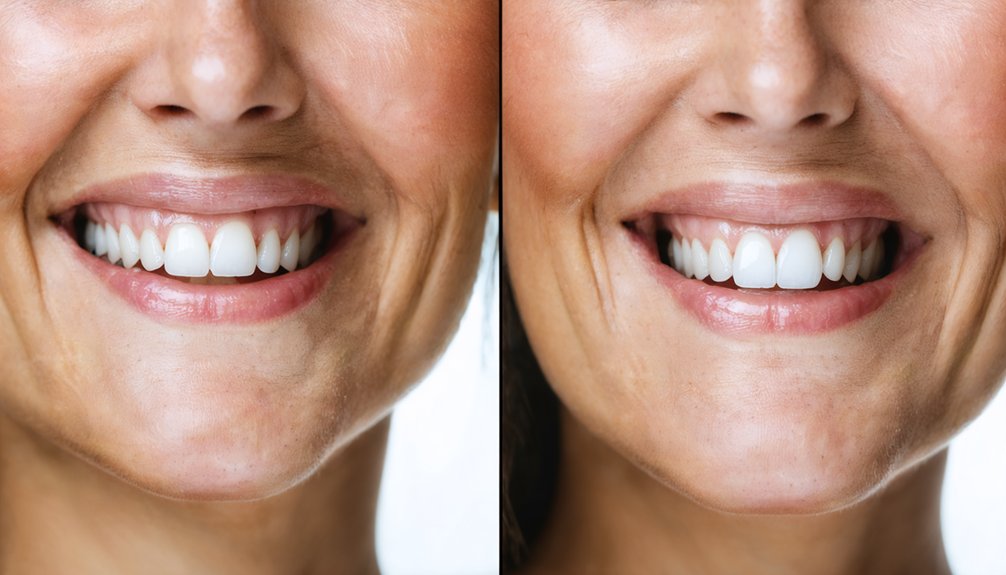
After 50, you’ll face unique whitening challenges as your thinned enamel reveals more yellow dentin while reducing treatment effectiveness. Studies show 36.8% color improvement over three weeks, though results vary based on enamel condition. Professional treatments ($300-$1,500) deliver 8-shade improvements in 60-90 minutes, while at-home options ($100-$600) achieve 3-6 shades over 10-14 days. You’ll likely experience increased sensitivity due to exposed root surfaces, requiring 10-15% peroxide formulations with desensitizing agents. Understanding your specific dental anatomy determines ideal treatment selection.
Key Takeaways
- Aging thins enamel and exposes yellow dentin, making teeth appear darker and potentially reducing whitening effectiveness compared to younger adults.
- Professional in-office treatments cost $300-$1,500 but deliver immediate 8-shade improvements in 60-90 minutes with longer-lasting results.
- At-home whitening systems are more affordable at $100-$600 but require 10-14 days of daily applications for 3-6 shade improvements.
- Tooth sensitivity affects 30-78% of users; manage it with lower-concentration products, desensitizing toothpaste, and avoiding temperature extremes post-treatment.
- Studies show 36.8% color improvement over three weeks with significant satisfaction increases, though deeper age-related stains may resist home methods.
How Aging Affects Your Teeth and Whitening Results
Your teeth undergo substantial structural and compositional changes after age 50 that directly impact whitening efficacy and treatment tolerance. Enamel thinning impacts whitening outcomes as decreased thickness reveals more underlying yellow dentin, requiring stronger peroxide concentrations to achieve visible results.
Your enamel’s increased brittleness and reduced permeability alter bleaching agent penetration patterns, potentially causing uneven color correction. Recession impacts treatment sensitivity greatly—exposed root surfaces lack protective enamel and respond poorly to whitening agents while experiencing heightened discomfort.
The calcification of organic matter between enamel prisms creates resistant staining that standard treatments can’t effectively address. Your existing restorations won’t whiten with natural tooth structure, creating color mismatches. Combined with decreased pulp volume and sclerotic dentin formation, these age-related modifications necessitate modified whitening protocols and realistic outcome expectations.
