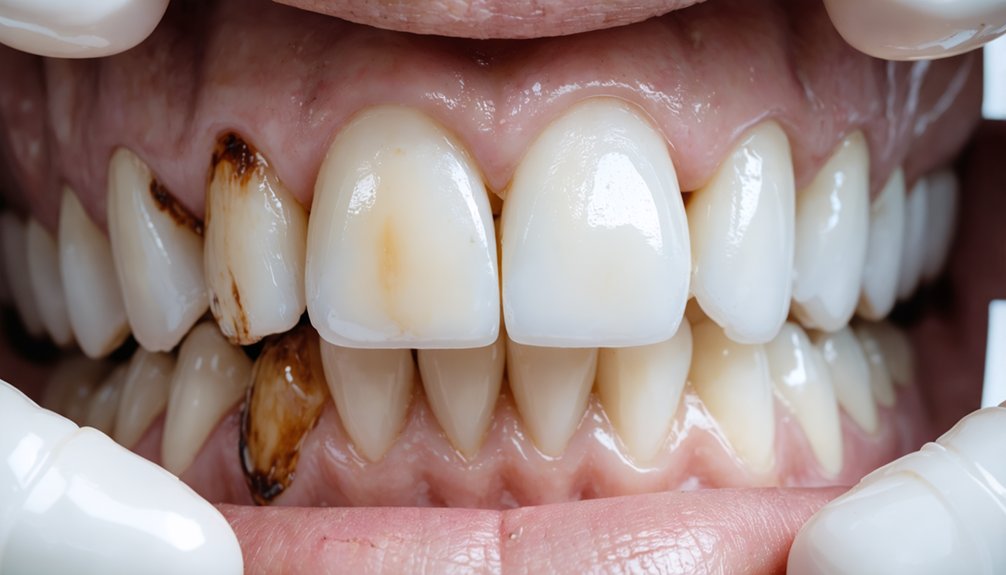
Deep fluoride stains form within your enamel’s structure, making standard whitening products ineffective. Your best options include professional bleaching with 25–40% hydrogen peroxide, microabrasion for superficial-to-moderate stains, and resin infiltration for early-stage white spots. Combining treatments—like microabrasion followed by bleaching—can maximize results, with mild cases seeing 60–70% improvement. Severe stains may only improve 20–40%, making veneers worth considering. The right approach depends on your stain’s depth, and there’s much more to uncover about each technique.
Key Takeaways
- Deep fluoride stains are intrinsic, making standard whitening ineffective; professional treatments using 25–40% hydrogen peroxide are required for meaningful results.
- Microabrasion removes 100–200 micrometers of discolored enamel, achieving 80–90% stain removal in superficial fluorosis within one to three appointments.
- Resin infiltration seals hypomineralized lesions non-invasively, delivering immediate aesthetic improvement for early-stage fluorosis, though it cannot mask deep discoloration.
- Combination therapy, such as microabrasion paired with professional bleaching, maximizes effectiveness for moderate-to-severe cases where single treatments yield limited improvement.
- For deep stains, bleaching alone improves appearance by only 20–40%; veneers are recommended when other treatments prove insufficient.
Why Deep Fluoride Stains Are Hard to Whiten
Deep fluoride stains resist whitening because they originate within the enamel’s structural matrix rather than on its surface. Understanding the stain causes clarifies why standard approaches fall short.
During tooth development, excess fluoride disrupts mineralization, embedding discoloration into hypomineralized enamel layers. Surface treatments can’t penetrate these structural deficits effectively.
Excess fluoride during development embeds discoloration deep within enamel, where surface treatments simply cannot reach.
You’re also likely encountering treatment myths that misrepresent what whitening can achieve. Over-the-counter products target surface chromogens, not intrinsic structural staining.
Even professional bleaching improves severe deep stains by only 20–40%, confirming that no single solution eliminates them entirely. The porous, hypomineralized enamel absorbs peroxide unevenly, limiting consistent results.
