regardless of which whitening techniques you use.
Without prioritizing dental safety first, you’re also accelerating existing decay. Whitening agents aggravate damaged enamel, widen cavity areas, and mask decay progression—delaying treatment you actually need.
Severe nerve damage may ultimately require root canal therapy or tooth extraction.
The temporary cosmetic result isn’t worth permanent structural damage. Address active cavities with your dentist before pursuing any whitening treatment.
Should You Fill Cavities Before Whitening Your Teeth?
Filling cavities before whitening your teeth isn’t just recommended—it’s crucial for protecting your dental health. One of the most common whitening misconceptions is that cosmetic treatments can proceed safely despite untreated decay. They cannot.
Active cavities expose dentin tubules and pulp chambers to peroxide-based agents, increasing your risk of nerve damage, prolonged sensitivity, and accelerated decay progression.
Peroxide agents penetrate active cavities, reaching nerves and accelerating decay—transforming a cosmetic treatment into a dental emergency.
Prioritizing dental safety means addressing all cavities first, then whitening. This sequencing also guarantees your future restorations match your final whitened shade—preventing costly color mismatches later.
Whitening over untreated cavities doesn’t mask the problem; it worsens it while delaying necessary treatment.
Before starting any whitening protocol, schedule a thorough dental exam. You control the outcome by making informed, clinically sound decisions before cosmetic procedures begin.
Can Teeth Whitening Damage Your Tooth Nerves?
When you have cavities, hydrogen peroxide in whitening agents can penetrate your compromised enamel and reach the sensitive inner layers of your tooth.
The deeper your cavity extends toward the pulp chamber, the greater your risk of direct chemical contact with your nerve endings, triggering acute pain and potential irreversible nerve damage.
In severe cases, this damage can’t be undone, leaving root canal treatment or extraction as your only remaining options.
Peroxide Penetrating Compromised Enamel
Healthy enamel acts as a protective barrier, but cavities compromise its structural integrity and create pathways for bleaching agents to penetrate deeper into the tooth.
Weakened tooth enamel accelerates peroxide absorption, exposing vulnerable inner layers to chemical damage.
Key risks of peroxide penetrating compromised enamel include:
- Dentin exposure — Peroxide bypasses damaged enamel, reaching dentin tubules and triggering acute sensitivity and pain.
- Pulp chamber infiltration — Bleaching agents traveling through cavity openings contact nerve endings directly, risking irreversible nerve damage.
- Accelerated structural breakdown — Hydrogen peroxide weakens already-compromised enamel further, expanding cavity margins and deepening decay.
Understanding these mechanisms gives you the information needed to make an informed decision before pursuing whitening treatments on teeth with untreated cavities.
Cavity Depth And Nerve Exposure
The deeper a cavity extends into your tooth, the greater the risk that whitening agents will reach your nerve tissue.
Dentists use cavity classification systems to assess decay progression through enamel, dentin, and toward the pulp. Once decay breaches dentin, nerve exposure becomes a serious concern during whitening treatment.
When peroxide-based agents contact an advancing cavity, they can penetrate directly into the pulp chamber, triggering acute pain and potentially irreversible nerve damage.
You may require root canal therapy or extraction if this damage becomes permanent. Cavities classified at deeper stages markedly amplify this risk compared to surface-level decay.
Before pursuing any whitening procedure, you should confirm through professional examination that no active decay threatens nerve exposure during chemical treatment.
Irreversible Nerve Damage Risks
Irreversible nerve damage represents one of the most serious consequences you can face when whitening teeth affected by active decay.
When peroxide-based whitening techniques penetrate compromised enamel, they reach the pulp chamber directly, triggering acute nerve responses that may become permanent.
Protecting your nerve health requires understanding what’s at stake:
- Pulp exposure — Hydrogen peroxide contacts nerve endings through cavity openings, causing immediate, severe pain and potential irreversible tissue destruction.
- Progressive damage — Repeated whitening sessions compound nerve trauma, increasing the likelihood that damage becomes permanent rather than temporary.
- Irreversible outcomes — Severe nerve compromise may require root canal treatment or extraction to resolve.
Addressing cavities before pursuing any whitening techniques is non-negotiable for preserving long-term nerve health.
