Your teeth resist whitening when stains penetrate deep into the enamel or originate from inside the tooth structure itself. Medications like tetracycline antibiotics, excessive fluoride, and physical trauma create intrinsic discoloration that surface treatments can’t reach. Additionally, eroded enamel from overusing whitening products makes your teeth resistant to further brightening. Your genetic blueprint, natural aging processes, and saliva composition also determine how well your teeth respond to whitening treatments. Understanding these specific factors will help you identify the most effective solutions for your situation.
Key Takeaways
- Deep-set stains penetrate beyond surface enamel into tooth structure, making them unreachable by standard whitening treatments.
- Intrinsic discoloration from medications like tetracycline antibiotics creates permanent internal staining that whitening agents cannot address.
- Eroded or thinned enamel from overuse of whitening products becomes resistant and unable to hold whitening results effectively.
- Genetic factors determine natural tooth color, enamel thickness, and dentin hue, limiting individual whitening potential.
- Aging causes enamel wear and dentin exposure, creating discoloration that conventional whitening methods struggle to improve.
Deep-Set Stains That Penetrate Beyond Surface Enamel
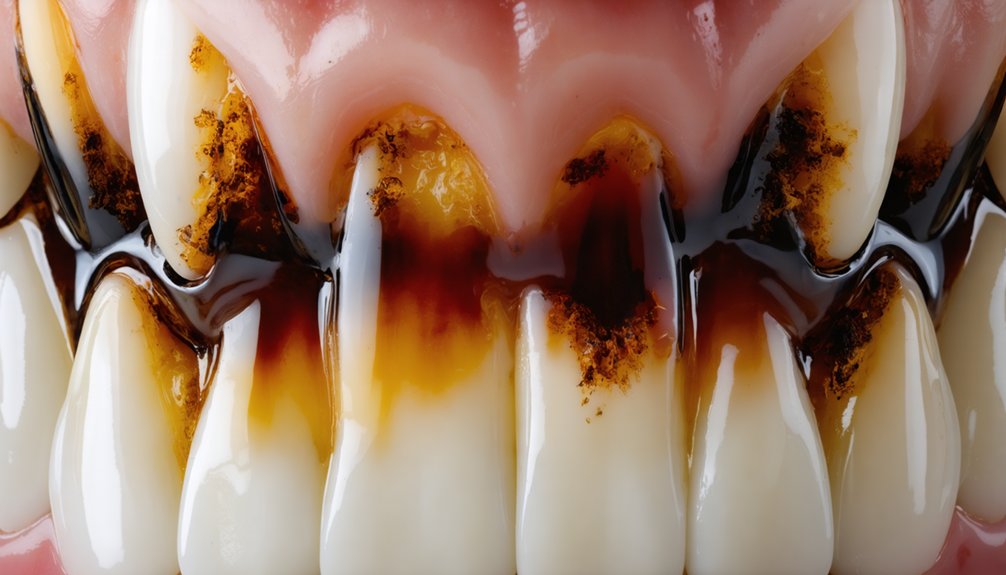
The most stubborn tooth discoloration begins as surface stains but doesn’t stay there. When you consume coffee and tea staining compounds or pigment rich food and drink, particles initially adhere to microscopic textures in your enamel.
Tooth stains start on your enamel’s surface but quickly penetrate deeper when pigmented particles from foods and beverages aren’t promptly removed.
Without daily removal through proper brushing and flossing, these particles gradually penetrate deeper into your tooth structure. This migration transforms what started as extrinsic discoloration into set-in stains that resist standard whitening approaches.
The depth of penetration directly determines which treatments will prove effective for your situation. Surface-level stains respond well to at-home products, but once discoloration works its way through your enamel layer, you’ll need stronger interventions.
Understanding this progression helps you recognize when professional evaluation becomes necessary rather than continuing ineffective over-the-counter treatments.
Intrinsic Discoloration Originating Inside Tooth Structure
When discoloration develops from within your tooth structure rather than on its surface, traditional whitening treatments often can’t reach deep enough to create noticeable change. Medications like tetracycline antibiotics taken during childhood, dental trauma that damages internal tooth tissue, and natural changes in your dentin layer all create intrinsic stains that resist conventional bleaching methods.
