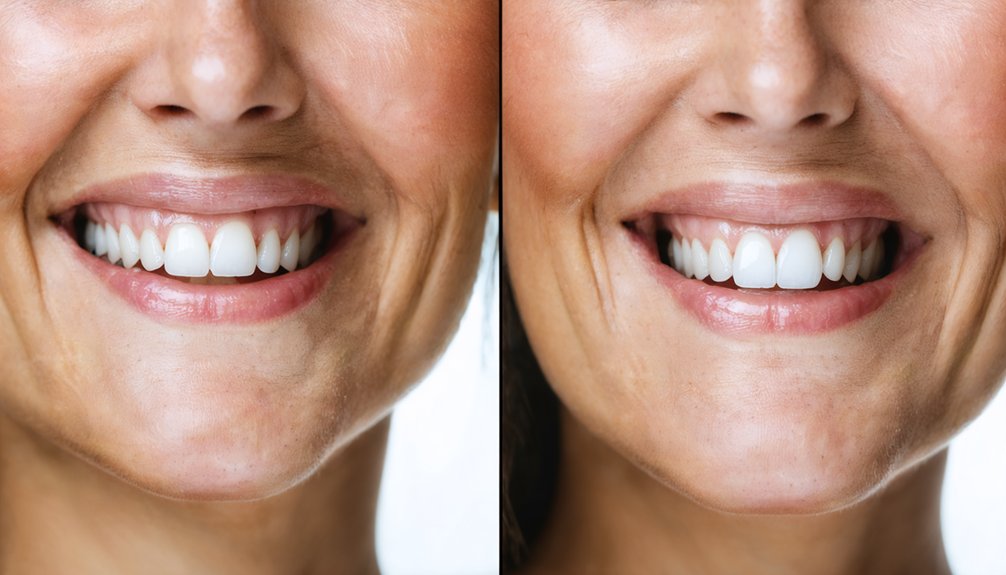
Your aging teeth darken as enamel thins and dentin shifts toward grayish-yellow tones, but you can reverse this through professional bleaching (15-40% hydrogen peroxide) or at-home treatments (10-16% carbamide peroxide). In-office protocols deliver 7-8 shade improvements in single visits, while custom trays provide gradual results over two weeks. You’ll need modified protocols if you’re experiencing enamel thinning or heightened sensitivity. This thorough guide explores ideal whitening strategies, sensitivity management, and maintenance protocols tailored specifically for mature dental structures.
Key Takeaways
- Aging teeth darken as enamel thins, dentin yellows, and chromogenic substances from coffee, tea, and tobacco penetrate weakened tooth surfaces.
- Professional in-office bleaching with 15-40% hydrogen peroxide delivers 7-8 shade improvements in one visit with light-activated technology.
- At-home options include custom trays with prescription-strength gel, whitening strips, and toothpastes for gradual results over two weeks.
- Older adults require lower peroxide concentrations and desensitizing agents to manage sensitivity from thinning enamel and exposed dentin tubules.
- Maintain results through biannual cleanings, professional touch-ups every 6-12 months, and minimizing exposure to staining beverages with straws.
Understanding Why Teeth Darken With Age
Why do teeth inevitably lose their youthful brightness as decades pass? Your enamel microstructure changes progressively through mechanical wear, calcification, and increased porosity, exposing the inherently yellowish dentin beneath. This structural degradation occurs regardless of meticulous oral hygiene.
Despite flawless brushing habits, enamel inevitably thins with age, revealing the yellow dentin layer underneath through structural breakdown beyond your control.
Simultaneously, your dentin naturally darkens with age, shifting toward grayish-yellow tones while the pulp chamber contracts through fibrosis and mineralization. These intrinsic transformations alter light refraction properties within tooth layers.
Extrinsic factors compound this process: chromogenic substances from coffee, tea, wine, and tobacco penetrate thinned enamel, embedding pigments deeply. Acidic exposure facilitates stain adhesion by temporarily softening enamel surfaces. Additionally, genetic tooth pigmentation factors determine baseline coloration and susceptibility to discoloration.
Understanding these multifactorial mechanisms enables you to implement targeted interventions that address both structural deterioration and accumulated staining effectively.
