Your teeth can discolor after whitening due to several factors. The treatment temporarily dehydrates your enamel, which initially creates a whiter appearance but reverses as rehydration occurs. Whitening also increases enamel porosity, making your teeth more susceptible to staining from coffee, tea, and acidic beverages. Additionally, bleaching agents can’t penetrate intrinsic stains from medications or trauma, and they won’t lighten dental restorations, creating color mismatches. Understanding these mechanisms will help you maintain your whitening results more effectively.
Key Takeaways
- Enamel rehydration after treatment causes slight darkening called shade relapse as teeth absorb moisture and return to normal hydration levels.
- Whitening creates temporary enamel porosity that allows tannins from coffee, tea, and dark foods to penetrate and restain teeth.
- Intrinsic stains from tetracycline, fluorosis, or trauma resist whitening agents and become more apparent after surrounding enamel lightens.
- Pre-existing enamel defects and thin spots become more visible post-whitening as underlying yellow dentin shows through bleached areas.
- Dental restorations like fillings and crowns cannot whiten, creating color mismatches when surrounding natural teeth lighten and fade.
Temporary Dehydration Effects That Cause Color Rebound
Whitening treatments trigger a predictable dehydration response in your enamel that directly influences the color changes you observe. When carbamide peroxide or hydrogen peroxide penetrates your enamel, it displaces natural water and increases internal tooth temperature, creating temporary moisture loss.
This dehydration makes your teeth appear dramatically whiter initially because dehydrated enamel reflects light differently and looks more porous.
The tooth rehydration process begins immediately after treatment, with moisture gradually returning over several days to one week. As your enamel rehydrates, you’ll notice slight darkening—called shade relapse—where your teeth settle to a color brighter than baseline but darker than the immediate post-treatment shade.
While long term dehydration effects can include increased cavity risk, proper rehydration through adequate water intake prevents complications and stabilizes your whitening results.
Intrinsic Stains That Resist Whitening Treatments
Several distinct factors create intrinsic stains that originate deep within your tooth structure rather than on the enamel surface. Tetracycline antibiotics taken during tooth development cause bluish-gray discoloration that resists standard whitening protocols due to medication effects on dentin.
Excessive fluoride exposure leads to dental fluorosis, creating white or brown spots that block chemical lightening agents. Genetic predisposition determines your dentin thickness and natural color, making some teeth inherently darker regardless of bleaching attempts.
Dental trauma disrupts internal tooth structure, producing persistent gray or brown shades. These intrinsic stains resist whitening because they’re embedded within dentin layers where external peroxide can’t effectively penetrate. Alternative treatments include porcelain veneers, internal whitening procedures, or walking bleach techniques that address discoloration from inside the tooth structure.
New Surface Stains From Food and Beverages
While intrinsic stains originate from within the tooth structure, you’ll face a different challenge immediately after whitening treatments: your teeth become highly susceptible to new surface discoloration. The bleaching process creates temporary porosity in your enamel, opening microscopic channels that remain vulnerable for approximately 48 hours.
During this critical window, tannins from coffee and tea bind directly to exposed enamel surfaces, while acidic beverages like wine and soda weaken your enamel’s protective barrier. Dark-colored foods—berries, tomato-based sauces, and spices like turmeric—deposit chromogens into these unseen microfissures. Even genetic enamel defects can intensify staining patterns during this period.
You can protect your results by avoiding pigmented foods and acidic drinks, then rinsing immediately after any potential exposure to prevent permanent discoloration.
Pre-Existing Enamel Defects Becoming More Visible
Whitening treatments can expose enamel defects you’ve had for years but never noticed until the surrounding tooth structure lightens. Areas with thinner enamel allow the underlying yellow dentin to show through more prominently, while fluorosis spots and decalcification marks become starkly visible against your newly whitened teeth.
This contrast effect occurs because the whitening agent lightens healthy enamel more effectively than compromised areas, making pre-existing structural irregularities appear as white spots, streaks, or patches.
Thin Enamel Reveals Dentin
When enamel thins naturally or through wear, it becomes more translucent and allows the underlying dentin—a naturally yellow tissue—to show through more prominently. Whitening treatments remove surface stains from your enamel, which paradoxically can make this yellow undertone more noticeable if your enamel is already compromised.
The bleaching process causes temporary enamel dehydration, further increasing translucency and dentin visibility immediately after treatment. You’ll notice this effect particularly along tooth edges and worn surfaces where enamel is thinnest.
If you’re experiencing unexpected yellowing post-whitening, it likely indicates pre-existing enamel thinning rather than treatment failure. A professional assessment can determine your enamel thickness and help you develop appropriate whitening strategies that account for your tooth structure, potentially including alternative approaches that won’t emphasize underlying dentin.
Fluorosis and White Spots
Pre-existing enamel defects like dental fluorosis and white spots often become strikingly more visible after whitening treatments, creating an unexpected cosmetic concern for patients who anticipated uniform brightening. Fluorosis develops from excess childhood fluoride exposure, causing enamel hypomineralization that appears as white lines or patches.