How Whitening Chemicals Accelerate Cavity Damage
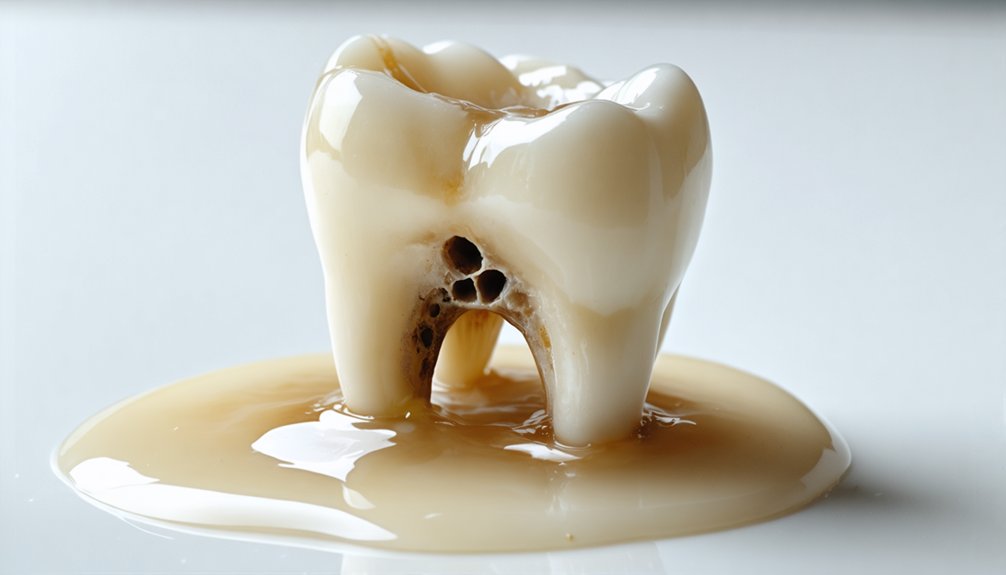
When you apply whitening products to teeth with active cavities, you’re not just risking sensitivity—you’re actively accelerating decay.
Bleaching agents penetrate compromised enamel, chemically aggravating damaged tooth structure and widening existing cavity areas.
This combination of whitening chemicals and active decay breaks down your tooth faster than decay alone, often requiring more extensive treatment than if you’d addressed the cavity first.
Bleaching Agents Worsen Decay
Many people assume teeth whitening simply brightens their smile, but bleaching agents actively worsen existing tooth decay rather than leaving it undisturbed.
When you apply peroxide-based products to compromised teeth, you’re accelerating cavity progression and intensifying enamel erosion beyond its current state.
Bleaching chemicals create three measurable dangers for decayed teeth:
- Structural breakdown – Peroxide penetrates weakened enamel, widening and deepening existing cavity areas.
- Decay masking – Temporary whitening effects conceal active deterioration, delaying necessary treatment.
- Accelerated damage – Combining whitening chemicals with active decay speeds tooth structure breakdown considerably.
You won’t reverse damage by whitening over it.
Address cavities before pursuing cosmetic treatment to maintain control over both your dental health and your whitening outcomes.
Enamel Breakdown Accelerates
Hydrogen peroxide doesn’t simply bleach surface stains—it actively penetrates compromised enamel and chemically disrupts the weakened mineral structure surrounding existing cavities.
When you apply whitening agents to decayed teeth, the peroxide accelerates enamel erosion by breaking down already-fragile mineral bonds. Your enamel loses its protective integrity faster than it would through normal decay progression alone.
The whitening effects you’re chasing come at a structural cost. Bleaching chemicals widen microscopic fissures within cavity margins, creating larger pathways for bacteria and acids to penetrate deeper into your tooth.
What began as a manageable cavity can rapidly advance into dentin exposure requiring more invasive treatment. You’re not just whitening—you’re actively compromising your tooth’s remaining structural defense when untreated decay is present.
Chemicals Deepen Cavity Damage
Beyond structural weakening, whitening chemicals don’t just passively occupy the spaces that decay creates—they actively worsen the damage already present.
These chemical interactions accelerate breakdown in already-compromised enamel integrity, turning a manageable cavity into a more serious dental problem.
Here’s what’s happening inside your tooth:
- Bleaching agents widen existing cavity openings, allowing deeper peroxide penetration into dentin and pulp tissue.
- Whitening chemicals aggravate active decay, accelerating the breakdown of surrounding tooth structure rather than halting it.
- Decay progression becomes masked by surface-level whitening results, delaying the treatment you actually need.
You’re not just whitening a damaged tooth—you’re introducing reactive chemicals into an already unstable environment, compounding the damage with every application.
Why Cavities Make Whitening Sensitivity So Much Worse
When cavities compromise enamel integrity, they expose dentin tubules directly to whitening agents, dramatically amplifying the sensitivity response beyond what healthy teeth experience.
