You can whiten aging teeth safely and effectively, but results depend on understanding what’s driving the discoloration. Thinning enamel and natural dentin darkening limit how bright your teeth can get, while deep stains from coffee, tea, or tobacco require stronger professional-grade treatments. Sensitivity risks increase with age, so professional oversight helps minimize side effects. The right approach makes a real difference, and each factor covered below will help you make the most informed decision.
Key Takeaways
- Aging teeth can be whitened, but thinning enamel and dentin darkening create natural limitations that affect achievable results.
- Professional whitening uses higher peroxide concentrations to penetrate deep stains, though existing restorations like crowns won’t respond to treatment.
- Older adults face heightened sensitivity risks due to thinner enamel, making professional oversight essential for safe, customized treatment.
- Non-peroxide alternatives like bromelain and PAP offer gentler options for removing surface stains without risking enamel damage.
- Completing whitening before replacing restorations ensures accurate color matching, preventing costly aesthetic mismatches between natural teeth and dental work.
Why Aging Teeth Stain and Discolor Over Time
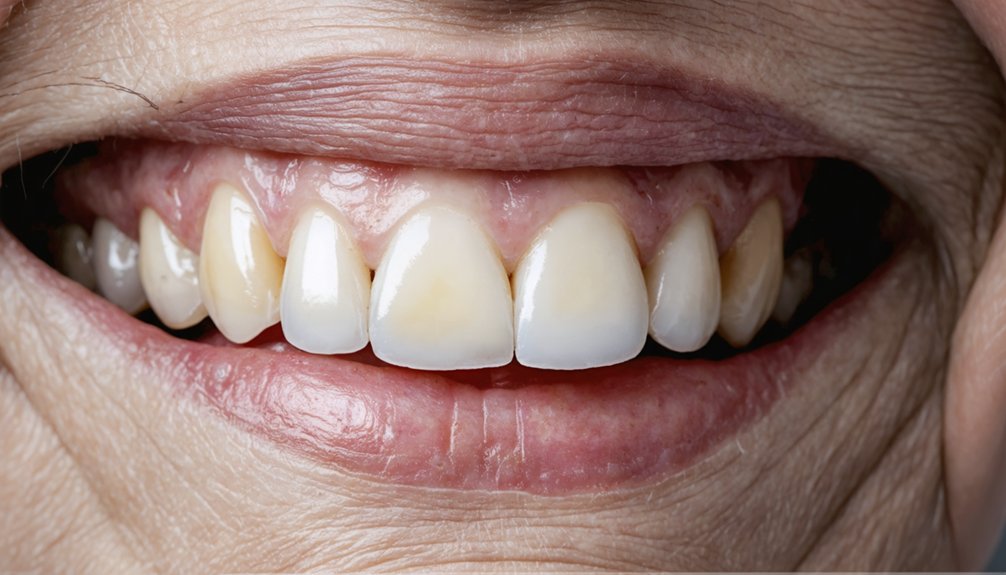
As you age, your teeth undergo structural and compositional changes that make discoloration increasingly difficult to avoid. Enamel gradually thins, exposing the naturally darker dentin beneath. Simultaneously, dentin itself darkens over time, compounding the effect.
These aging factors combine to produce a yellowed or grayish appearance that surface cleaning alone can’t address.
Lifestyle impacts accelerate this process considerably. Decades of consuming chromogenic substances like coffee, tea, and red wine embed stains deep within enamel. Tobacco use introduces persistent, stubborn discoloration that resists standard hygiene efforts.
Even certain medications taken over time contribute to intrinsic staining.
Understanding these underlying causes helps you make informed decisions about whitening interventions. Discoloration in aging teeth isn’t simply cosmetic neglect—it reflects cumulative biological and behavioral factors requiring targeted, professional strategies.
Is Teeth Whitening Actually Safe for Older Adults?
If you’re an older adult considering teeth whitening, you’ll face higher risks than younger patients, including increased sensitivity, gum irritation, and potential damage to existing restorations due to thinner enamel and exposed dentin.
Professional oversight markedly reduces these risks by allowing your dentist to evaluate your gum health, identify vulnerable areas, and customize treatment to your specific oral conditions.
Without that assessment, you’re more likely to experience the temporary sensitivity that affects up to 80% of peroxide users—a concern that’s amplified when aging teeth already compromise your enamel’s protective capacity.