The Effectiveness of Whitening Treatments for Older Adults
Given these age-related modifications to dental structure, whitening treatments still produce measurable color improvements in adults over 50, though with important limitations. Research demonstrates a 36.8% improvement in tooth color over three weeks, with significant increases in color satisfaction (p<.001). However, whitening safety considerations become more critical as you age.
Adults over 50 can achieve notable whitening results—36.8% improvement in three weeks—but safety considerations intensify with age-related dental changes.
You’ll experience specific challenges:
- Thinning enamel reduces visible whitening effects as underlying dentin becomes more apparent
- Increased tooth sensitivity from enamel erosion or gum recession intensifies during treatment
- Deeper stains from decades of aging, smoking, or dietary factors resist home whitening methods
- Restorative materials like crowns don’t respond to bleaching agents, creating potential color mismatches
Professional consultation enables assessment of your gum health and minimizing treatment discomfort through lower concentration products or treatment breaks.
Professional vs. At-Home Whitening Options
When selecting a whitening method after 50, you’ll choose between in-office professional treatments that deliver immediate multi-shade improvements in one hour, dentist-supervised take-home kits with custom trays for gradual results over several weeks, or over-the-counter products with limited efficacy on age-related intrinsic discoloration.
In-office procedures using high-concentration hydrogen peroxide (15-43%) with protective barriers provide the most predictable outcomes but cost substantially more than professional take-home systems (10-22% carbamide peroxide), which offer controlled application ideal for sensitivity management.
Over-the-counter strips and gels contain legally restricted peroxide concentrations that primarily address surface stains rather than the deeper yellowing characteristic of aging enamel.
In-Office Treatment Advantages
Professional in-office whitening delivers transformative results that at-home alternatives can’t replicate, primarily due to the substantially higher hydrogen peroxide concentrations permitted under clinical supervision. You’ll achieve noticeable shade improvement in a single session through customized application protocols tailored to your specific dental condition.
Critical advantages include:
- Accelerated outcomes: Light-activated gel systems produce immediate dramatic brightening unattainable through gradual at-home methods
- Enhanced agent penetration: Professional-grade concentrations target intrinsic discoloration beneath enamel surface
- Real-time adjustments: Monitored efficacy allows practitioners to modify intensity based on sensitivity responses
- Extended durability: Intensive treatment protocols create longer-lasting results compared to over-the-counter alternatives
Your dentist manages gum protection, addresses age-related enamel concerns, and coordinates shade matching with existing restorations—oversight impossible with unsupervised products.
At-Home Product Effectiveness
At-home whitening systems for patients over 50 demonstrate measurably different performance characteristics than in-office protocols, achieving ΔE values around 2.0 through carbamide peroxide concentrations of 10-16%. You’ll find that cost effectiveness favors these methods, though product safety considerations reveal sensitivity incidence ranging from 30-78% of users.
Your results will take longer due to age-related enamel thinning and dentin darkening, making over-the-counter products with regulatory-limited hydrogen peroxide concentrations less effective on deep intrinsic stains. While 15% carbamide peroxide formulations with fluoride deliver comparable long-term whiteness to professional treatments, you won’t achieve immediate dramatic transformation.
Physical pain subscale increases (4.84 to 7.10) indicate temporary quality-of-life reduction, though sensitivity typically resolves within days. Clinical trials confirm significant color change, but temper expectations for youthful-level brightness restoration.
Cost and Time Considerations
Budget allocation for teeth whitening requires understanding the stark cost-performance differential between professional in-office treatments ($300-$1,500, averaging $575-$792 depending on technology) and dentist-provided take-home systems ($100-$600, typically $375-$500 for custom trays). Since insurance excludes cosmetic procedures, you’ll need upfront payment plans or treatment payment options.