The cavity impact on your nerve endings is immediate — peroxide penetrates these open pathways, triggering sharp, prolonged pain that healthy enamel would otherwise block.
Your sensitivity levels won’t just spike during treatment; they’ll persist long after you’ve finished whitening.
Hot, cold, and sweet foods become sources of significant discomfort, sometimes requiring professional intervention to manage effectively.
Even standard over-the-counter products deliver enough chemical contact to cause severe reactions when cavities are present.
You’re not experiencing ordinary post-whitening sensitivity — you’re experiencing chemical exposure to compromised dental tissue.
Addressing cavities before whitening gives you direct control over preventing this avoidable outcome.
How Long Does Tooth Pain Last After Whitening With Cavities?
Pain duration after whitening with cavities isn’t predictable — it depends on how deep your cavities are, how close they sit to the nerve, and what concentration of whitening chemicals made contact with compromised tissue.
Toothache duration varies greatly based on damage severity:
- Mild cases — Sensitivity resolves within 24–48 hours with basic pain management strategies like desensitizing toothpaste.
- Moderate cases — Pain persists several days, requiring professional evaluation to rule out nerve involvement.
- Severe cases — Prolonged toothaches signal potential irreversible nerve damage, possibly requiring root canal treatment or extraction.
Don’t underestimate persistent pain as temporary discomfort.
If your pain extends beyond 48 hours post-whitening, contact your dentist immediately.
Delayed intervention converts manageable dental issues into costly, complex procedures.
How Whitening Puts Your Gums at Risk When Cavities Are Present
Tooth pain isn’t the only consequence you risk when whitening over cavities — your gum tissue faces its own set of chemical threats.
Whitening agents that contact gum tissue directly cause irritation and chemical burns. When cavities sit near the gum line, peroxide-based gels seep into surrounding periodontal tissues far more easily, compromising gum health in ways that extend beyond cosmetic concern.
At-home whitening kits heighten this risk because ill-fitting trays and strips allow gel to leak freely onto soft tissue. If you’re also managing gum disease alongside cavities, your inflammatory response to whitening chemicals intensifies greatly.
Prioritizing whitening safety means addressing existing decay first — doing otherwise exposes vulnerable gum tissue to chemical damage that professional treatment may ultimately be required to correct.
Frequently Asked Questions
Can Whitening Toothpaste Cause the Same Risks as Bleaching Gels?
Whitening toothpaste carries lower risks than bleaching gels due to reduced whitening effectiveness, but you’ll still experience enamel sensitivity if cavities are present. It’s less aggressive, yet you shouldn’t ignore existing decay before use.
Are Certain Whitening Product Brands Safer for People With Cavities?
No brand’s a safe harbor when cavities exist. You shouldn’t trust brand effectiveness over dental reality — product ingredients like hydrogen peroxide penetrate decay regardless of label. See your dentist first.
Does Dental Insurance Cover Treatments Needed After Whitening Over Cavities?
Your dental insurance coverage typically won’t cover complications from elective whitening over cavities. You’ll likely pay out-of-pocket for treatment options like root canals or fillings, as insurers classify these as self-inflicted, preventable damages.
How Many Cavities Make Teeth Whitening Completely Unsafe to Attempt?
There’s no magic number — cavity severity, not quantity, determines your whitening safety. Even one deep cavity compromises whitening effectiveness and risks nerve damage, making dental evaluation essential before you attempt any whitening treatment.
Can Remineralizing Products Reduce Whitening Risks for Cavity-Prone Teeth?
Remineralizing products offer some remineralizing benefits and enamel protection, but they don’t eliminate whitening risks if you have active cavities. You should address existing decay with your dentist before attempting any whitening treatment.
References
- https://www.summercreekdentistry.com/blog/2021/05/02/the-dangers-of-teeth-whitening-while-you-have-cavities/
- https://www.lifetime.dental/blog/2024/12/13/dangerous-duo-why-cavities-and-teeth-whitening-dont-mix/
- https://www.evansstdental.com/blog/2025/04/04/cavities-and-teeth-whitening-a-dangerous-combination/
- https://www.lakeoconeedental.com/blog/why-cavities-and-teeth-whitening-are-a-dangerous-combination/
- https://www.dentistindallastx.com/blog/2025/06/30/why-cavities-and-teeth-whitening-are-a-dangerous-combination/
- https://www.bickfordandshirley.com/blog/cavities-teeth-whitening/
- https://www.moderndaysmiles.com/is-teeth-whitening-possible-with-cavities
- https://pearlzadehdds.com/common-dental-misconceptions/
- https://www.zumbrofamilydental.com/blog/dangers-cavities-teeth-whitening/