Risks for Seniors
Teeth whitening is generally safe for older adults, but the aging process introduces specific risks that make professional oversight essential. Your enamel thins over time, exposing dentin and markedly increasing sensitivity. Between 43% and 80% of peroxide users experience temporary sensitivity, making sensitivity management a critical consideration before starting any whitening protocol.
Receding gums expose root surfaces, heightening irritation risk during treatment. Aggressive bleaching can also alter enamel’s surface microstructure, causing long-term damage to already compromised teeth.
Restoration compatibility presents another challenge. Peroxide doesn’t whiten crowns, veneers, or sealants, and chemical reactions with these materials can cause unexpected changes.
A dentist evaluates your restorations, gum health, and enamel condition beforehand, giving you precise control over outcomes while minimizing preventable harm.
Professional Oversight Benefits
Professional oversight transforms teeth whitening from a risky guessing game into a controlled, evidence-based procedure tailored to your aging dentition.
Under professional supervision, your dentist evaluates gum recession, enamel thickness, and existing restorations before selecting appropriate whitening techniques.
This structured approach delivers three critical advantages:
- Customized concentration control — your dentist adjusts peroxide levels to minimize sensitivity while maximizing effectiveness.
- Pre-treatment risk assessment — gum health and exposed dentin are identified and addressed before whitening begins.
- Restoration compatibility screening — crowns and sealants are evaluated to prevent chemical reactions or uneven coloring.
Without professional supervision, you’re fundamentally guessing.
With it, you’re making calculated, informed decisions that protect your enamel, manage sensitivity, and produce measurably better outcomes for aging teeth.
Sensitivity and Enamel Concerns
While teeth whitening is generally safe for older adults, the risks of sensitivity and enamel damage are measurably higher than they’re for younger patients.
As you age, your enamel thins and dentin becomes exposed, which amplifies tooth sensitivity during and after whitening treatments. Research shows that 43% to 80% of peroxide users experience temporary sensitivity, and that figure skews higher for older patients with receding gums.
Enamel erosion becomes a real concern if you overuse bleaching agents or choose aggressive concentrations without professional guidance.
Thinner enamel offers less protection against peroxide penetration, increasing nerve irritation and structural vulnerability. You can reduce these risks considerably by having a dentist evaluate your enamel thickness and gum condition before starting any whitening protocol.
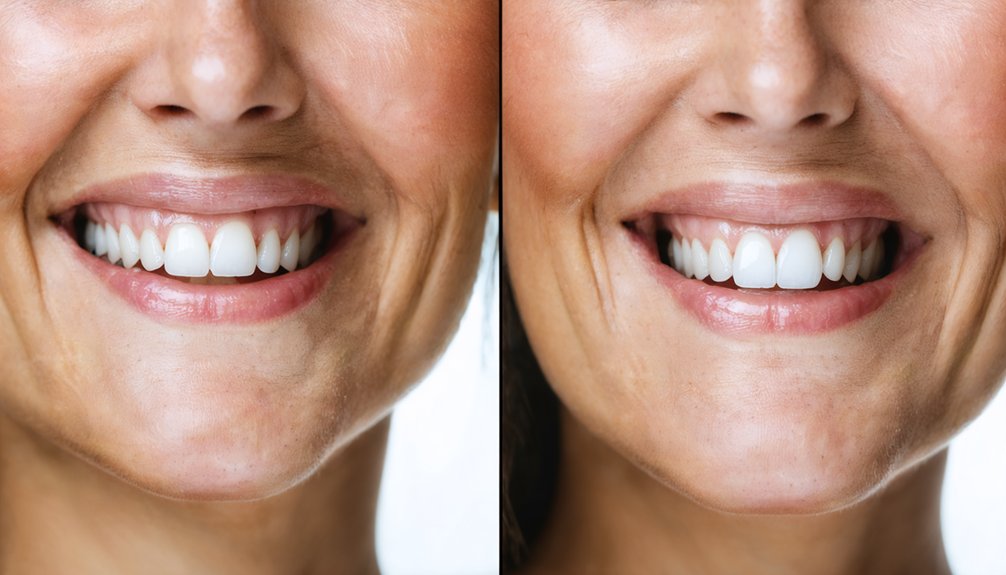
How Well Does Professional Whitening Work on Aging Teeth?
