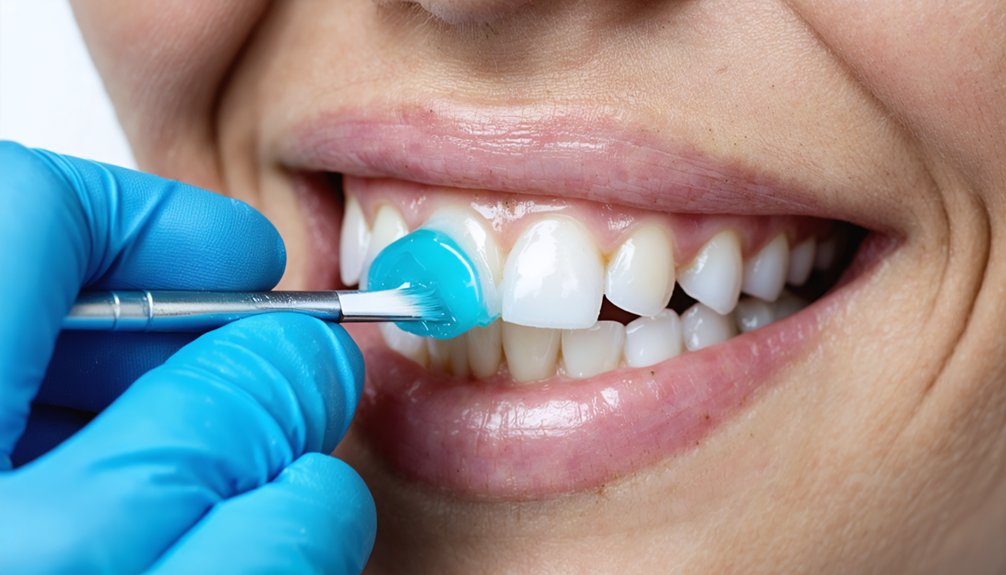
Teeth whitening won’t cause permanent sensitivity, but it can trigger temporary discomfort lasting anywhere from 24 hours to a week. Bleaching agents temporarily open dentin tubules, creating pathways to nerves and causing heightened reactions to temperature changes. These effects are reversible as your enamel rehydrates and tubules close. Pre-existing conditions like worn enamel or gum recession can intensify your experience. The full picture of what’s actually happening — and how to manage it — goes deeper than most people realize.
Key Takeaways
- Teeth whitening does not cause permanent nerve damage; sensitivity is temporary and typically resolves within 24–72 hours post-treatment.
- Bleaching agents temporarily open dentin tubules, creating pathways to nerves, but enamel rehydrates and sensitivity reverses naturally.
- Higher peroxide concentrations may prolong discomfort, but most sensitivity resolves within 1–3 days without special treatment.
- Pre-existing conditions like worn enamel or gum recession can amplify sensitivity but do not make it permanent.
- Consult a dentist if sensitivity persists beyond one week, as professional supervision helps prevent long-term complications.
Can Teeth Whitening Cause Permanent Sensitivity?
When performed correctly under professional supervision, teeth whitening doesn’t cause permanent sensitivity. The evidence is clear: properly administered teeth whitening techniques carry no lasting damage to your teeth or nerves.
Any sensitivity you experience post-treatment is temporary, typically resolving within 24–72 hours.
Post-treatment sensitivity is temporary — most patients find complete relief within 24 to 72 hours.
Pre-existing conditions like enamel erosion or gum recession can amplify discomfort, but whitening itself doesn’t create permanent nerve damage. What you’re feeling is your dentin tubules temporarily opening in response to bleaching agents—a short-term physiological response, not irreversible harm.
Your risk increases when you skip professional supervision and rely on high-concentration over-the-counter products. Choosing clinically appropriate teeth whitening techniques, guided by a qualified dentist, gives you control over both your results and your comfort.
Why Your Teeth Feel Sensitive After Whitening
- Dentin tubule exposure: Peroxide opens microscopic channels connecting your tooth’s surface to its nerve, creating a direct pathway for temperature and pressure signals.
- Enamel dehydration: Bleaching temporarily draws moisture from enamel, leaving teeth hypersensitive to cold drinks, hot beverages, and air exposure.
- Nerve irritation: Hydrogen peroxide penetrates enamel layers, chemically stimulating nerve endings inside the pulp chamber.
These changes are reversible. Your enamel rehydrates, tubules reseal, and nerve irritation subsides — typically within 24-48 hours.
Knowing the mechanism lets you choose lower-concentration products and appropriate application times strategically.
How Long Does Whitening Sensitivity Last?
After whitening, you’ll typically experience sensitivity for 24 to 48 hours, with most cases resolving fully within one to three days.