Recognizing these biological realities lets you pursue accurate severity assessments and targeted professional interventions rather than ineffective remedies.
What to Expect From Professional Bleaching on Severe Stains
Once you understand why severe fluoride stains resist standard treatments, professional bleaching becomes a more realistic option to evaluate.
Dentists use 25–40% hydrogen peroxide concentrations, applied in 15–20 minute intervals with light activation, to maximize penetration into discolored enamel.
However, you should calibrate your treatment expectations carefully. Severe, deep stains typically yield only 20–40% improvement with bleaching alone.
Professional results depend heavily on stain depth, enamel integrity, and session frequency. Multiple appointments, spaced 1–2 weeks apart, are often necessary to achieve measurable change.
If bleaching alone proves insufficient, your dentist may recommend combining it with microabrasion or resin infiltration.
For the most advanced cases, veneers remain the most predictable solution for achieving a uniform, aesthetically acceptable outcome.
Bleaching Options That Cause Less Sensitivity
Sensitivity is a common concern when bleaching fluoride-stained enamel, but lower-concentration agents and alternative compounds can greatly reduce discomfort without sacrificing results.
Carbamide peroxide is a strong option for sensitivity reduction, as it releases hydrogen peroxide slowly, minimizing irritation in compromised enamel. This controlled release also supports enamel preservation by avoiding aggressive oxidation that higher concentrations can trigger.
Sodium hypochlorite offers another alternative, oxidizing organic material within hypomineralized lesions without peroxide-related gingival irritation. Your dentist may combine it with resin perfusion afterward to seal treated enamel and block future staining.
If you have mild-to-moderate fluorosis, these gentler agents deliver measurable improvement while keeping post-treatment discomfort manageable. Always discuss your sensitivity history with your dentist to identify the most appropriate bleaching protocol for your specific enamel condition.
How Microabrasion Removes Deep Fluorosis Stains
While gentler bleaching agents handle surface-level organic staining well, they often fall short against the deeper discolorations that moderate fluorosis produces. Microabrasion directly addresses this limitation by removing 100–200 micrometers of discolored enamel using a hydrochloric acid and pumice mixture applied in controlled circular motions.
You’ll find that microabrasion benefits extend beyond stain removal — the technique targets only compromised areas, making enamel preservation a central advantage. Rather than treating the entire surface indiscriminately, your dentist focuses precisely on stained zones, leaving healthy enamel intact.
Clinical outcomes support this precision: microabrasion achieves 80–90% stain removal in superficial fluorosis and 50–70% in mild-to-moderate cases.
Expect temporary sensitivity lasting 24–48 hours post-procedure — a minor trade-off for measurable, lasting structural improvement.
What Resin Infiltration Can and Can’t Do for Fluorosis Stains
If you’re dealing with early-stage fluorosis white spots, resin infiltration offers a non-invasive solution that penetrates porous enamel, seals hypomineralized lesions, and delivers immediate aesthetic improvement without drilling or discomfort.
You can also combine it with professional bleaching to enhance organic stain removal for more thorough results.
However, if your fluorosis stains are severe or deeply embedded, resin infiltration won’t provide sufficient coverage, and you’ll likely need to explore more aggressive treatments like microabrasion, veneers, or bonding.
Resin Infiltration’s Key Benefits
Resin infiltration stands out as one of the most conservative options for addressing fluorosis-related white spots, particularly in early-stage cases with minimal enamel loss.
Its resin advantages center on a non-invasive process that requires no drilling, no anesthesia, and no removal of healthy tooth structure. You’re preserving natural enamel while the resin penetrates hypomineralized lesions, sealing porous zones to block future chromogen absorption.
This enamel preservation approach delivers immediate aesthetic improvement, with white spot opacity visibly reduced after a single session.
When you combine resin infiltration with professional bleaching, you’ll target both structural discoloration and residual organic staining simultaneously.
It’s an evidence-backed method that gives you precise control over treatment intensity without sacrificing structural integrity or subjecting your teeth to aggressive intervention.