How Different Whitening Methods Work
You’ll encounter three primary categories of whitening methods when addressing age-related tooth discoloration: professional in-office bleaching systems utilizing high-concentration hydrogen peroxide, at-home options employing custom trays with carbamide peroxide gels, and light-activated gel technologies that combine chemical bleaching with LED or violet light exposure.
Each approach operates through distinct mechanisms with varying concentrations of peroxide compounds, application durations, and delivery systems. Understanding these differences enables you to select the most appropriate intervention based on your specific discoloration pattern, sensitivity tolerance, and treatment timeline expectations.
Professional In-Office Bleaching Systems
Professional in-office bleaching systems deliver concentrated hydrogen peroxide formulations ranging from 15% to 40%, substantially higher than over-the-counter alternatives, to achieve rapid tooth lightening in a single clinical visit. Pre-treatment preparations include thorough cleaning and examination, followed by gum isolation using protective barriers.
Leading systems include Philips Zoom! (25% peroxide with blue light activation), Opalescence (40% hydrogen peroxide with desensitizing agents), and BriteSmile (15% peroxide at neutral pH). Each treatment cycle applies gel for 15-20 minutes, with multiple rounds producing results up to eight shades whiter.
Clinical evidence demonstrates outcomes equivalent to extended at-home protocols (p=0.95), though delivered within 60-90 minutes. Maintenance procedures guarantee color stability exceeding one year. Higher concentrations correlate with superior efficacy despite mixed data on light-activation benefits.
At-Home Whitening Options
While professional treatments deliver rapid results, at-home whitening options provide accessible alternatives with varying efficacy profiles suited to different clinical needs and patient compliance patterns.
You’ll find whitening toothpastes utilize mild abrasives for surface stain removal with minimal risk, requiring consistent application for gradual effects. Whitening strips deliver medium effectiveness through peroxide-based gels applied for 30 minutes daily, though they may produce uneven coverage on irregular dental surfaces.
Over-the-counter trays offer cost-effective solutions with lower peroxide concentrations, yet inconsistent fit compromises results. Dentist-dispensed take-home kits provide superior outcomes through custom trays containing 15-16% hydrogen or carbamide peroxide, worn 15-20 minutes daily. These prescription-strength formulations incorporate desensitizing agents like potassium nitrate, ensuring effective usage techniques and product application guidance for ideal whitening control.
Light-Activated Gel Technology
Light-activated whitening systems harness specific wavelengths to catalyze peroxide-based bleaching agents, accelerating the oxidation reactions that break down chromophore molecules within tooth enamel. You’ll find that LED light performance factors—including wavelength specificity, intensity levels, and exposure duration—directly impact treatment efficacy. Clinical studies demonstrate shade improvements of 4.8 units with photoactivation versus 3.8 units without light enhancement.
Your dentist customizes whitening gel formulations by adjusting hydrogen peroxide or carbamide peroxide concentrations based on your sensitivity threshold and stain characteristics. Professional systems integrate multiple LED bulbs with precise timing mechanisms to guarantee consistent light distribution across tooth surfaces. Research validates that diode lasers, halogen lamps, and LED technology all produce significant color changes, with light source selection proving more critical than bleaching agent choice alone.
Professional In-Office Whitening Options
When enamel discoloration resists over-the-counter treatments, in-office whitening delivers immediate, dramatic results through concentrated peroxide formulations administered under direct dental supervision. Your dentist initiates the protocol with dental prophylaxis, removing plaque and tartar to optimize gel penetration. Gingival protection—liquid rubber dam, hardening resin, or protective gel—shields soft tissues from chemical burns caused by 15-43% peroxide concentrations.
You’ll receive 3-4 application cycles of hydrogen or carbamide peroxide gel, each lasting 10-30 minutes, often activated with LED or UV light. Systems like Philips Zoom! (25% peroxide) and Opalescence (40% peroxide with potassium nitrate) provide customizable intensity levels. The 1-2 hour session produces immediate shade improvement, though final color stabilizes 2-6 weeks post-treatment as dehydration reverses. Post-procedure fluoride application manages transient sensitivity while maximizing retention.
At-Home Whitening Solutions

Between professional treatments, at-home whitening systems provide cost-effective maintenance through lower-concentration peroxide formulas you’ll apply independently over extended periods. Strips and gels containing hydrogen peroxide deliver visible results within two weeks when used 30 minutes twice daily, with effects lasting 5-6 months.
