Whitening sensitive teeth can trigger sharp nerve pain called “zingers,” accelerate enamel erosion, and cause chemical burns to your gum tissue. Hydrogen peroxide penetrates compromised enamel more easily, reaching your dental pulp and potentially causing long-term nerve damage. Pre-existing conditions like cavities, cracked teeth, or exposed roots amplify these risks considerably. Two-thirds of patients report serious discomfort from over-the-counter products alone. Understanding each danger in detail will help you make a safer, more informed decision.
Key Takeaways
- Hydrogen peroxide penetrates compromised enamel more easily, triggering sharp “zinger” pains and intensifying sensitivity to hot, cold, and sweet stimuli.
- Repeated whitening without recovery periods increases the risk of long-term nerve damage, particularly when cavities or cracks create deeper penetration pathways.
- Bleaching agents strip essential minerals from already-thin enamel, increasing vulnerability to fractures and accelerating demineralization in sensitive teeth.
- Prolonged peroxide exposure can chemically burn and irritate gum tissue, with OTC ill-fitting trays significantly worsening this risk.
- Untreated dental issues like cavities, exposed roots, and enamel erosion can transform temporary discomfort into lasting pulp damage requiring serious intervention.
Why Sensitive Teeth React Badly to Whitening
When you whiten sensitive teeth, hydrogen peroxide or carbamide peroxide penetrates the enamel and reaches the dentin and pulp, triggering sharp, sudden pains known as “zingers.”
Sensitive teeth already have compromised or thinner enamel, meaning the peroxide encounters less resistance on its path to the nerve.
These whitening effects intensify pre-existing tooth sensitivity, making ordinary stimuli — heat, cold, or sweetness — unbearable.
Approximately two-thirds of patients using over-the-counter gels, strips, or paint-on films report significant discomfort. Higher peroxide concentrations amplify this reaction further.
Your enamel also temporarily dehydrates during treatment, compounding nerve irritation.
Without adequate enamel defense, peroxide reaches pulp tissue faster, prolonging discomfort beyond typical recovery windows of 24-72 hours.
Understanding this mechanism lets you make informed, controlled decisions about whitening.
How Bad Can Whitening Pain Get With Sensitive Teeth?
If you have pre-existing sensitivity, whitening can make hot, cold, or sweet stimuli nearly unbearable.
In severe cases, discomfort persists well beyond the typical 24-72 hour recovery window, signaling potential nerve irritation or pulp damage.
Effective pain management requires recognizing when symptoms cross from temporary to serious.
Knowing the difference between normal post-whitening sensitivity and a warning sign could save your smile.
If pain escalates, exploring whitening alternatives—such as desensitizing treatments or lower-concentration professional options—becomes essential to protecting your long-term dental health.
Does Whitening Erode Enamel When Your Teeth Are Already Sensitive?
Bleaching agents strip essential minerals from your enamel, and already-sensitive teeth face a compounded risk because their protective surface is often thinner or compromised to begin with.
Peroxide accelerates demineralization, leaving enamel softer, rougher, and increasingly vulnerable to fracture. If you’re overusing at-home kits without professional guidance, you’re directly undermining enamel integrity with every application.
Temporary tooth dehydration during whitening worsens the damage, intensifying both erosion and discomfort.
Worn enamel offers little resistance against aggressive bleaching concentrations, making sensitivity management a prerequisite—not an afterthought—before starting any whitening regimen.
Prioritize remineralizing treatments using nano-hydroxyapatite or fluoride to rebuild enamel density first.
Professional oversight guarantees you’re not accelerating irreversible structural loss while chasing cosmetic results your teeth currently can’t safely support.