Limitations With Severe Stains
Despite resin infiltration‘s strengths in early-stage fluorosis, it reaches clear boundaries when stain severity increases. When you’re dealing with moderate-to-severe fluorosis, resin can’t penetrate deep enough to mask brown or yellow discoloration embedded within the enamel’s subsurface layers.
Accurate stain identification determines whether infiltration is even worth attempting. Your dentist evaluates lesion depth, opacity, and mineral loss before committing to any protocol. Without this assessment, you risk investing in a procedure that delivers incomplete results.
Treatment personalization becomes non-negotiable at this stage. Resin infiltration works best as one component within a broader strategy—combined with microabrasion or professional bleaching—rather than a standalone solution.
For severe cases, veneers or bonding often deliver the coverage and aesthetic control that infiltration alone simply can’t achieve.
Microabrasion Plus Bleaching: Why Sequencing Treatments Gets Better Results
Combining microabrasion with professional bleaching reveals results that neither treatment achieves alone. When you sequence treatments correctly, microabrasion removes 100–200 micrometers of discolored enamel first, creating a smoother surface that accepts bleaching agents more effectively. That foundation matters.
Your stain assessment determines the order. Microabrasion targets superficial fluorosis, achieving 80–90% stain removal before bleaching addresses deeper intrinsic discoloration.
Stain assessment directs the sequence—microabrasion clears superficial fluorosis first, setting the stage for deeper bleaching work.
Professional bleaching then penetrates the refreshed enamel layer with 25–40% hydrogen peroxide concentrations, amplifying whitening outcomes remarkably.
Treatment sequencing also reduces overall sensitivity by eliminating surface debris before chemical agents contact enamel. If deep staining persists after both treatments, veneers or bonding address remaining imperfections.
You’re directing each phase strategically, not guessing—and that precision consistently outperforms single-treatment approaches for moderate-to-severe fluoride stains.
How to Match Treatment to Your Stain Depth
Stain depth dictates which treatment protocol your dentist will recommend, so understanding severity levels directly shapes your outcome expectations.
Your dentist’s stain assessment determines whether you need conservative or aggressive intervention.
For superficial fluorosis, microabrasion removes 80-90% of discoloration efficiently.
Mild-to-moderate cases respond better to combined microabrasion and professional bleaching, achieving measurable improvements through treatment customization.
Icon resin infiltration targets early-stage white spots without drilling, making it ideal when enamel loss remains minimal.
Deep, severe stains realistically yield only 20-40% improvement through bleaching alone, making veneers the more predictable option.
You’ll want to discuss enamel thickness, stain penetration depth, and sensitivity history with your dentist before committing to any protocol.
Matching intervention to severity prevents wasted time and unnecessary enamel loss.
How Long Do Deep Fluoride Stain Treatments Last?
When you pursue deep fluoride stain treatment, you should know that results vary greatly depending on the method used, with professional bleaching typically lasting one to three years before touch-ups become necessary.
You can extend those results considerably by committing to a consistent maintenance routine, including periodic in-office sessions and avoiding stain-promoting foods and beverages.
If you opt for combination therapy—such as microabrasion followed by professional bleaching—you’ll generally achieve longer-lasting outcomes, since the sequential approach addresses both surface and deeper stains more thoroughly.
Treatment Duration Varies
Treatment duration for deep fluoride stains varies greatly depending on the severity of discoloration and the method your dentist selects. Your treatment timeline typically spans several weeks to months.
Professional bleaching requires multiple sessions spaced 1-2 weeks apart, while microabrasion delivers results within one to three appointments. Resin infiltration often achieves visible improvement in a single visit.
Your patient experience will differ based on stain depth. Mild fluorosis responds faster, showing 60-70% improvement with bleaching alone.
Moderate-to-severe cases demand combination approaches—microabrasion followed by bleaching—extending your timeline but yielding superior outcomes. Severe deep stains may ultimately require veneers for complete correction.
Consult your dentist for a severity assessment so you can establish realistic expectations and maintain control over your treatment decisions.