These defects differ fundamentally in chromophoric chemical composition from surface stains—they’re structural enamel formation abnormalities, not discoloration. Whitening agents lighten surrounding enamel while hypomineralized areas remain unchanged, dramatically increasing contrast. Dehydration from bleaching further amplifies this visibility.
Fluorosis severity assessment before treatment helps determine appropriate interventions. Moderate to severe cases typically require alternatives: enamel microabrasion removes thin surface layers, composite bonding covers spots directly, porcelain veneers conceal imperfections, or resin infiltration addresses persistent concerns. Standard bleaching proves ineffective on these developmental defects.
Decalcification Highlighted by Whitening
Similar to fluorosis, decalcification creates pre-existing enamel defects that become strikingly apparent following whitening procedures—but unlike developmental fluorosis, these mineral-deficient areas result from post-eruption acid exposure rather than formation abnormalities.
You’ll notice these white patches emerge when bacterial acids from poor hygiene, acidic foods, or discolored plaque buildup weaken your enamel’s mineral structure. The bleaching process highlights these defects by lightening surrounding healthy enamel while mineral-deficient zones remain unchanged, creating stark contrast.
Hydrogen peroxide temporarily dehydrates your enamel, exaggerating mineral loss patterns as patchy streaks. Your dentist can identify decay-related demineralization before treatment and recommend targeted fluoride therapy afterward.
These spots typically fade within days as your enamel rehydrates and remineralizes, though addressing underlying hygiene practices prevents recurrence.
Dental Restorations That Remain Unchanged
Unlike natural teeth, dental restorations such as crowns, bridges, veneers, and fillings won’t respond to whitening treatments due to their fundamental material composition. The porcelain, ceramic, and resin materials used in these restorations are nonporous and engineered to resist degradation, creating material incompatibility with hydrogen peroxide-based bleaching agents.
Key characteristics of restorations during whitening:
- Whitening agents can’t penetrate the nonporous surfaces of dental work
- Restorations maintain their original shade permanently, regardless of treatment duration
- Natural teeth may lighten several shades while adjacent restorations remain unchanged
- Color instability becomes apparent as whitened natural teeth create visible contrast with darker restorations
- Replacement after whitening is necessary to achieve uniform color across your smile
You’ll need to wait at least two weeks post-whitening before replacing visible restorations for ideal shade-matching results.
Age-Related Enamel Thinning and Dentin Exposure
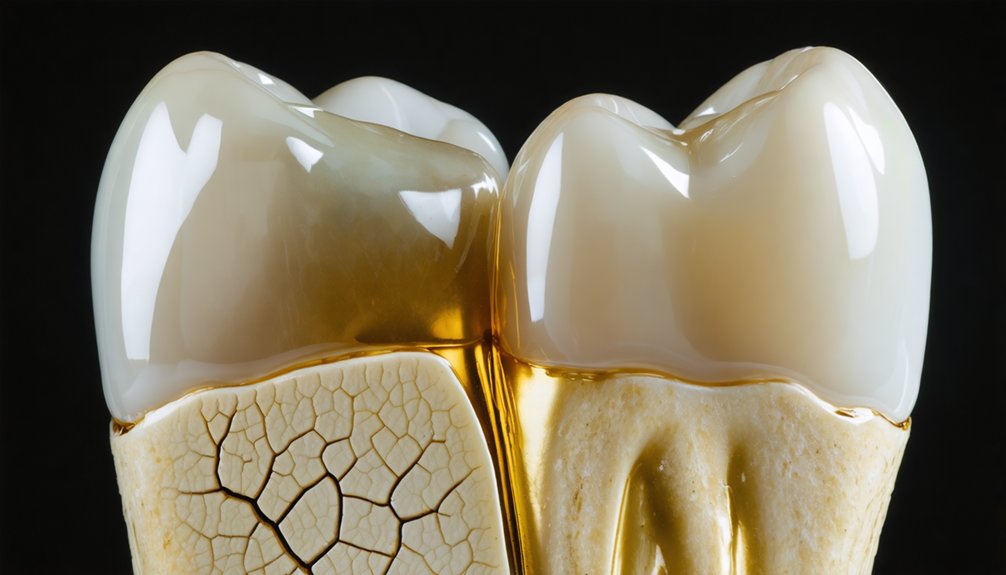
Your natural tooth structure undergoes progressive deterioration that fundamentally affects whitening outcomes, particularly as you age. As enamel wears from acidic exposure, grinding, and decades of use, it reveals the yellowish dentin beneath. This thinning creates a critical challenge: whitening treatments brighten surface enamel but can’t alter dentin’s inherent color. When dentin shows through thinned or cracked enamel, yellowing persists despite treatment.