If you have pre-existing enamel wear, gum recession, or naturally sensitive teeth, your recovery time may extend up to a week.
The concentration of the bleaching agent you used and how closely you followed application guidelines also influence how quickly your sensitivity subsides.
Typical Sensitivity Duration
Visualize your recovery timeline:
- Hours 1-24: Sharp twinges when drinking cold water or breathing cool air — your dentin tubules are temporarily exposed.
- Hours 24-48: Gradual dulling of discomfort as enamel rehydrates and tubules reseal naturally.
- Days 3-7: Residual mild sensitivity in vulnerable individuals, slowly fading without intervention.
You’re not powerless here. Most sensitivity resolves within 1-3 days without special treatment, confirming the process is temporary and physiologically predictable.
Factors Affecting Recovery Time
Recovery time isn’t one-size-fits-all. Several variables directly influence how quickly your sensitivity resolves after whitening.
Your baseline dental health matters most. If you have pre-existing sensitivity, worn enamel, or gum recession, expect longer recovery times than average. The concentration of peroxide used also determines severity—higher concentrations extend discomfort beyond the typical 24-48 hour window.
Effective sensitivity management accelerates recovery. Using potassium nitrate toothpaste before and after treatment reduces nerve irritation considerably. Avoiding temperature extremes during recovery also shortens your discomfort window.
Your whitening frequency compounds cumulative enamel stress. Spacing treatments appropriately allows enamel to remineralize fully between sessions.
Incorporating targeted recovery techniques—like fluoride rinses and room-temperature foods—gives your teeth the environment needed to reseal dentin tubules efficiently.
Who Is Most at Risk for Whitening Sensitivity?
While most people experience only mild, fleeting sensitivity after teeth whitening, certain groups face a particularly higher risk of pronounced discomfort. If you have sensitive teeth, worn enamel, or gum recession, you’re already working with compromised dental defenses. Taking whitening precautions becomes essential rather than optional.
You’re at elevated risk if you fall into these categories:
- Pre-existing sensitive teeth: Your exposed dentin tubules amplify whitening agents’ effects, intensifying nerve irritation considerably.
- Worn enamel: Thinned protective layers offer reduced buffering against peroxide penetration, accelerating discomfort onset.
- Gum recession: Exposed root surfaces lack enamel entirely, making bleaching agents far more aggressive against vulnerable tissue.
Identifying your risk profile before treatment lets you make informed, controlled decisions about whitening protocols and concentration levels.
What Else Can Teeth Whitening Do to Your Teeth?
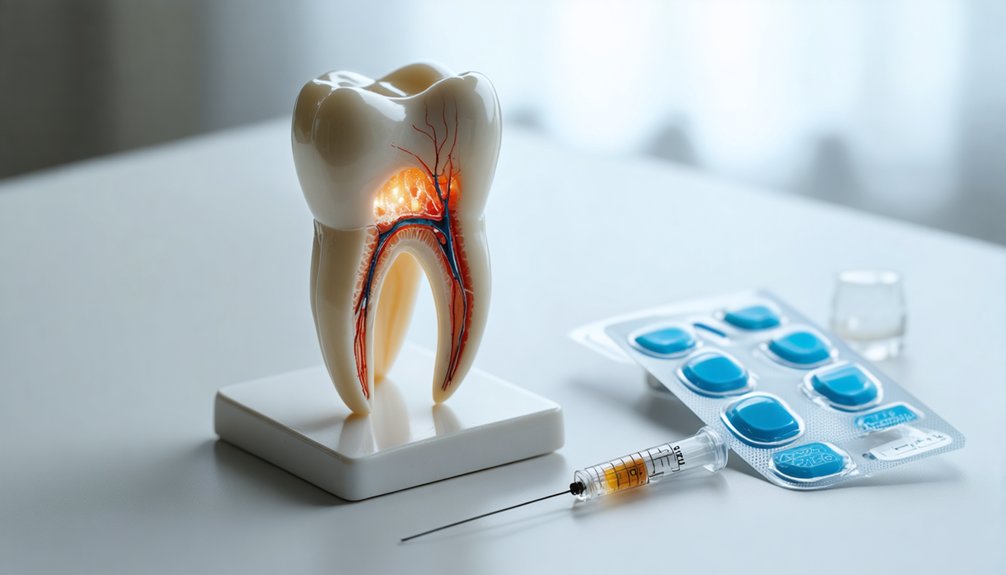
Beyond sensitivity, teeth whitening can produce several other side effects you should recognize.
You may notice gum irritation, uneven coloring, white spots, or a burning sensation in soft tissue when bleaching agents contact damaged areas.