Understanding these internal causes helps explain why your teeth may not respond to over-the-counter whitening products designed only for surface stains.
Medication-Induced Internal Staining
Unlike surface stains that develop from coffee or wine, certain medications can permanently discolor your teeth from the inside out. Tetracycline antibiotics taken during childhood (ages 4 months to 7 years) produce bluish-gray enamel that whitening treatments can’t reach. Medication dosage effects matter greatly—higher doses increase staining severity.
Iron supplements create dark brown discoloration, while excessive fluoride causes dental fluorosis with characteristic brown patches. Even minocycline and doxycycline react with your tooth proteins, creating oxidation stains. Antihistamines like Benadryl reduce saliva production, allowing bacterial buildup that worsens intrinsic staining.
Your dentist can identify medication-induced discoloration during examination. While dental fluoride treatments prevent decay, excessive amounts during tooth development cause permanent staining. Understanding these medication risks helps you make informed decisions about treatment alternatives when tooth development occurs.
Trauma Causes Tooth Darkening
Physical trauma to your teeth triggers internal bleeding that standard whitening treatments simply can’t address. When blood vessels rupture inside your pulp chamber during an accident or sports injury, trapped blood darkens your tooth structure from within, turning it gray, brown, or dark yellow as hemoglobin breaks down.
Nerve death from severe trauma creates particularly stubborn tissue discoloration. Dead pulp tissue naturally darkens as cellular breakdown products accumulate, producing gray discoloration that resists external whitening methods. Fractures from impact also expose deeper tooth layers, allowing stains to penetrate beyond enamel’s protective barrier.
Childhood trauma presents additional concerns—damage to developing tooth buds can permanently discolor adult teeth before they even emerge. This developmental disruption creates lifelong discoloration requiring specialized internal whitening procedures or cosmetic restoration.
Dentin Layer Color Changes
Your tooth’s inner dentin layer can develop permanent discoloration that no amount of surface whitening will fix. Unlike surface stains, these intrinsic changes originate deep within your tooth structure, making them particularly resistant to conventional bleaching treatments.
Common causes of dentin discoloration include:
- Tetracycline antibiotics taken before age 8, which bind to calcium during tooth development and create gray, brown, or yellow bands
- Excessive fluoride exposure during formation, causing hypomineralization with white flecks or brown patches
- Developmental disruptions from systemic diseases like celiac disease or metabolic disorders that alter dentin composition
- Failed root canal treatments where endodontic materials, silver points, or necrotic tissue penetrate and stain surrounding dentin
- Inherited enamel defects that expose underlying yellowish dentin and accelerate age-related darkening
These conditions require specialized interventions beyond standard whitening protocols.
Enamel Erosion and Structural Damage
The aggressive pursuit of whiter teeth can paradoxically create the very problems that make further whitening ineffective. When you engage in overuse of whitening products, you’re gradually eroding your enamel—the protective outer layer that whitening agents need to work properly. Research demonstrates significant erosion differences across treatments (F(9,50) = 25.19; p < 0.0001), with frequent bleaching depleting calcium and creating brittleness.
This damage to your underlying enamel structure makes teeth increasingly resistant to whitening. Thinned, porous enamel can’t hold whitening results effectively, and you’ll notice a disappointing rebound effect within 24-48 hours. Pre-existing cracks or cavities worsen this cycle. Since weakened enamel can’t regenerate, moderation becomes essential—allowing 7-day remineralization periods between treatments helps restore your enamel’s microhardness to normal levels.