When it comes to aging teeth, professional whitening delivers some of the most effective results available. Higher peroxide concentrations used in whitening techniques penetrate deeper stains that aging effects produce over decades.
However, you should understand these key realities:
- Natural limits exist — dentin darkening and enamel thinning restrict how white your teeth can ultimately become.
- Restorations won’t respond — crowns and veneers remain unchanged, potentially requiring replacement for uniform color matching.
- Genetics and lifestyle matter — your achievable results depend on factors beyond technique alone.
Despite these limitations, in-office treatments remain your strongest option for meaningful improvement.
A professional assessment guarantees the approach suits your specific oral health condition before treatment begins.
What Professional Whitening Still Cannot Change About Your Teeth
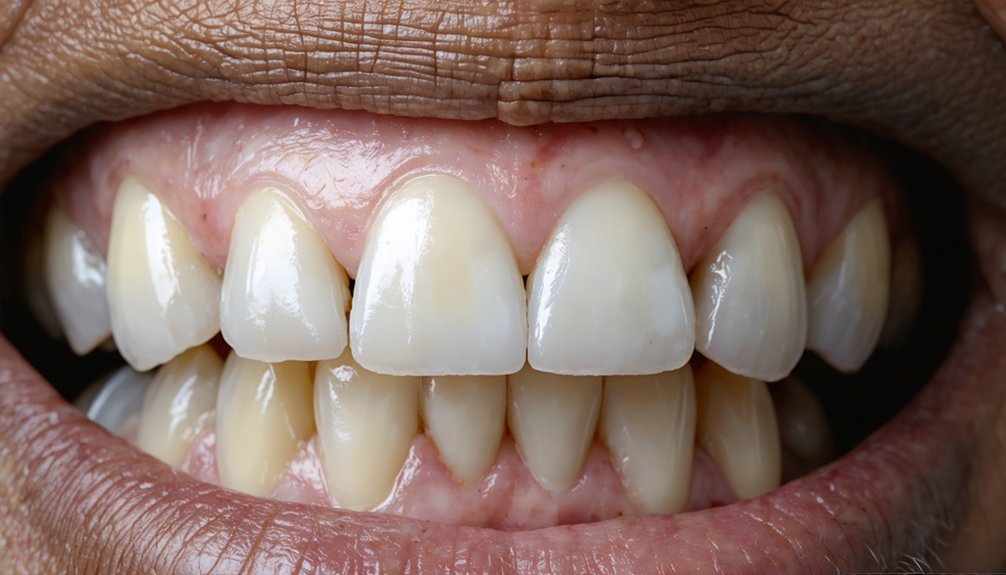
Even with the most advanced in-office treatments, certain structural and restorative factors remain beyond whitening’s reach. Understanding these limits dismantles common whitening myths and resets aging perceptions about achievable outcomes.
Natural dentin darkening progresses with age, and no bleaching agent reverses this internal shift. Enamel thinning similarly restricts how bright your results can appear. Genetics and lifestyle choices further define your ceiling, regardless of treatment strength.
Aging darkens dentin from within—no bleaching agent can reverse what genetics and time have already decided.
Dental restorations—crowns, veneers, and sealants—don’t respond to peroxide. If your crowns predate whitening treatment, they’ll visibly contrast against newly brightened natural teeth, requiring replacement for uniform aesthetics.
Chemical interactions between bleaching agents and existing restorations also introduce unpredictable outcomes.
Knowing these boundaries lets you make informed decisions, set realistic expectations, and plan strategically with your dentist before committing to treatment.
Is It Safe to Whiten Teeth When You Have Crowns or Fillings?
Whitening your teeth when you have crowns or fillings is generally safe, but the process carries specific complications you need to understand before starting.
Bleaching agents don’t alter restorations, creating visible color mismatches once your natural teeth brighten. Chemical reactions between peroxide and crown or sealant materials can also compromise their integrity.
Control these risks by following three critical steps:
- Schedule a professional assessment to evaluate your restorations’ condition before any whitening treatment.
- Understand crowns safety limitations—your crowns won’t respond to peroxide, requiring replacement afterward for uniform results.
- Address fillings whitening boundaries—composite fillings may discolor unevenly, demanding strategic planning with your dentist.
