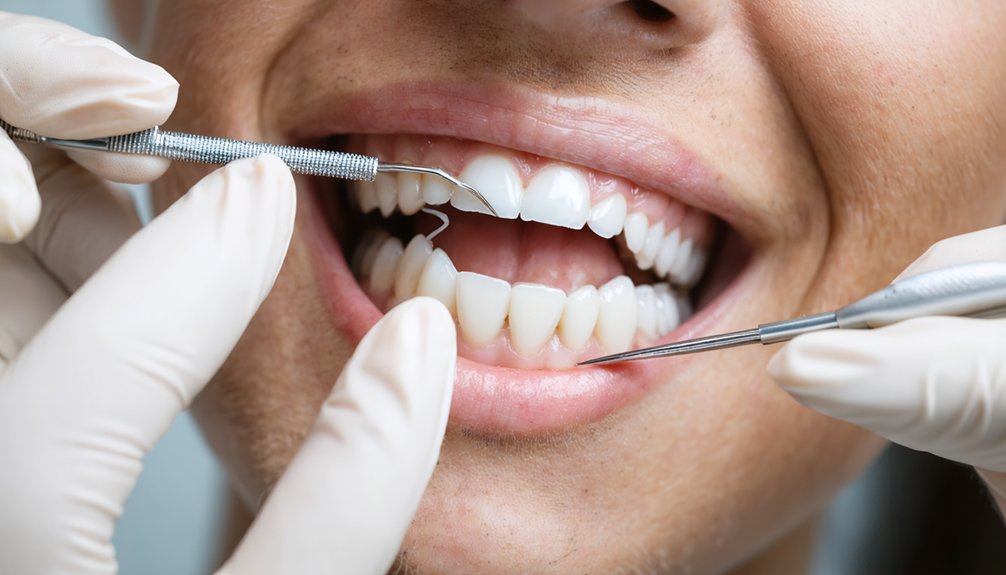
Teeth whitening directly impacts your oral health through both behavioral and chemical pathways. The treatment motivates you to adopt better hygiene practices—studies show 100% of whitening patients add supplementary cleaning products afterward. Chemically, peroxide agents penetrate your enamel to oxidize stain molecules while disrupting plaque formation. However, high-concentration products (25-40% hydrogen peroxide) can damage enamel proteins and trigger tooth sensitivity. Professional-grade treatments deliver superior results while minimizing risks when you select appropriate concentrations and follow evidence-based application protocols that protect your dental structures.
Key Takeaways
- Teeth whitening motivates improved oral hygiene habits, with 100% of patients adopting supplementary products and 94.2% maintaining enhanced brushing routines.
- Peroxide-based whitening agents require pre-treatment plaque removal, which establishes better conditions for oral health and prevents bacterial reformation.
- Professional-strength whitening significantly improves hygienic index scores, dropping from 2.34 to 1.33 within one year after treatment.
- High-concentration peroxide products can cause enamel degradation, demineralization, and pulp cell damage if not properly monitored.
- Temporary tooth sensitivity occurs when peroxide penetrates enamel, but can be managed with desensitizing products and adjusted concentration levels.
How Teeth Whitening Encourages Better Oral Hygiene Habits
Teeth whitening serves as a catalyst for improved oral hygiene behaviors, with research demonstrating measurable changes in patient habits following cosmetic dental procedures. You’ll find that 100% of whitening patients adopted supplementary hygiene products post-treatment, compared to 83.3% before, with mouth rinses and interdental brushes becoming routine additions.
This motivation for lifestyle changes extends beyond product use—94.2% maintained enhanced brushing frequency exceeding three minutes twice daily, while 80% eliminated staining beverages from their diets. The hygienic index improved dramatically from 2.34±0.14 to 1.33±0.09 within one year, extensively outperforming the control group’s 2.45 rating.
Your investment in whitening naturally promotes interdental cleaning practices, establishing sustainable behaviors that reduce decay risk and preserve treatment outcomes through consistent plaque management.
The Science Behind Whitening: Breaking Down Stains and Plaque
Understanding the chemical mechanisms behind teeth whitening reveals how peroxide-based agents penetrate your enamel to oxidize chromogenic molecules while simultaneously reducing bacterial plaque. The concentration of active ingredients—whether hydrogen peroxide or carbamide peroxide—directly correlates with treatment efficacy and the depth of stain removal you’ll achieve.