Time-efficiency comparison:
- In-office procedures deliver immediate results in 60-90 minutes (laser treatments compress to 30-60 minutes)
- Take-home systems require daily 1-3 hour applications across 10-14 days
- Professional treatments achieve 8-shade improvements versus 3-6 shades at-home
- Results longevity: in-office maintains 6 months-3 years; take-home sustains 4-6 months
Your decision hinges on prioritizing immediate, dramatic outcomes against gradual, budget-conscious whitening protocols.
Managing Tooth Sensitivity During Treatment
Tooth sensitivity represents one of the most prevalent adverse effects you’ll encounter during whitening procedures, with clinical studies documenting occurrence rates up to 78% among patients receiving professional bleaching treatments. Peroxide agents penetrate tooth structures, generating oxidative free radicals that inflame pulpal nerves.
You’ll minimize discomfort by implementing strategic product application techniques: select lower-concentration formulations (10-15% peroxide) with shortened contact intervals, and incorporate pre-treatment desensitizing toothpaste containing potassium nitrate two weeks before initiating bleaching. Managing sensitivity through hygiene requires maintaining consistent twice-daily brushing and flossing protocols.
Apply desensitizing agents directly to affected teeth post-treatment, avoid temperature extremes for 48-72 hours, and utilize 5% sodium fluoride varnish for extended relief. Contact your dental provider if sensitivity persists beyond one week, as this indicates potential underlying structural complications requiring professional intervention.
Expected Duration and Longevity of Results
After successfully traversing discomfort management protocols, you’ll want to understand realistic timeframes for maintaining your enhanced dental aesthetics. Professional in-office treatments deliver 12-18 months of brightness with proper maintenance requirements, while high-concentration protocols can extend results up to three years. Age-related enamel thinning may accelerate relapse, necessitating strategic planning.
Professional whitening treatments maintain brightness for 12-18 months, though high-concentration protocols may extend results up to three years with proper care.
Duration varies by modality:
- Professional in-office: 6 months to 3 years depending on concentration
- Take-home custom trays: 6-12 months with compliant application
- Over-the-counter products: 3-6 months requiring frequent reapplication
- Maintenance touch-ups: Extend results 2+ years when scheduled appropriately
Optimize longevity through disciplined oral hygiene, tobacco avoidance, and limiting chromogenic beverages. Ideal application timing for touch-up treatments occurs before visible relapse begins, typically at six-month intervals, preserving cumulative brightness while minimizing retreatment intensity.
When Whitening May Not Work for You
Certain intrinsic discolorations resist peroxide-based bleaching agents, particularly tetracycline staining and trauma-induced chromogenic changes that penetrate deep into dentin structures.
Your existing dental restorations—including crowns, bridges, and composite veneers—won’t respond to whitening treatments, creating potential color mismatches with your newly bleached natural teeth.
These limitations necessitate a thorough dental assessment before initiating any whitening protocol to establish realistic outcome expectations.
Medication and Trauma Stains
While surface stains typically respond well to whitening treatments, intrinsic discolorations from medications and trauma present significant challenges that you’ll need to understand before pursuing bleaching protocols. Intrinsic stain identification determines your treatment trajectory, particularly with tetracycline exposure during tooth development or trauma-induced pigmentation from blood breakdown products.
Medication and trauma stains exhibit distinct limitations:
- Tetracycline stains require 12 months of treatment versus 6 weeks for extrinsic discoloration
- Professional bleaching achieves moderate lightening but rarely complete resolution
- Trauma-related nerve damage creates deeply embedded pigments resistant to penetration
- Over-the-counter products lack sufficient potency for meaningful results
Customized treatment plans often necessitate combining initial whitening attempts with veneers or bonding. Clinical trials demonstrate 73% of patients achieve 2+ shade guide units improvement, though complete stain removal remains unlikely for intrinsic discolorations.
Dental Restorations Won’t Whiten
Beyond intrinsic staining limitations, your dental restorations create permanent color boundaries that bleaching agents can’t overcome. Crowns, veneers, implants, and fillings maintain their original shade because peroxide-based whiteners penetrate natural enamel pores but lack sufficient strength to alter nonporous porcelain or composite materials.