Genetic Factors and Natural Aging Processes
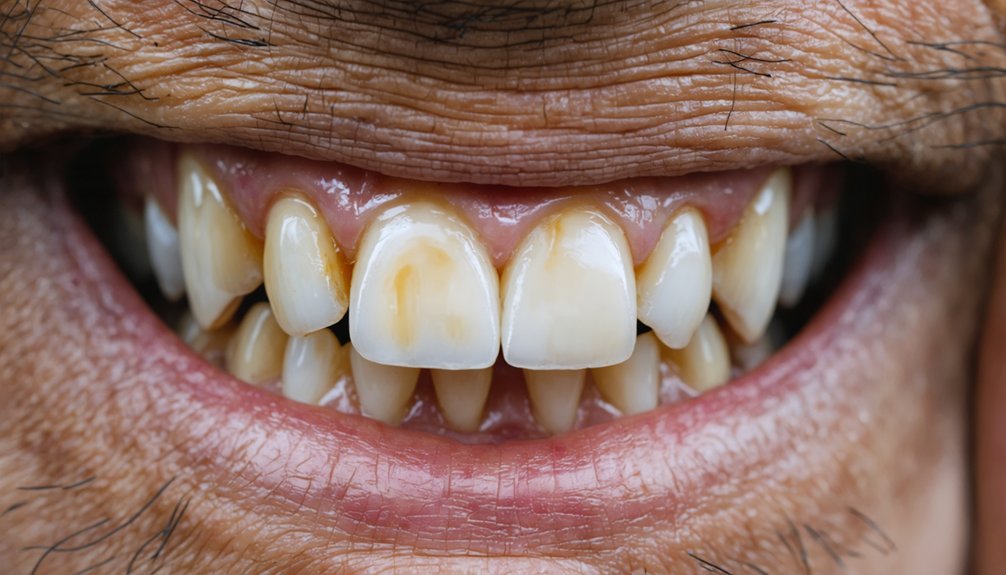
While you might assume all teeth respond equally to whitening treatments, your genetic blueprint markedly determines both your natural tooth color and how successfully bleaching agents can lighten it. Your inherited dental traits control enamel thickness, dentin hue, and structural composition—factors that directly impact stain resistance and whitening outcomes.
Key genetic factors affecting whitening success:
- Enamel thickness: Thinner hereditary enamel reveals yellowish dentin underneath, creating discoloration resistant to surface treatments
- Dentin color variation: Your genetically-determined dentin ranges from yellow to gray, influencing overall tooth shade
- Saliva composition variations: Inherited pH levels and consistency affect how whitening agents interact with tooth surfaces
- Aging acceleration: Genetic factors control enamel wear rates and dentin exposure speed
- Hereditary conditions: Amelogenesis imperfecta and dentinogenesis imperfecta create intrinsic stains unresponsive to conventional whitening
Medication-Induced Stains From Childhood
Certain medications taken during childhood can permanently embed themselves into developing teeth, creating intrinsic stains that resist conventional whitening treatments. Tetracycline antibiotics represent the most notorious culprits, causing discoloration in 23-92% of children under 8 when incorporated during tooth development. These medications bind to calcium in forming enamel, creating gray-brown stains and antibiotic induced enamel hypoplasia that penetrate deep within tooth structure.
Tigecycline produces similar permanent effects, with studies showing 16.7% of treated children developing yellow discoloration. You’ll find macrolide antibiotics like azithromycin and clarithromycin cause macrolide suspension discoloration, though these stains typically remain superficial and removable through professional cleaning. Understanding your medication history helps determine whether your stains originate from childhood drug exposure, guiding appropriate treatment selection beyond standard whitening approaches.
Fluorosis and Excessive Fluoride Exposure
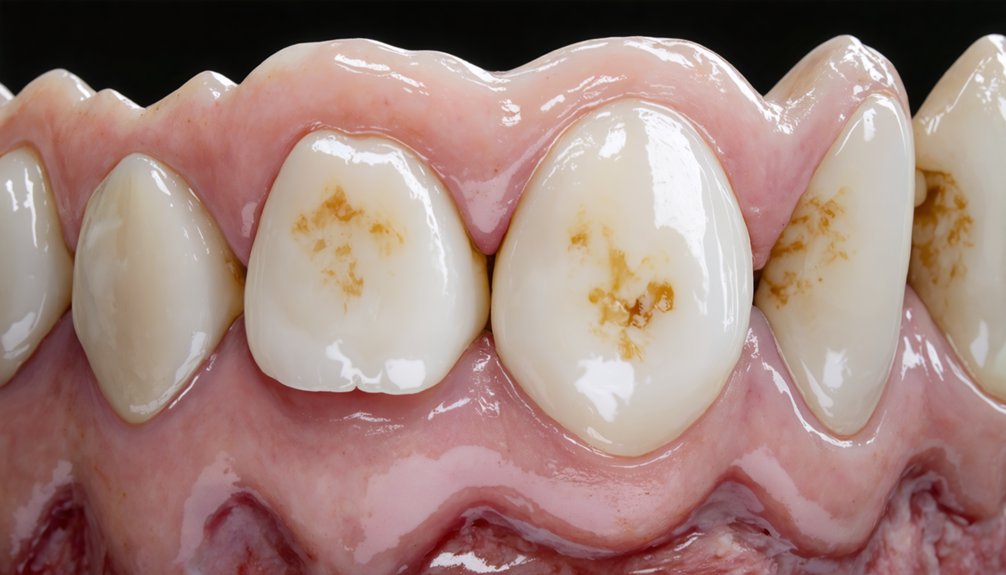
- Bleaching dehydrates teeth, making white or brown fluorosis spots more visible rather than less
- Structural enamel porosity extends deep to the dentino-enamel junction in severe cases
- Peroxide-based treatments can’t reverse developmental mineralization defects
- Vigorous brushing and standard whitening agents fail against fluorosis-induced blemishes
- Temporary improvements require renewal every 3-5 years, making it an impractical long-term solution
Tobacco-Related Nicotine and Tar Buildup
When you smoke or use tobacco products, nicotine penetrates deep into your enamel’s porous structure, creating yellow-brown discoloration that resists standard whitening treatments.