Working with a professional guarantees you whiten effectively while protecting your existing dental work from unnecessary damage.
When Aging Teeth Need New Restorations After Whitening
If you whiten your teeth and your existing crowns, veneers, or fillings no longer match your brighter smile, you’ll likely need to replace those restorations to achieve a uniform appearance.
Dentists recommend completing your whitening treatment first, then waiting one to two weeks for your tooth color to stabilize before matching new restorations to your whitened shade.
This sequencing guarantees your dental lab can accurately fabricate replacements that align with your post-whitening results rather than your previous, darker baseline.
Restoration Replacement After Whitening
Although teeth whitening can brighten your natural enamel, it doesn’t affect dental restorations like crowns, veneers, or bonding—which means mismatches in tooth color often become visible after treatment.
To maintain color matching and restoration longevity, you’ll need a strategic approach:
- Complete whitening first — Finalize your whitening treatment before replacing any restorations so your dentist can accurately match the new shade.
- Wait two weeks — Allow your enamel color to stabilize post-treatment before selecting restoration materials.
- Replace outdated restorations — Crowns or bonding that appear darker than your whitened teeth require replacement to achieve a uniform result.
Coordinating this sequence with your dentist guarantees your restorations complement your natural teeth precisely and maintain aesthetic consistency long-term.
Matching New Dental Restorations
Once your whitened shade has stabilized, matching new restorations to your natural teeth becomes the next step in completing your smile’s aesthetic transformation.
Your dentist uses shade guides and digital color-matching technology to select restoration materials—porcelain, composite resin, or ceramic—that precisely mirror your post-whitening tone.
Waiting two weeks after treatment guarantees your tooth color has fully settled before fabrication begins. This timing prevents mismatches that require costly replacements later.
Porcelain restorations offer superior color stability and resist future staining, making them a practical long-term choice for aging teeth.
Your dentist documents your achieved shade numerically, giving technicians exact specifications for crafting restorations.
Accurate color matching eliminates visible discrepancies between natural teeth and restorations, delivering a cohesive, uniform result that reflects intentional clinical planning rather than chance.
The Real Limits of At-Home Whitening Products for Aging Teeth
Over-the-counter whitening products promise convenience, but they fall considerably short for aging teeth.
At-home limitations stem from low hydrogen peroxide concentrations that can’t penetrate aging stains embedded deep within dentin. You’re fundamentally treating surface discoloration while the structural causes remain untouched.
Three critical shortcomings define these products:
- Insufficient peroxide levels produce minimal whitening compared to professional-grade treatments.
- Ineffectiveness against deep stains means age-related discoloration persists despite consistent use.
- Overuse risks include enamel erosion and microstructural damage, particularly dangerous for already-thinning aging enamel.
Non-peroxide alternatives like bromelain and PAP offer gentler options but deliver even less whitening power.
If you want meaningful results, professional oversight isn’t optional—it’s necessary.
Side Effects That Hit Harder as Teeth Age
As your teeth age, you face a heightened risk of sensitivity and gum irritation when whitening, since thinning enamel and receding gums expose the dentin beneath.
Peroxide-based treatments trigger temporary sensitivity in 43% to 80% of users, but aging teeth amplify that discomfort considerably.
You’ll also risk enamel surface alterations if you use aggressive bleaching agents, making professional oversight essential before starting any whitening regimen.
Sensitivity and Gum Irritation
Tooth sensitivity and gum irritation rank among the most common side effects of whitening treatments, affecting anywhere from 43% to 80% of peroxide users. As you age, thinning enamel and receding gums amplify these reactions greatly.
Effective sensitivity management starts with understanding your specific vulnerabilities before treatment begins.
Three evidence-based strategies support your gum health and comfort:
- Use dentist-prescribed desensitizing agents containing potassium nitrate or fluoride before and after whitening sessions.
- Limit treatment duration and peroxide concentration based on professional assessment of your enamel thickness.
- Avoid acidic foods and beverages 48 hours post-treatment to reduce irritation.
You’re not powerless against these side effects.
Professional oversight lets you adjust protocols precisely, minimizing discomfort while still achieving meaningful whitening results.
Enamel Thinning Risks
Enamel naturally thins as you age, and aggressive bleaching accelerates that loss by altering the tooth’s microstructure. Thinner enamel exposes the underlying dentin, increasing sensitivity and vulnerability to chemical damage.
