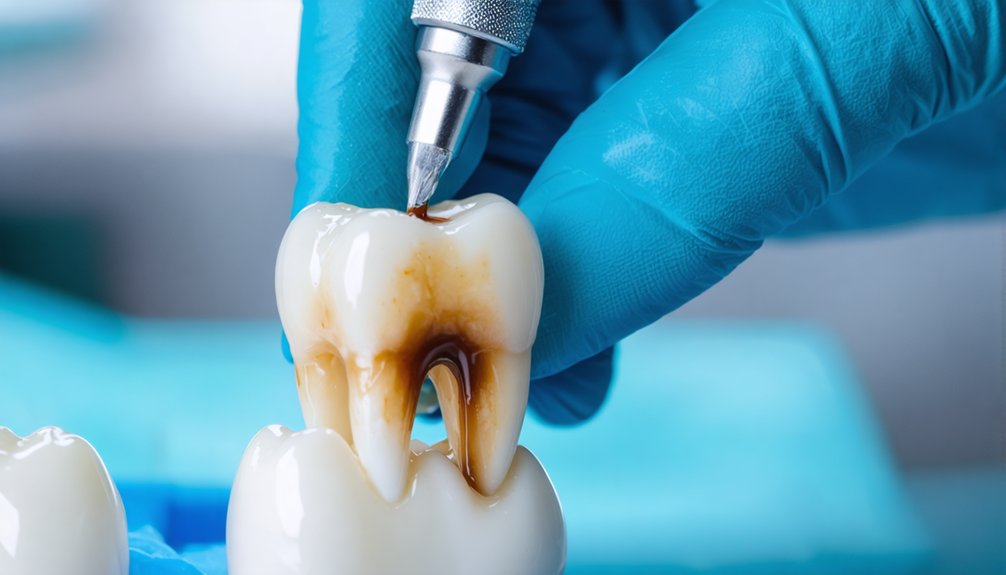
You’ll find fluoride stain removal depends on your fluorosis severity. Mild cases respond well to professional whitening systems using high-concentration bleaching agents, while moderate staining benefits from enamel microabrasion that removes the outer 0.2mm of affected enamel. Severe cases with brown mottling and structural defects require advanced interventions like resin infiltration techniques or porcelain veneers. Your dentist can combine these approaches—microabrasion followed by at-home bleaching delivers ideal results. The following sections explore each treatment modality’s clinical protocols and expected outcomes.
Key Takeaways
- Fluoride stain severity ranges from mild white streaks to severe brown discoloration with pitting, determining appropriate treatment approach.
- Professional whitening using high-concentration bleaching agents effectively treats mild-to-moderate fluorosis under dentist supervision with customized trays.
- Enamel microabrasion removes surface stains less than 0.2mm deep through chemical dissolution and mechanical abrasion techniques.
- Combining microabrasion with at-home bleaching delivers superior results for generalized fluorosis with varying stain depths.
- Severe fluorosis requires advanced solutions including resin infiltration, high-concentration fluoride treatments, or porcelain veneers for definitive restoration.
Understanding Fluoride Stains and Their Severity Levels
Dental fluorosis manifests in varying degrees of severity, each characterized by distinct clinical presentations that range from barely perceptible cosmetic changes to significant structural compromise.
Fluorosis severity spans a clinical spectrum—from minimal aesthetic alterations to substantial enamel degradation requiring therapeutic intervention.
In mild cases, you’ll observe white opaque streaks affecting less than 50% of tooth surfaces—primarily a cosmetic concern with enamel remaining functional. Moderate fluorosis presents with widespread brown staining across affected surfaces, though structural integrity stays largely intact.
Severe fluorosis represents an adverse health effect, featuring confluent pitting, hypoplastic changes, and poorly mineralized enamel that’s prone to chipping and decay. Understanding these fluoride exposure effects is essential for treatment planning.
While mild-to-moderate cases demonstrate caries resistance, severe natural tooth discoloration indicates compromised enamel requiring immediate intervention to prevent further deterioration and sensitivity.
Professional Teeth Whitening Solutions for Fluoride Discoloration
Professional teeth whitening represents the first-line treatment option for mild fluorosis cases, utilizing concentrated hydrogen peroxide or carbamide peroxide to oxidize chromogenic materials within enamel.
In-office procedures deliver immediate results through high-concentration bleaching agents applied during single appointments, while dentist-supervised take-home kits provide gradual whitening suitable for mild-to-moderate discoloration.