OTC kits utilize carbamide or hydrogen peroxide up to 10% concentration, requiring daily application for 1-2 weeks while monitoring progress via shade guides.
Whitening toothpastes offer gentler alternatives through mild abrasives, suitable for sensitive teeth with gradual improvement over months. Natural alternatives include baking soda-peroxide combinations and activated charcoal, though proper use demands restraint—limit application to once or twice weekly to prevent enamel erosion.
Monthly touch-ups extend results, while consistent maintenance protocols optimize long-term whitening persistence.
Comparing Results: Professional vs. DIY Treatments
Although both professional and at-home whitening systems effectively lighten teeth, they differ markedly in speed, intensity, and clinical outcomes. In-office treatments achieve ΔE values around 3.3 with 40% hydrogen peroxide, delivering 5-8 shades lighter within one hour. At-home systems using 10-16% carbamide peroxide produce ΔE values of 2.0, requiring 2-4 weeks for comparable results.
Professional procedures like Zoom® average 7-8 shades lighter, while Opalescence® Boost yields approximately 4 shades. Your cost benefit analysis should weigh immediate results against treatment investment. Patient preferences typically favor in-office speed and supervision, with 32% of dental procedures involving professional whitening.
Systematic reviews confirm no significant long-term shade differences between methods, though professional treatments guarantee protocol adherence and maintain superior oral hygiene indices (1.33 at one year).
Managing Sensitivity and Side Effects

While whitening treatments deliver impressive aesthetic results, sensitivity remains the most prevalent complication you’ll encounter. Two-thirds of patients using over-the-counter products experience this reaction, with professional treatments affecting up to 78%. You’ll typically notice symptoms peaking within 24 hours, then diminishing over 2-3 days as enamel recovers.
To maintain control, adjust treatment duration based on your tolerance—shorter contact times reduce peroxide penetration into dentin tubules. Incorporate desensitizing agents containing potassium nitrate or fluoride before and after whitening sessions. You’ll minimize risk by avoiding temperature extremes and acidic foods during treatment.
If gum inflammation occurs from gel leakage, rinse immediately with water. Monitor symptoms carefully; persistence beyond one week warrants professional evaluation to rule out underlying conditions like enamel defects or recession.
Special Considerations for Older Adults
As you age beyond 55, physiological changes in your oral structures demand modified whitening protocols to guarantee both safety and efficacy. Your thinning enamel and sensitive gum tissue require lower bleach concentrations, while managing fluoride treatments becomes essential for strengthening compromised tooth structure.
You’ll need comprehensive examination identifying dental conditions like untreated cavities, gum disease, or exposed roots before proceeding. Your existing restorations—crowns, bridges, veneers—won’t respond to whitening agents, necessitating professional assessment for uniform aesthetic outcomes.
With 40% of adults 65+ experiencing significant discoloration from decades of staining, you must establish realistic expectations regarding achievable whiteness levels. Professional supervision allows controlled application, customized concentration adjustments, and coordinated restoration replacement.
Your dentist’s evaluation of enamel thickness, restoration status, and staining patterns determines ideal treatment protocols tailored to your specific dental history.