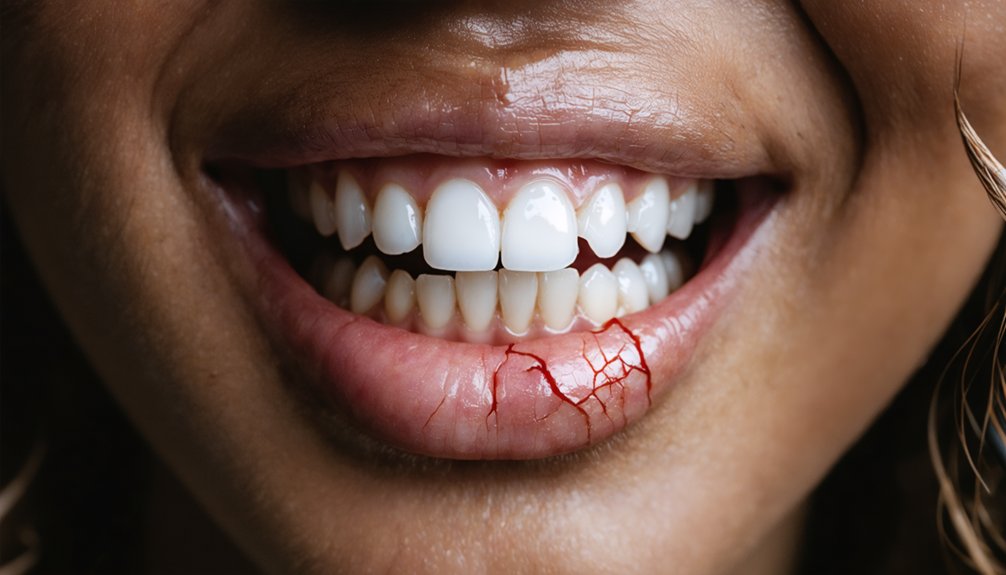
How Whitening Bleach Burns and Irritates Sensitive Gums
Hydrogen peroxide and carbamide peroxide don’t just target tooth stains—they aggressively contact surrounding gum tissue, triggering chemical burns, swelling, and gingival recession upon prolonged exposure. OTC products heighten this risk because ill-fitting trays and improper application allow bleaching agents to saturate vulnerable tissue.
Symptoms typically emerge within 24 hours and persist for several days, markedly delaying gum healing.
Irritation prevention requires strategic action on your part. Professional treatments incorporate protective barriers that shield gingival tissue from direct chemical contact, considerably reducing burn risk.
If your gums appear white or unusually sore post-treatment, seek immediate dental evaluation—these signs indicate chemical injury, not superficial irritation.
Avoiding prolonged exposure and choosing sensitivity-formulated products gives you measurable control over your tissue’s inflammatory response and recovery timeline.
Can Whitening Damage the Nerves in Sensitive Teeth?
When you apply whitening agents, the peroxide chemicals penetrate through your enamel and reach the inner pulp, directly irritating the nerves—particularly if you have cracked, decayed, or worn teeth that offer less protective barrier.
Repeated whitening sessions without adequate recovery periods compound this risk, progressively increasing the likelihood of long-term nerve damage rather than temporary sensitivity.
Pre-existing conditions like cavities or enamel erosion amplify this danger considerably, as compromised tooth structure accelerates peroxide’s pathway to vulnerable nerve tissue.
Chemicals Reaching Tooth Pulp
One of the most serious concerns with whitening sensitive teeth is the ability of peroxide-based chemicals to penetrate beyond the enamel and dentin, reaching the inner pulp where the tooth’s nerves reside.
Even brief chemical exposure during 5-15 minute sessions triggers pulp irritation. Your risk escalates considerably under these conditions:
- Cracked or decayed teeth create direct pathways for peroxide penetration.
- Worn enamel provides minimal barrier protection against chemical infiltration.
- Multiple sessions without recovery periods compound cumulative nerve damage.
- Pre-existing cavities amplify chemical exposure to vulnerable pulp tissue.
When peroxide reaches your pulp, temporary sensitivity can progress into persistent discomfort.
Understanding these mechanisms lets you make precise, informed decisions before initiating any whitening protocol.
Multiple Sessions Risk Damage
Repeated whitening sessions without adequate recovery intervals compound nerve irritation, elevating your risk of long-term pulp damage beyond temporary sensitivity. Each application drives peroxide deeper into already-compromised pulp tissue, intensifying inflammation with diminishing recovery capacity.
Without proper sensitivity management, consecutive treatments can shift reversible nerve irritation into persistent, chronic discomfort requiring professional intervention.
You’re not simply extending a cosmetic routine—you’re potentially forcing irreversible structural changes within your tooth’s nerve network. Dentists recommend spacing sessions strategically and monitoring cumulative exposure to prevent escalating damage.
If recurring sensitivity signals ongoing nerve stress, explore treatment alternatives like professional desensitizing applications or lower-concentration formulas with extended intervals.
Prioritizing pulp recovery over accelerated whitening timelines protects your long-term dental health and prevents complications that far outweigh cosmetic benefits.
Pre-Existing Conditions Amplify Risk
Pre-existing conditions like cavities, exposed roots, and enamel erosion dramatically amplify nerve damage risks when you undergo whitening treatments.
These vulnerabilities create direct pathways for peroxide to penetrate deeper, accelerating risk amplification beyond typical sensitivity responses.
Key pre-existing conditions that heighten danger:
- Cavities — Decay exposes inner dentin, allowing chemicals to reach pulp tissue faster.