You’ll need to ponder your age and overall oral health status before pursuing professional whitening, as dentists must evaluate for contraindications such as active tooth decay, gum disease, or extensive fluorosis that may worsen in appearance post-treatment.
In-Office Whitening Effectiveness
When fluoride stains compromise your smile, in-office whitening treatments offer the most potent chemical intervention available, utilizing high-concentration hydrogen peroxide or carbamide peroxide formulations that penetrate enamel to oxidize discolorations at the dentin level. Professional calibration guarantees controlled delivery systems that over-the-counter products can’t imitate.
However, treatment limitations exist specifically for fluorosis cases. Unlike extrinsic stains from coffee or wine—which demonstrate 94.45% stain area reduction—fluorosis represents hypermineralized enamel rather than surface discoloration. This structural difference produces variable outcomes: mild cases respond adequately, while moderate-to-severe fluorosis shows minimal improvement. The whitening process may paradoxically enhance stain visibility through dehydration effects, making white spots more pronounced against bleached enamel.
Clinical supervision permits your dentist to determine candidacy and recommend alternative interventions like bonding or veneers when whitening proves inadequate.
Take-Home Professional Kits
For patients seeking controlled whitening intervention between clinical visits, custom-fitted trays loaded with moderate-concentration peroxide gels (typically 10-20% carbamide peroxide) provide sustained contact that maximizes oxidative penetration while minimizing soft tissue exposure. These home use whitening kits offer predictable results through extended wear protocols spanning 2-4 weeks.
Professional take-home systems demonstrate superior efficacy compared to over the counter treatment options through:
- Customized tray design preventing gel migration and ensuring uniform tooth coverage
- Higher peroxide concentrations achieving deeper stain oxidation while maintaining enamel integrity
- Professional monitoring protocols allowing treatment adjustments based on individual response
This approach enables you to maintain consistent whitening progress with professional oversight, particularly valuable when addressing fluorosis-related discoloration requiring extended oxidative intervention beyond single clinical appointments.
Age and Safety Considerations
Patient age fundamentally shapes both treatment selection and protocol implementation when addressing fluorosis-related discoloration through professional whitening interventions. For pediatric patients aged 10 and under, you’ll prioritize enamel preservation through non-invasive sodium hypochlorite bleaching rather than restorative alternatives. Single appointment whitening lasting 25-30 minutes achieves acceptable aesthetic outcomes without compromising developing tooth structure.
Professional supervision guarantees FDA-approved formulations containing controlled peroxide concentrations, protective barriers for soft tissue, and thorough pre-treatment evaluation of candidacy. Post treatment sealing with clear resin composite bonding agents protects hypomineralized enamel surfaces in younger patients while addressing organic material penetration.
You can manage sensitivity through desensitizing toothpaste containing potassium nitrate, fluoride applications, and high-fluoride products applied via custom trays pre-treatment. Temporary sensitivity typically resolves within 24-48 hours.
Enamel Microabrasion for Superficial Stain Removal
Enamel microabrasion removes superficial fluorosis stains through simultaneous chemical dissolution and mechanical abrasion, utilizing a 6.6% hydrochloric acid compound with silicon carbide or pumice particles applied to enamel surfaces.
The technique effectively eliminates white and brown discolorations less than 0.2mm deep by removing only the demineralized outer enamel layer while creating a smooth, glassy surface that’s more resistant to future caries.
You’ll achieve ideal aesthetic outcomes when combining microabrasion with professional whitening treatments, particularly for cases of generalized fluorosis where stains vary in depth and severity across multiple teeth.
How Microabrasion Works
Microabrasion employs a dual-action mechanism that combines 6.6% hydrochloric acid with silicon carbide microparticles to simultaneously remove superficial fluoride stains through chemical dissolution and mechanical polishing. The hydrochloric acid pre-conditions your enamel surface by removing approximately 40 micrometers of tissue, while silicon carbide particles mechanically smooth the affected areas. This process eliminates the demineralized outer layer, replacing prism-rich enamel with a densely compacted prism-free region.
Penetration depth considerations determine treatment success:
- Defects less than 0.2mm respond ideally to microabrasion alone
- Lesions exceeding 0.3mm require preliminary diamond bur reduction
- Multiple applications (2-6) address varying stain severity levels
Acid concentration effects influence efficacy, with research demonstrating 18% hydrochloric acid formulations produce superior results compared to 35% phosphoric acid alternatives. The procedure removes only insignificant enamel amounts while permanently eliminating discoloration.