Age compounds this issue through enamel permeability changes—mineral deposits from saliva reduce ion exchange, making enamel less responsive to whitening agents. Simultaneously, dentin mineral deposition increases brittleness and alters color properties. Gum recession and aggressive brushing accelerate dentin exposure, while acid reflux erodes remaining enamel. These structural changes explain why your teeth may yellow rapidly post-whitening, as underlying dentin color dominates your tooth’s appearance.
Poor Oral Hygiene Accelerating Discoloration
When whitening treatments conclude, your oral hygiene practices immediately determine how long results persist. Inconsistent homecare habits create conditions where stains cling to dental plaque, causing patchy yellowing within weeks. The progression of plaque buildup harbors pigments from coffee, tea, and wine while producing acid that weakens enamel integrity.
Your whitening results face these hygiene-related threats:
- Porous enamel in the first 24-48 hours post-treatment rapidly absorbs pigments from staining agents
- Plaque accumulation from irregular brushing creates uneven surface dehydration and blotchy discoloration
- Bacterial acid production from poor hygiene weakens enamel, accelerating stain penetration
- Decalcification causes mineral loss areas that appear as white spots after whitening
- Interdental neglect from inadequate flossing leaves areas vulnerable to rapid reaccumulation
Trauma-Induced Internal Pigmentation
If you’ve experienced dental trauma from a fall, sports injury, or accident, internal damage to your tooth’s pulp can cause persistent discoloration that whitening treatments can’t address. The injury disrupts blood vessels within the tooth, leading to internal bleeding that deposits pigments directly into the dentin layer.
As damaged pulp tissue breaks down, these blood breakdown products create characteristic gray, brown, or yellow stains that originate from within the tooth structure rather than on its surface.
Pulp Damage From Injury
Dental trauma compromises your tooth’s internal structures in ways that profoundly affect whitening outcomes. When injury severs your pulp’s blood supply, necrosis begins—triggering pigment release into dentin that creates characteristic grayish discoloration. You’ll need pulp essentiality assessment through thermal sensitivity analysis before attempting any whitening protocol.
Critical indicators demanding immediate evaluation:
- Throbbing pain post-whitening signals active pulp inflammation or advancing necrosis
- Persistent thermal sensitivity to cold or heat reveals compromised pulp status
- Gray-brown discoloration emerges months after trauma from internal tissue breakdown
- Pain on percussion indicates irreversible pulpitis requiring endodontic intervention
- Radiographic changes confirm pulp death before proceeding with internal bleaching
Dead pulp tissue releases hemoglobin breakdown products that penetrate dentin tubules, creating stains external bleaching can’t address. You’ll require root canal therapy followed by internal bleaching protocols for effective color correction.
Blood Pigments Within Dentin
Following traumatic injury, blood escaping from damaged pulp vessels infiltrates your tooth’s dentinal tubules—initiating a cascade of hemolysis that produces intrinsic discoloration external whitening can’t reverse. These hemoglobin byproducts penetrate deeply within dentin, creating gray, brown, yellow, or black pigmentation that develops over days to months as breakdown progresses.
Standard surface bleaching lacks the penetration depth necessary to address injury induced staining embedded below enamel. You’ll require internal bleaching following root canal therapy, where oxidative agents like sodium perborate paste directly contact affected dentin to break down trapped blood pigments. Combined internal-external approaches maximize chromatic correction.
Early professional assessment within weeks of trauma determines whether discoloration represents temporary bruising or permanent pigmentation requiring intervention. Delayed treatment allows deeper pigment embedding, complicating subsequent removal efforts.
Frequently Asked Questions
How Long Should I Wait Between Professional Whitening Sessions?
You’d think teeth whitening works like coffee—more’s better, right? Wrong. You should wait 6-12 months between professional sessions to prevent enamel damage. Consult your dentist for personalized recommendations that minimize time between whitening sessions while protecting your teeth.
Can Whitening Toothpaste Prevent Discoloration After Professional Treatments?
Yes, you’ll maintain professional results by using whitening toothpaste with alternative whitening agents like sodium hexametaphosphate. However, dietary influence on discoloration remains significant—you must limit coffee and chromogenic foods for ideal long-term color stability.
Do Teeth Whitening Strips Cause the Same Rebound as Professional Treatments?
Like a fading photograph, strips cause less dramatic rebound than professional treatments due to lower concentrations. However, you’ll experience similar discoloration from improper application techniques or excessive whitening use, requiring careful adherence to manufacturer protocols for ideal outcomes.
Will Drinking Through a Straw Reduce Staining After Whitening?
Yes, you’ll reduce staining if straw use frequency targets high-risk beverages during the 48-hour vulnerable period. Straw placement effects depend on positioning liquid past anterior teeth, minimizing contact with porous enamel surfaces where pigments absorb most readily.
Are Some Teeth Naturally Too Yellow to Whiten Effectively?
No teeth are naturally too yellow to whiten, but enamel discoloration factors like intrinsic staining from tetracycline limit effectiveness. You’ll need professional treatments addressing teeth sensitivity concerns to achieve ideal results with severely discolored teeth.