Tar compounds the problem by forming sticky bonds with your tooth surface and existing plaque, creating stubborn deposits that can turn nearly black over time. These dual staining agents work together—nicotine absorbing into subsurface layers while tar adheres externally—making tobacco-related discoloration among the most challenging to reverse.
How Nicotine Penetrates Enamel
As nicotine enters your mouth during smoking, it undergoes a chemical transformation that permanently marks your teeth. The colorless nicotine oxidizes through air exposure and oral enzymes, turning yellow and binding to your enamel’s surface. Within weeks of regular smoking, this oxidized substance infiltrates your porous enamel structure, creating intrinsic stains that resist standard whitening treatments.
The penetration depth extends beyond surface coating, making removal exceptionally challenging. This process simultaneously causes enamel degradation—reducing microhardness by up to 46.81% while disrupting the crystalline structure and depleting essential minerals like calcium and phosphorus.
Key penetration mechanisms include:
- Oxidation converts nicotine from colorless to yellow adherent substance
- Porous enamel structure allows deep intrinsic stain formation
- Microhardness reduction creates vulnerable, weakened surfaces
- Mineral depletion decreases calcium-to-phosphorus ratios
- Crystalline structure damage increases discoloration susceptibility
Tar’s Stubborn Bonding Properties
While nicotine oxidation creates the foundation for tooth discoloration, tar’s unique physical properties make these stains remarkably persistent. You’re dealing with a substance whose adhesive qualities enable it to bond tightly to your enamel surfaces, forming deep yellow-brown discolorations that resist standard whitening methods.
Tar’s penetration properties worsen as it seeps into your tooth’s natural pores, creating intrinsic stains beneath the surface. When combined with plaque and tartar buildup, you’re facing multi-layered deposits that shield staining particles from removal. Research shows cigarette tar produces significant color changes (∆E MD: 16.22), far exceeding heated tobacco products.
You’ll find over-the-counter treatments inadequate against this deep penetration. Professional cleaning every six months, combined with quitting smoking, offers your most effective path forward.