During the whitening process, oxidative reactions break down both extrinsic surface discoloration and intrinsic stains, while the mechanical action of application can disrupt existing plaque biofilm on your tooth surfaces.
How Peroxide Breaks Stains
When you apply whitening products to your teeth, hydrogen peroxide immediately begins breaking down into highly reactive oxygen radicals (H₂O + O₂) that target pigmented stain molecules embedded within your enamel and dentin. These free radicals attack chromogens through oxidation, causing molecular structure changes that render discolored compounds colorless. The process doesn’t alter your tooth’s composition—it specifically decolorizes stain molecules by changing how they filter light.
Peroxide penetration depth depends on concentration and contact time, following Fick’s Law of diffusion. Professional treatments using 35-40% hydrogen peroxide for 15-20 minutes achieve rapid results, while at-home carbamide peroxide formulations (10-22%) require approximately 8 hours to penetrate effectively. Higher concentrations create faster diffusion rates, allowing oxidizing agents to reach deep-seated discoloration at your dentin-enamel interface and throughout your tooth structure.
Plaque Removal During Whitening
Before any whitening treatment can achieve ideal results, your dental professional must perform extensive plaque and calculus removal to eliminate barriers that would otherwise block peroxide penetration. This pre-whitening protocol establishes perfect conditions for chemical agents to access enamel effectively.
Plaque disruption patterns during treatment involve both mechanical and chemical approaches. Abrasive particles in whitening formulations—silica, alumina, and perlite—mechanically dislodge surface deposits while remaining softer than enamel. Tartar elimination effects extend beyond aesthetics, reducing bacterial colonization sites that contribute to cavity formation.
Antiredeposition agents like polyphosphates prevent chromophore reattachment and inhibit plaque reformation post-treatment. This dual mechanism of initial cleaning plus ongoing prevention sustains your whitening outcomes while simultaneously improving overall oral hygiene through biofilm disruption and reduced decay risk.
Concentration Levels and Efficacy
Whitening agent concentration directly determines both treatment speed and final shade improvement you’ll achieve. Professional use dosage contains higher peroxide levels—typically 25-40% hydrogen peroxide or 35-44% carbamide peroxide—enabling dramatic shade changes in fewer sessions. These stronger concentrations produce more free radicals that rapidly oxidize stain molecules within your dentin layer.
At home application guidelines restrict products to 3-10% hydrogen peroxide or 10-22% carbamide peroxide for safety. While lower concentrations require extended treatment periods, they still penetrate enamel’s porous structure to break down chromogens effectively. You’ll achieve 1-2 shade improvements with over-the-counter products versus 3-8 shades professionally.
Carbamide peroxide provides slower, sustained oxygen release compared to hydrogen peroxide’s immediate action. Your exposure duration and concentration level together dictate your whitening endpoint.
Potential Risks of High-Concentration Peroxide Products
High-concentration peroxide products can compromise your oral health through multiple biological pathways that extend beyond surface-level effects. These formulations degrade enamel’s organic protein matrix, induce cellular death in dental pulp tissue, and trigger nerve-mediated pain responses through direct neurotoxic mechanisms.
Understanding these risks helps you make informed decisions about whitening treatments, particularly when concentrations exceed professional oversight thresholds.
Enamel Protein Degradation
Higher concentrations—particularly 35% carbamide peroxide—intensify oxidative stress and protein loss. You’ll experience surface roughening, decreased hardness, and demineralization that makes your teeth susceptible to decay.
The compromised prismatic layer and increased porosity between enamel prisms weaken structural integrity. Over-whitening accelerates these degradative processes beyond your saliva’s natural remineralization capacity, potentially leading to irreversible damage requiring professional intervention.
Dental Pulp Cell Mortality
3. Peroxide diffuses through 3mm dentin layers, reaching vulnerable pulp tissue where oxidative stress reduces cell proliferation and triggers necrosis.
4. Dose-dependent damage occurs across 5%, 10%, and 35% concentrations, with human dental pulp stem cells showing high sensitivity to all protocols.
Understanding these risks helps you avoid irreversible pulp damage requiring costly restorative dental procedures.
Nerve Sensitivity and Toxicity
Beyond cellular death in the pulp, peroxide exposure creates immediate neurological responses that manifest as the most frequently reported complication in whitening treatments. You’ll experience this sensitivity when hydrogen peroxide penetrates enamel, causing dentin permeability changes that expose nerve endings to external stimuli. Higher concentrations—particularly the 40% solutions used professionally—intensify these neural reactions through pH balance disruption within tubules leading to your pulp.