Maximizing Your Whitening Results
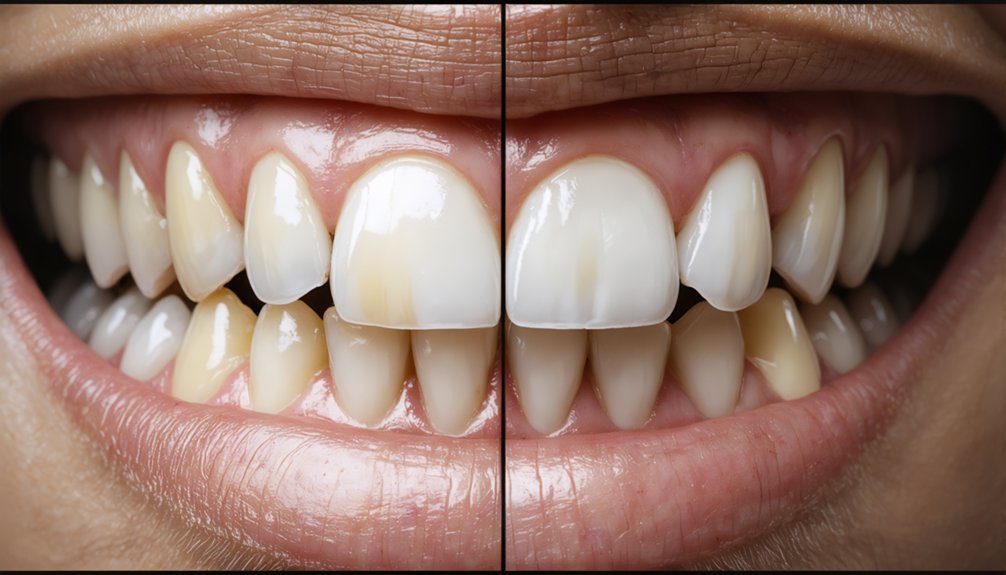
Selecting the ideal peroxide concentration and treatment duration directly determines your whitening outcome‘s magnitude and sustainability. You’ll achieve 7-8 shade improvements through in-office protocols utilizing 35-40% hydrogen peroxide during 30-60 minute sessions, while 10-16% carbamide peroxide home treatments deliver comparable ΔE values of 2.0 over extended periods. Professional systems demonstrate 90% success rates, vastly outperforming OTC alternatives requiring three months for minimal improvement.
Your best treatment schedule combines two in-office sessions spaced one week apart, followed by monthly home bleaching for three months—this regimen extends color persistence beyond six months. Personalized whitening recommendations must account for your initial tooth color, discoloration etiology, and sensitivity threshold. Strategic concentration adjustments reduce sensitivity incidence while maintaining efficacy, ensuring sustained results influenced by oral hygiene compliance, dietary modifications, and smoking cessation.
Keeping Your Smile Bright Long-Term
Your whitening investment requires systematic maintenance protocols to preserve treatment outcomes beyond initial results. Stain prevention demands proactive dietary modifications and consistent oral hygiene execution to protect enamel integrity.
Implement these evidence-based strategies for avoiding discoloration:
- Utilize straw delivery systems when consuming darkly pigmented beverages—coffee, red wine, cola—minimizing anterior tooth surface contact
- Execute immediate water rinses following staining food exposure such as berries, tomato-based sauces, and soy products
- Schedule biannual professional cleanings to eliminate tartar accumulation and surface deposits beyond home care capabilities
- Apply professional-grade maintenance treatments every 6-12 months based on lifestyle factors and shade monitoring
Monitor enamel response carefully. Alternate whitening toothpaste with fluoride formulations to balance stain removal against enamel preservation. Strategic touch-up protocols sustain results for extended durations while minimizing sensitivity risks and maintaining structural tooth integrity.
Frequently Asked Questions
Can Whitening Damage Dental Crowns, Veneers, or Implants in Older Patients?
No, whitening won’t damage your crowns, veneers, or implants—structurally they’re safe, chemically they’re resistant, functionally they’re unaffected. However, you’ll experience potential teeth discoloration mismatches and possible sensitivity after whitening, requiring strategic restoration replacement for ideal aesthetic outcomes.
How Much Does Professional Teeth Whitening Typically Cost for Seniors?
Professional teeth whitening for seniors typically costs $300-$1,000. In-office whitening options range from $400-$800 per session, while dentist-prescribed at-home kits cost $150-$600. Unfortunately, dental insurance coverage rarely includes cosmetic whitening procedures for aging patients.
Will Whitening Treatments Work on Teeth With Root Canals or Fillings?
Your tooth’s ironic fate: external whitening won’t penetrate root canal discoloration or alter fillings. You’ll need internal bleaching for treated teeth, managing bleaching sensitivity while considering long-term effects. Professional assessment determines your ideal protocol for uniform results.
Are There Health Conditions That Prevent Older Adults From Whitening Teeth?
Yes, several conditions prevent safe whitening. You’ll need treatment first if you have untreated cavities, active gum disease, or severe tooth sensitivity concerns. Additionally, medications causing dry mouth and dietary staining issues require modified whitening protocols for ideal safety.
How Soon After Dental Work Can I Start a Whitening Treatment?
Wondering when it’s safe? You’ll need 7-14 days after composite work, 2-4 weeks following crowns, and 3-4 weeks post-root canal. Whitening schedule considerations and sensitivity concerns vary by procedure, so consult your dentist first.