High-concentration peroxides, when overused, cause surface alterations that compromise enamel preservation long-term.
You can control this risk by choosing professional whitening techniques over unsupervised at-home overuse. A dentist evaluates your enamel thickness before treatment, selecting appropriate peroxide concentrations and application times. This targeted approach delivers results without unnecessary structural compromise.
Avoid household hydrogen peroxide entirely—its unregulated use heightens erosion risk considerably.
Overusing OTC strips compounds damage by repeatedly exposing already-thin enamel to chemical stress. Strategic, professionally guided whitening preserves both your results and your tooth structure.
Non-Peroxide Whitening Options That Are Safer for Aging Teeth
For seniors with sensitive teeth or compromised enamel, non-peroxide whitening agents offer a gentler path to a brighter smile. These alternatives let you manage sensitivity while still achieving visible improvement:
- Bromelain benefits include effective surface stain removal without cytotoxicity or enamel microstructure changes, making it a safe enzymatic option for aging teeth.
- PAP effectiveness delivers measurable whitening with no reported enamel alterations, though results fall short of peroxide-based treatments.
- Sodium bicarbonate and whitening mouthwashes with minimal peroxide support daily hygiene while providing mild brightening.
You should understand that these options work best on surface stains rather than deep, age-related discoloration.
Consult your dentist to determine which agent aligns with your enamel condition, sensitivity levels, and whitening goals.
Dentist-Approved Steps for Whitening Without Damaging Aging Teeth

Following four dentist-approved steps can protect your aging teeth while still achieving meaningful whitening results.
First, consult your dentist to assess gum recession, enamel thickness, and existing restorations before selecting whitening techniques. Age-related factors like dentin darkening and enamel thinning directly affect treatment choices.
Second, choose professional or custom-fitted tray systems over OTC strips, which rarely penetrate deep stains effectively.
Third, follow application instructions precisely—overuse accelerates enamel erosion and heightens sensitivity.
Fourth, maintain consistent oral hygiene by brushing, flossing, and limiting acidic foods that weaken enamel further.
If your restorations no longer match your whitened teeth, discuss replacement options with your dentist.
These structured steps give you meaningful control over outcomes while minimizing risks associated with aging oral tissues.
Frequently Asked Questions
Can Teeth Whitening Interact Negatively With Blood Pressure or Diabetes Medications?
Direct evidence of teeth whitening causing medication interactions with blood pressure or diabetes drugs is limited, but you should consult your dentist, as teeth sensitivity and systemic health conditions can complicate your whitening treatment plan.
How Often Should Seniors Repeat Professional Whitening Treatments Annually?
Ironically, less is more—you should limit professional whitening frequency to once or twice yearly. Your dentist customizes treatment duration based on sensitivity, enamel condition, and stain depth, ensuring you maintain control over safe, effective results.
Does Dental Insurance Ever Cover Whitening Procedures for Older Adults?
Most insurance policies don’t cover whitening since it’s cosmetic. You’ll likely face coverage limitations, so consult your dentist to explore flexible spending accounts or payment plans that help you manage whitening costs effectively.
Can Whitening Worsen Existing Jaw Pain or TMJ Issues in Seniors?
With 43%-80% experiencing whitening sensitivity, you’ll want to consult your dentist if you have jaw pain or TMJ issues, as treatment options should protect your oral health while minimizing discomfort risks.
Are There Specific Whitening Risks for Seniors With Dry Mouth Conditions?
Yes, dry mouth heightens whitening risks by reducing saliva’s protective buffering. You’ll want to explore dry mouth remedies before treatment and consider whitening alternatives like PAP, which won’t further irritate sensitive, moisture-deprived aging teeth.
References
- https://mccannltc.net/blog/evaluating-safety-teeth-whitening-seniors
- https://sunlakesdentistry.com/can-senior-teeth-be-whitened/
- https://health.clevelandclinic.org/is-teeth-whitening-safe
- https://www.doctorrichardlondon.com/can-older-people-whiten-their-teeth/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC9915942/
- https://www.doverfamilydentistry.org/teeth-whitening-for-aging/
- https://blog.ultradent.com/does-aging-make-it-harder-to-whiten-teeth
- https://www.bu.edu/articles/2012/the-truth-about-teeth-whiteners/