This discomfort typically presents as sharp responses to temperature variations and sweet substances. You can control severity by selecting lower-concentration products (≤3.5% per ADA guidelines) and adhering strictly to recommended exposure times. The 2018 Cochrane review confirms sensitivity resolves after treatment cessation, though you shouldn’t dismiss persistent symptoms—they may indicate excessive peroxide exposure requiring immediate intervention.
Temporary Tooth Sensitivity: What to Expect During Treatment
When undergoing teeth whitening treatment, you’ll likely experience temporary tooth sensitivity as the most common side effect. This occurs when peroxide agents penetrate enamel, exposing dentin tubules and causing nerve inflammation. Addressing preexisting conditions like gum recession or thin enamel before treatment reduces your risk considerably.
Peroxide penetrates enamel and exposes dentin tubules during whitening, triggering temporary sensitivity that resolves faster when preexisting dental issues are treated first.
What to expect during treatment:
- Sensitivity peaks within 24 hours post-treatment, typically resolving within 48 hours
- Professional treatments cause sharper but shorter discomfort than over-the-counter products
- Higher peroxide concentrations (above 6%) increase sensitivity likelihood
- Discomfort manifests when consuming hot, cold, or sweet substances
Managing dentin hypersensitivity involves using desensitizing toothpaste with potassium nitrate, applying fluoride gel, and selecting lower-concentration products. You’ll maintain control by choosing custom-fitted trays and consulting your dentist to adjust peroxide levels based on your tolerance.
Comparing Whitening Methods: Gels, Strips, and Rinses

Selecting among gels, strips, and rinses requires understanding how each method delivers peroxide to your enamel and the trade-offs in effectiveness, convenience, and safety.
Custom tray whitening with 10-16% carbamide peroxide gels achieves ΔE values around 2.0 within 7-14 days, matching professional results with color stability lasting 1-2.5 years. Prescription strength whitening gels offer superior coverage and professional oversight compared to over-the-counter alternatives.
Strips effectively whiten your front 6-8 teeth but require 30-minute daily applications and produce less durable results than tray systems. You’ll need 16 days with strips to match what tray gels accomplish in seven.
Rinses provide the lowest peroxide exposure, minimizing sensitivity but delivering modest whitening gains. Their non-custom application creates uneven coverage versus gels or strips, making them the least effective option.
Long-Term Oral Health Benefits of Professional Whitening
Professional whitening delivers sustained aesthetic improvements while guaranteeing your commitment to extensive oral care. This clinical approach provides improved dental aesthetics through FDA-approved agents that minimize enamel damage while achieving results lasting 12 months or more. You’ll experience reduced chairside time—just 60-90 minutes for treatments lightening teeth up to 8 shades.
Long-term benefits include:
- Enhanced oral hygiene awareness through post-treatment education on brushing, flossing, and dietary modifications
- Preventive health integration via professional assessments identifying underlying conditions before treatment
- Enamel protection protocols using barriers and desensitizing agents customized to your oral health history
- Sustained maintenance guidance with custom take-home trays enabling controlled touch-ups between professional sessions
You’ll maintain control over your dental wellness while professional oversight secures safe, effective, evidence-based whitening outcomes.