Combining With Whitening Treatments
Treatment protocols that integrate microabrasion with whitening agents deliver superior aesthetic outcomes compared to either modality alone, particularly when addressing mild to moderate fluorosis. You’ll achieve ideal results by combining microabrasion with at-home tooth bleaching, which effectively reduces staining across severity levels. Clinical studies demonstrate that McInnes bleaching technique produces superior outcomes compared to microabrasion as a standalone treatment.
Following microabrasion, you should implement in office fluoride treatments using 2% neutral-pH sodium fluoride gel applied for four minutes to enhance enamel hardness and reduce surface roughness. Subsequently, at home fluoride regimens maintain the glass-like luster and resistance to discoloration. This integrated approach proves particularly valuable for moderate to severe fluorosis cases, where microabrasion alone shows limited efficacy, requiring ten applications compared to five for mild staining.
Resin-Based Treatments: Injection and Bonding Techniques
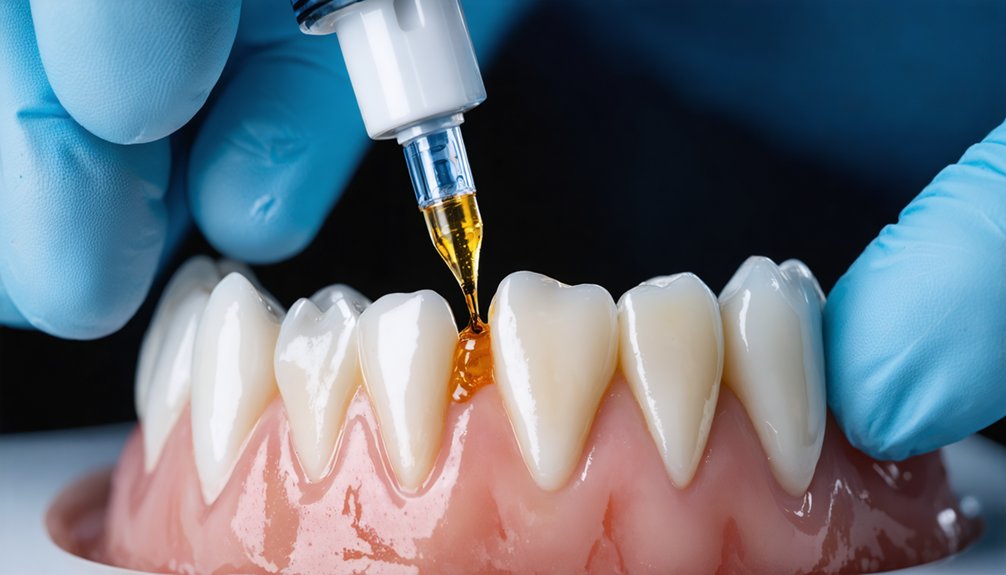
Fluoride-induced enamel opacity presents a unique clinical challenge that requires minimally invasive interventions capable of penetrating hypomineralized tissue without sacrificing sound tooth structure. Enamel infiltration techniques utilize low-viscosity resins that achieve capillary resin penetration deeper than conventional adhesives, accessing fluorosis lesions through natural enamel porosity.
The protocol requires:
- 15% hydrochloric acid gel applied for 120 seconds with microbrush agitation to eliminate hypermineralized surface layers
- 3-minute resin contact time away from light sources for complete capillary infiltration
- Two sequential applications with 40-second polymerization between cycles to minimize residual porosity
You’ll maintain rubber dam isolation throughout erosion and infiltration procedures. This approach eliminates staining while preserving enamel integrity, offering superior aesthetic outcomes compared to traditional restorative methods.
Remineralization Approaches to Restore Tooth Enamel
When hypomineralized enamel responds poorly to resin infiltration or requires biological restoration, remineralization protocols offer evidence-based alternatives that rebuild crystalline structure through ionic exchange mechanisms.
You’ll achieve ideal outcomes by combining high-concentration fluoride (5,000 ppm) with casein phosphopeptide amorphous calcium phosphate formulations like MI Paste Plus, which demonstrate 65% white spot lesion reduction within three months.
Nano-hydroxyapatite toothpastes provide superior remineralization compared to fluoride-only treatments through crystal nucleation mechanisms that mirror natural amelogenin activity.
For early occlusal lesions, you can employ self assembling peptide remineralization agents such as P11-4, which reverse carious lesions with 6-12 month stability.
Implementing quarterly professional fluoride varnish applications alongside daily CPP-ACP use establishes sustained remineralization control, particularly when traditional aesthetic interventions prove contraindicated or insufficient for structural rehabilitation.