Maintenance Extends Results
Once your dentist completes your fluoride stain treatment, results can last anywhere from one to three years depending on the method used and how well you maintain them.
Combination therapies, like microabrasion followed by bleaching, typically deliver longer-lasting outcomes than single treatments.
Apply these maintenance tips consistently to protect your investment:
- Avoid staining foods, beverages, and tobacco that reintroduce chromogens into treated enamel
- Use dentist-approved whitening products with low-concentration peroxide for periodic touch-ups
- Schedule professional reassessments every six months to monitor enamel integrity and stain recurrence
Severe fluorosis cases may require earlier retreatment, while superficial stain corrections hold longer with disciplined care.
You control how long your results last.
Combination Therapy Lasts Longer
Combination therapy outlasts single-treatment approaches because it addresses fluoride stains at multiple depths simultaneously.
When you pair microabrasion with professional bleaching, you’re removing surface discoloration while targeting deeper intrinsic stains—maximizing treatment effectiveness across all fluorosis severities.
Adding resin infiltration seals treated enamel, blocking future chromogens from penetrating and extending your long-term benefits considerably.
Sequential treatments also create a smoother enamel foundation, helping subsequent whitening agents penetrate more uniformly.
You’ll maintain results longer because each layer of treatment reinforces the previous one, reducing the likelihood of rapid re-staining.
Dentists typically recommend combination protocols for moderate-to-severe cases where single treatments yield only 20-40% improvement.
You’re investing in durability, not just immediate results—and that distinction determines how long your whitening outcomes actually hold.
Frequently Asked Questions
Can Deep Fluoride Stains Return After Professional Whitening Treatments Are Completed?
Yes, deep fluoride stains can return. You’ll need consistent long-term maintenance and stain reversal methods like combination therapies to preserve results. Professional treatments outperform over-the-counter options, but you must follow your dentist’s recommended maintenance plan.
Are Combination Fluorosis Treatments Covered by Dental Insurance Plans?
Your smile investment faces a coverage gap—most dental insurance plans don’t cover combination fluorosis treatments, as they’re deemed cosmetic. You’ll typically self-fund fluoride stain prevention procedures, so consult your dentist for cost-effective, evidence-based insurance coverage options.
What Age Is Appropriate to Begin Treating Severe Fluoride Stains?
You should consider early intervention around age 14-16, once permanent teeth fully erupt. At this stage, you’ll find treatment options like microabrasion and professional bleaching become viable, yielding ideal results for severe fluoride stains.
Can Fluorosis Stain Treatments Be Performed During Pregnancy Safely?
You should avoid fluorosis treatment options during pregnancy, as pregnancy dental safety guidelines restrict bleaching agents and microabrasion. Consult your dentist to defer elective procedures until postpartum, ensuring both your safety and your baby’s wellbeing.
Do Fluorosis Whitening Treatments Affect Dental Crowns or Existing Restorations?
Imagine your restorations standing untouched while whitening works around them—fluorosis treatments won’t alter crowns or existing restorations. You’ll notice uneven shading, though, as bleaching doesn’t affect crown longevity or restoration compatibility, requiring replacement for uniform results.
References
- https://drbvreddysdental.com/what-are-the-best-treatment-options-for-fluorosis-affected-teeth/
- https://teethwhiteninghochiminh.com/best-fluorosis-teeth-whitening/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC4606706/
- https://www.hazendentistry.com/blog/3-ways-you-can-treat-fluoride-stains-on-your-teeth.php
- https://warrdental.com/treating-deep-stains/
- https://www.colgate.com/en-us/oral-health/teeth-whitening/teeth-stain-removal-types
- https://www.dentistryofoldtownscottsdale.com/dental-blog/how-to-remove-white-stains-from-teeth/
- https://www.designerforsmiles.com/cosmetic-dentistry/how-can-i-treat-deep-stains-on-my-teeth/
- https://lindsayfamilydental.com/blog/how-teeth-whitening-targets-discoloration-and-stain/