Pre-Existing Dental Conditions and Decay
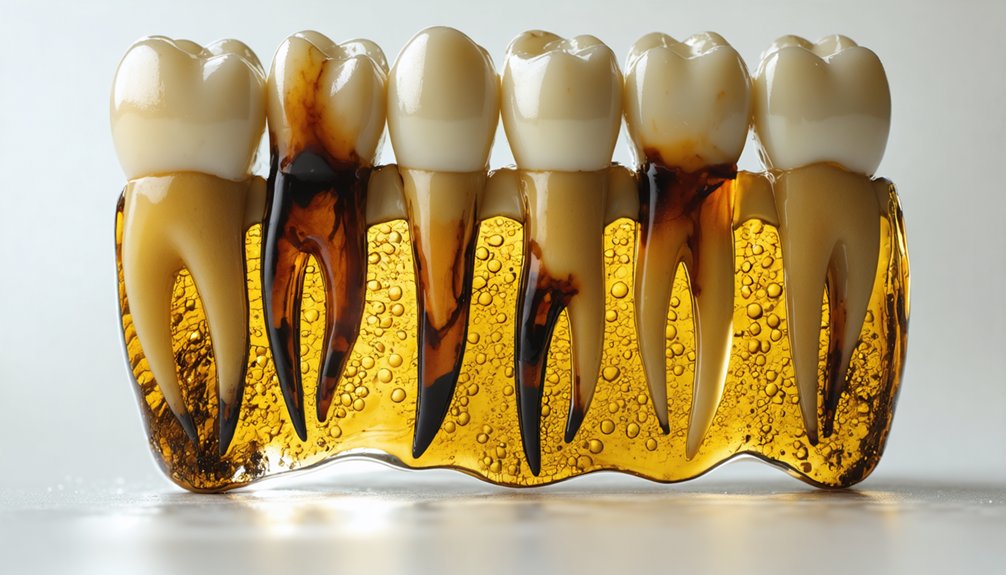
Before you pursue teeth whitening, your dentist needs to address any underlying dental conditions that could sabotage your results. Inadequate oral hygiene and improperly treated dental conditions create significant barriers to successful whitening outcomes.
Your existing dental issues directly impact whitening effectiveness:
- Untreated cavities allow whitening agents to penetrate decay, causing severe sensitivity while yielding poor color correction
- Periodontal disease intensifies gum inflammation when exposed to peroxide-based products, worsening your condition
- Eroded enamel exposes yellowish dentin that resists whitening attempts and increases penetration depth
- Pre-existing sensitivity affects 30-78% of whitening patients, requiring desensitizing fluoride pre-treatment
- Decayed tooth structure prevents uniform whitening and creates uneven, disappointing results
Professional evaluation verifies you’ve resolved these conditions before investing in whitening treatments, protecting both your oral health and treatment investment.
Dental Restorations That Don’t Respond to Whitening
Even after treating underlying dental conditions, your existing restorations won’t respond to whitening treatments the way natural teeth do. The restoration material composition—whether porcelain, zirconia, or composite resin—resists hydrogen peroxide penetration due to its non-porous structure. While your natural teeth lighten, crowns, veneers, and fillings maintain their original shade, creating noticeable color mismatches.
Restoration age considerations matter when planning whitening. Older restorations typically require replacement after treatment to match your newly whitened teeth. You’ll achieve ideal results by whitening first, then placing new restorations to match your lighter shade. However, aggressive high-concentration bleaching can damage composite materials and glass ionomer cements. Consult your dentist to assess your specific restorations and develop a strategic whitening plan that addresses both natural teeth and restoration replacement timing.
Frequently Asked Questions
Can Professional Whitening Treatments Damage Teeth That Are Already Weakened?
Yes, they absolutely can wreak havoc on your weakened teeth! Professional whitening causes potential tooth sensitivity and compromises enamel integrity when you’ve got pre-existing erosion. You’ll need a thorough dental assessment first to protect your vulnerable teeth from permanent damage.
How Long Should I Wait Between Whitening Attempts for Resistant Stains?
For resistant stains, you’ll need longer treatment intervals of 2-4 weeks between attempts, with increased application duration monitored by your dentist. This evidence-based spacing prevents enamel damage while maximizing whitening effectiveness for stubborn discoloration.
Are There Dietary Changes That Improve Whitening Treatment Effectiveness?
Ironically, dietary habits won’t boost whitening effectiveness—your teeth composition determines treatment response. However, you’ll protect results by choosing crunchy vegetables, dairy, and lean proteins while avoiding staining foods. Control what you can: maintenance, not enhancement.
Do Whitening Toothpastes Work Differently Than Professional Treatments for Stubborn Stains?
Yes, whitening toothpaste ingredients only scrub surface stains through abrasion, while professional treatments penetrate enamel with concentrated peroxide. Home whitening kit effectiveness falls between—they’re stronger than toothpaste but can’t match professional-grade bleaching for stubborn discoloration.
What Alternative Cosmetic Procedures Exist for Teeth That Won’t Whiten?
You’ve got options beyond ye olde whitening! Dental veneers cover resistant stains permanently, while enamel microabrasion removes superficial discolorations. Bonding and crowns also restore stubborn teeth, giving you complete control over your smile’s appearance.