Advanced Cosmetic Options: Veneers and Crowns for Severe Cases
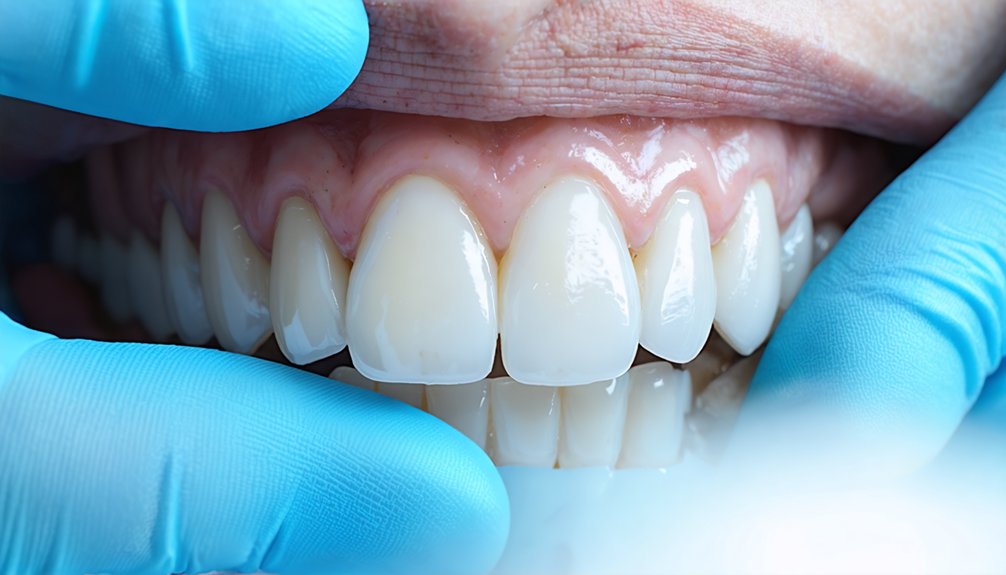
For patients presenting with severe fluorosis characterized by extensive enamel hypoplasia, deep brown discoloration, or structural pitting that resists conservative interventions, porcelain veneers and crowns represent the definitive restorative solution. These prosthetic options deliver predictable outcomes through:
- Porcelain veneers: Custom-fabricated shells requiring minimal (<1mm) tooth preparation, lasting 10–20 years
- Full-coverage crowns: Exhaustive restoration for teeth with significant structural compromise
- Material selection: Lithium disilicate and zirconia demonstrating superior clinical performance
Optimal treatment planning necessitates thorough assessment of enamel integrity and discoloration severity. Patient selection criteria prioritize adults with fully developed dentition, given the permanent nature of tooth modification.
While more invasive than microabrasion or bonding, these restorations outperform conservative alternatives when aesthetic demands exceed their clinical capabilities, providing complete stain concealment and structural reinforcement simultaneously.
Frequently Asked Questions
Can Fluoride Stain Treatments Be Covered by Dental Insurance?
Traversing coverage feels like deciphering fine print. Your dental plan coverage typically classifies fluoride treatments as preventive care at 100%, though insurance eligibility depends on your age and specific plan details. You’ll need to verify your individual benefits directly.
How Long Should I Wait Between Different Fluoride Stain Treatments?
You’ll need specific treatment protocols based on your fluorosis severity. Proper application duration and stain removal schedule vary by technique—microabrasion, resin infiltration, or composite bonding each require different intervals. Consult your dentist for personalized timing recommendations.
Will Removing Fluoride Stains Weaken My Teeth Over Time?
Like polishing marble without cracking its foundation, professional fluoride stain removal preserves enamel integrity. You’ll maintain tooth sensitivity at normal levels since treatments target discoloration, not structure. Your teeth won’t weaken when you follow evidence-based protocols and proper aftercare.
Are There Any Dietary Restrictions After Fluoride Stain Removal Procedures?
You’ll need to follow specific post-procedure guidelines based on your treatment type. Maintain a proper oral hygiene regimen, avoid staining foods temporarily, and schedule professional dental cleanings regularly to preserve results and safeguard ideal tooth integrity long-term.
Can Fluoride Stains Return After Successful Treatment Completion?
Like Sisyphus’s boulder, you might fear permanent stain reappearance, but successfully treated fluorosis won’t return. The underlying fluoride toxicity risks remain fixed in your enamel’s structure, though proper maintenance prevents new secondary staining from developing.