When Teeth Whitening May Not Work for Your Dental Condition
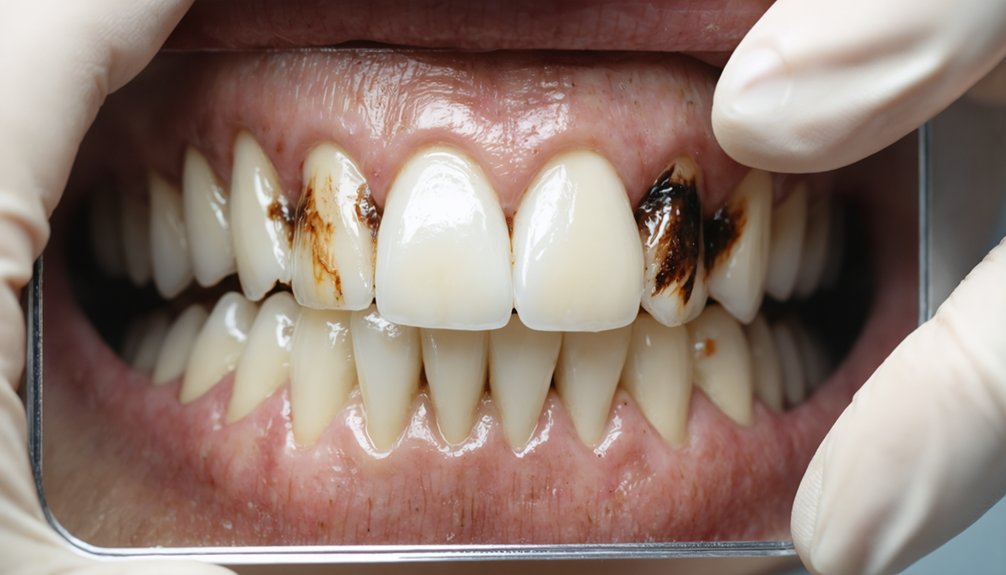
Why doesn’t teeth whitening produce uniform results for everyone? Pre-existing dental problems greatly limit whitening effectiveness. If you have untreated cavities, bleaching agents penetrate decayed areas, causing pain without addressing underlying decay. Gum disease creates additional complications as whitening chemicals irritate inflamed tissues and bleeding gums.
Dental restorative issues present another challenge. Your crowns, bridges, veneers, and fillings won’t respond to bleaching agents like natural teeth, resulting in mismatched coloring. Restorations remain their original shade while surrounding teeth lighten, creating uneven results that may require costly replacement.
Enamel erosion or thin enamel increases your demineralization risk. High-concentration peroxide can soften enamel and increase permeability, revealing yellow dentin beneath. Pre-existing sensitivity heightens during treatment, particularly when aggressive whitening methods penetrate compromised enamel structures.
Finding the Right Balance Between Effectiveness and Safety
Understanding which dental conditions limit whitening success helps you make informed decisions about treatment selection. Balancing effectiveness with safety requires compliance with instructions and patient communication with your dentist. Consider these evidence-based factors:
Effective whitening depends on understanding your dental health, following professional guidance, and weighing treatment benefits against potential sensitivity risks.
- Peroxide concentration trade-offs: Professional treatments deliver faster results (several shades in one visit) but cause sensitivity in 43-80% of users, while OTC products work gradually over two weeks with lower risk profiles.
- Non-peroxide alternatives: PAP (ΔE 6.6) and sodium bicarbonate (ΔE 7.5) provide gentler options than hydrogen peroxide (ΔE 9.6), though with reduced efficacy.
- Sensitivity management: Desensitizing toothpaste effectively mitigates temporary discomfort without compromising results.
- Personalized protocols: Dentist-recommended regimens account for restorations, existing sensitivity, and desired outcomes while maintaining enamel integrity through proper application timing and frequency.
Frequently Asked Questions
Can Whitening Damage Existing Dental Work Like Crowns or Fillings?
No, whitening won’t damage your crowns or fillings—the materials resist bleaching agents. However, you’ll experience enamel sensitivity and gum irritation on natural teeth during treatment, while restorations remain unchanged, potentially creating color mismatches you’ll need to address.
How Often Should I Whiten My Teeth Safely?
Like maintaining a car’s finish, you’ll need whitening frequency recommendations based on your method: professional in-office every 12–18 months, at-home kits every 6–12 months, preventing sensitive tooth exposure while preserving enamel integrity through controlled intervals.
Does Teeth Whitening Help Prevent Gum Disease?
No, teeth whitening doesn’t prevent gum disease. You’ll need healthy gums before whitening due to gum irritation potential from bleaching agents and enamel sensitivity concerns. Clinical evidence confirms whitening offers no therapeutic benefit for preventing or treating periodontal conditions.
Why Do Front Teeth Stay Cleaner Than Molars After Whitening?
Like Cinderella’s transformation, you’ll notice front teeth stay cleaner due to uneven tooth exposure driving your heightened motivation and differential stain removal. You preferentially maintain visible areas post-whitening (1.33±0.09 vs 2.45±0.07, p<0.05), controlling esthetic outcomes.
What Concentration of Peroxide Is Safest for Home Use?
You’ll find 3-6% hydrogen peroxide safest for home use, allowing you to control teeth sensitivity levels through proper whitening application techniques. The ADA recommends 10% carbamide peroxide as equally safe, giving you effective results with minimal risk.