Whitening natural teeth while restorations remain unchanged produces visible color mismatch, with studies documenting ΔE values exceeding the detectable threshold of 5 units. This discrepancy becomes particularly pronounced with silver amalgam fillings and older crowns.
Strategic timing proves essential: you’ll achieve uniform results by whitening before placement, allowing your dentist to match prosthetic shades to your lightened teeth. For existing restorations, replacement options provide the only solution to eliminate color inconsistencies post-whitening.
Professional consultation prevents aesthetic complications and guarantees coordinated treatment sequencing for ideal outcomes.
Special Considerations for Mature Patients
Several physiological changes distinguish teeth whitening protocols for patients over 50 from standard adult treatments. Your dentist must evaluate age-related factors before recommending specific bleaching concentrations and application methods.
Age-related enamel thinning and gum recession demand customized whitening protocols with adjusted peroxide concentrations for patients over 50.
Critical assessment areas include:
- Enamel thickness measurements — Thinner enamel requires lower-concentration peroxide formulations to guarantee no irreversible damage and heightened sensitivity
- Gum health considerations — Recession exposes vulnerable dentin surfaces that react adversely to standard whitening agents
- Restoration inventory — Existing crowns, bridges, and fillings won’t respond to bleaching, necessitating color-matching strategies
- Sensitivity thresholds — Your mature teeth typically require desensitizing treatments before and after whitening sessions
Professional supervision certifies your dental hygiene habits support treatment outcomes while minimizing risks associated with compromised enamel integrity and existing oral health conditions.
Making the Most of Your Whitening Investment
Maximizing return on your whitening investment requires strategic decisions aligned with your oral health status and realistic outcome projections. Customized treatment plans account for your enamel thickness, gum recession severity, and existing dental restorations—factors that greatly impact outcomes in patients over 50. Professional in-office procedures deliver superior results through higher-concentration agents adjusted specifically for thinning enamel, whereas generic over-the-counter products can’t address deep stains accumulated over decades.
Appropriate product selection begins with thorough dental assessment. You’ll achieve best value by addressing underlying conditions—cavities, gum disease—before initiating whitening protocols. Clinical evidence demonstrates 36.8% color improvement over three weeks in mature patients, with sustained satisfaction (p<0.001) when combining professional treatment with disciplined post-procedure maintenance. Your investment's longevity depends on consistent fluoride toothpaste use, daily flossing, dietary modifications limiting chromogenic substances, and scheduled dental evaluations.
Frequently Asked Questions
Can Teeth Whitening Damage Dental Work Like Crowns or Bridges?
Ironically, whitening won’t damage your crowns—they’re immune to bleaching agents. However, your existing dental work condition remains unchanged while natural teeth lighten, creating mismatched shades. Whitening treatment side effects include potential restoration deterioration from over-the-counter products.
Are There Medical Conditions That Prevent Teeth Whitening After 50?
Yes, several conditions prevent whitening after 50. You’ll face contraindications with diabetes, melanoma, heart problems, chemotherapy, or liver disease. Dental sensitivity concerns and increased tooth staining from medications also disqualify you from treatment until resolved.
How Much Does Professional Teeth Whitening Typically Cost for Older Adults?
You’ll pay $300-$1,200 for professional whitening, regardless of age. Average whitening costs don’t increase after 50, though your dentist may recommend gentler older whitening options like custom trays ($300-$600) over aggressive laser treatments for sensitive teeth.
Will Whitening Products Affect Medications I’m Currently Taking?
Whitening products won’t affect your prescription medications’ interactions systemically. However, you’ll need to disclose all medications because they impact over-the-counter whitening effectiveness and oral health. Heart medications particularly require professional assessment before whitening treatment.
Can I Whiten My Teeth if I Have Gum Disease?
You shouldn’t whiten with active gum disease due to gum health considerations and severe tooth sensitivity concerns. Whitening agents cause tissue damage and increased inflammation. Wait until your periodontal treatment resolves, then proceed under professional supervision with protective measures.