- Exposed roots — Lack of enamel protection makes roots highly permeable to peroxide penetration.
- Enamel erosion — Weakened enamel provides minimal barrier against chemical infiltration.
- Worn enamel — Thinning surfaces intensify nerve irritation, increasing persistent discomfort risk.
Address these conditions with your dentist before attempting any whitening protocol.
Skipping this step risks irreversible nerve damage rather than temporary sensitivity.
Who Should Never Whiten Sensitive Teeth?
While whitening can benefit many patients, certain conditions make it contraindicated entirely. If you have active gum disease, untreated cavities, or significant enamel erosion, peroxide penetration worsens these sensitive conditions rather than improving your smile.
Exposed roots and cracked teeth create direct pathways for chemicals to reach nerve tissue, escalating damage beyond reversible sensitivity.
You should also postpone whitening during pregnancy or breastfeeding, as peroxide safety remains understudied in these populations.
Severe pre-existing sensitivity warrants desensitizing treatment before considering any bleaching protocol.
When these contraindications apply, explore whitening alternatives like professional cleaning, nano-hydroxyapatite toothpaste, or composite bonding to improve appearance without risk.
Your dentist can assess your specific risk profile and recommend the safest, most effective path forward.
How to Whiten Safely if You Have Sensitive Teeth
Not every sensitive-tooth patient needs to avoid whitening altogether—many can bleach safely with the right precautions in place. Implementing targeted sensitivity solutions before, during, and after treatment markedly reduces your risk.
- Use desensitizing toothpaste containing potassium nitrate or nano-hydroxyapatite for two weeks pre-treatment to calm nerve pathways and reinforce enamel.
- Select gentle whitening formulas designed specifically for sensitive teeth, using lower peroxide concentrations to minimize pulp irritation.
- Space out your sessions to allow enamel remineralization and nerve recovery between applications.
- Consult a dentist who can apply protective gum barriers, prescribe professional-grade desensitizing agents, and monitor enamel integrity throughout the process.
Avoiding extreme temperatures and acidic foods post-treatment further protects your teeth while you achieve measurable whitening results.
Frequently Asked Questions
Can Whitening Products Permanently Stain or Discolor Already Sensitive Teeth?
Whitening products don’t permanently stain sensitive teeth, but they can compromise tooth enamel integrity. Overuse produces long-term effects like demineralization, leaving surfaces rough or uneven, which you’ll want to actively prevent through professional oversight.
Are Natural or Charcoal Whitening Alternatives Safer for Sensitive Teeth?
Natural remedies and charcoal effectiveness remain unproven for sensitive teeth. Charcoal’s abrasiveness can accelerate enamel erosion, worsening your sensitivity. You’re better protected choosing clinically-tested desensitizing toothpaste with nano-hydroxyapatite, which rebuilds enamel without introducing additional damage risks.
How Long Should You Wait Between Whitening Sessions With Sensitive Teeth?
Wait at least 48-72 hours between sessions for effective sensitivity management. You should monitor your whitening frequency carefully, allowing nerves and enamel to recover fully before resuming treatment to prevent compounding irritation or lasting damage.
Does Teeth Whitening Interact Negatively With Sensitivity Medications or Treatments?
While it won’t cancel your treatment, whitening techniques can reduce desensitizing agents’ effectiveness. You’re actively lowering your sensitivity levels when peroxide penetrates enamel, temporarily overriding potassium nitrate or nano-hydroxyapatite protection you’ve built up.
Can Children or Teenagers With Sensitive Teeth Safely Use Whitening Products?
You shouldn’t use whitening products on children or teenagers with sensitive teeth. Youth dental health demands caution, as developing enamel faces higher damage risks. Follow safe whitening guidelines and consult your dentist before considering any treatment.
References
- https://www.cornerstonedentistryvan.com/the-hidden-dangers-of-teeth-whitening-treatments/
- https://www.blvddentistry.com/can-you-get-whitening-treatment-with-sensitive-teeth/
- https://www.thesuperdentists.com/sensitive-teeth-hurting-after-whitening/
- https://www.suttonpda.com/sensitivity-safety-teeth-whitening/
- https://www.covefamilydental.com/teeth-whitening-risks/
- https://www.northroyaltonfamilydental.com/blog/the-dangers-of-over-whitening/
- https://www.centerportdental.com/blog/is-teeth-whitening-safe-for-sensitive-teeth/
- https://www.goodrx.com/conditions/dental-care/sensitive-teeth-after-whitening
- https://pubmed.ncbi.nlm.nih.gov/23846062/