If you observe transparent tooth edges, visible changes in texture, or discomfort extending well beyond a week, these signs may indicate enamel damage requiring professional evaluation.
Common Whitening Side Effects
Teeth whitening doesn’t just cause sensitivity — it can produce several other side effects worth knowing. Beyond sensitivity misconceptions and whitening myths, the procedure carries documented risks you should recognize before treatment.
- Gum irritation: Oxidizing agents contact soft tissue, causing visible redness, burning, or stinging sensations along the gumline.
- Uneven coloring: White spots or inconsistent shading may appear across tooth surfaces during active treatment.
- Enamel changes: Transparent edges or altered tooth texture signal potential structural compromise from overuse.
These effects are typically temporary, but ignoring them increases your risk of lasting damage.
Ill-fitting trays accelerate these outcomes by allowing gel to spread beyond target areas. Knowing what to watch for puts you in control of your whitening experience and overall dental health.
Signs of Enamel Damage
Gum irritation and uneven coloring are manageable concerns, but enamel damage represents a more serious consequence of improper whitening. Watch for transparent tooth edges, visible texture changes, or persistent discomfort extending beyond typical sensitivity timeframes — these signal potential structural compromise.
Unlike temporary sensitivity, enamel doesn’t regenerate naturally, making enamel restoration a complex clinical challenge requiring professional intervention. Excessive whitening frequency accelerates enamel thinning, undermining your long-term dental integrity.
Sensitivity management becomes considerably harder once structural damage occurs, as exposed dentin creates chronic vulnerability to temperature and acidic foods. If you notice these warning signs, discontinue whitening immediately and consult your dentist. Early intervention prevents irreversible progression.
Ill-fitting trays and high-concentration over-the-counter products carry the greatest risk for producing these damaging outcomes.
What Actually Reduces Whitening Sensitivity Before and After Treatment?
Whether you’re whitening for the first time or managing recurring sensitivity, a few evidence-based strategies can meaningfully reduce discomfort before and after treatment.
Apply sensitivity toothpaste containing potassium nitrate or stannous fluoride two weeks before starting your whitening regimen. Temperature management is equally critical — avoid hot coffee, ice water, or cold air exposure for 48 hours post-treatment.
- Pre-treat with sensitivity toothpaste: Massage it directly onto teeth for two minutes nightly, letting active ingredients penetrate dentin tubules before bleaching begins.
- Select lower-concentration peroxide products: Choose formulas around 5-6% hydrogen peroxide to minimize nerve irritation without sacrificing results.
- Control your environment post-treatment: Drink room-temperature water, avoid acidic foods, and use a straw to limit direct tooth contact.
Frequently Asked Questions
Can I Whiten My Teeth While Pregnant or Breastfeeding Safely?
You should avoid teeth whitening during pregnancy due to limited pregnancy safety research. While breastfeeding effects remain unstudied, dentists recommend waiting until after you’ve finished nursing before pursuing any whitening treatments.
Does Teeth Whitening Sensitivity Affect Dental Implants or Crowns Differently?
“You can’t fit a square peg in a round hole.” Whitening effects don’t cause implant sensitivity—implants and crowns lack natural nerve connections, so you’ll experience zero sensitivity response; however, surrounding natural teeth remain fully susceptible.
Can Whitening Treatments Interact Negatively With Prescription Medications I Take?
Whitening interactions with your medications can occur. Certain drugs heighten medication effects on sensitivity or tissue response. You should consult your prescribing physician and dentist before starting any whitening treatment to guarantee safe, controlled outcomes.
Is Professional Whitening Safer for Teenagers Compared to Adult Treatments?
You’re still maturing — teen dental health demands caution. Whitening age guidelines suggest waiting until enamel fully develops, typically around 16. Professional treatments offer safer oversight, but you’d benefit most from consulting your dentist first.
How Soon After Whitening Can I Resume Normal Eating Habits?
You can resume normal eating habits 24-48 hours after whitening. Monitor your sensitivity levels during this window, as whitening duration directly impacts recovery time. Avoid extreme temperatures until discomfort subsides completely.
References
- https://www.bayviewdentalarts.com/blog/can-teeth-whitening-cause-permanent-sensitivity/
- https://www.diamondfamilydental.net/teeth-whitening-sensitivity-causes-and-prevention/
- https://www.glassdentistry.com/why-teeth-whitening-causes-sensitivity
- https://www.manateekidsdentist.com/does-teeth-whitening-hurt/
- https://crest.com/en-us/oral-care-tips/teeth-sensitivity/teeth-whitening-sensitivity-causes-how-to-avoid-it
- https://www.nestdental.com/blog/can-teeth-whitening-cause-permanent-sensitivity
- https://www.norththorntondental.com/truth-about-tooth-sensitivity-after-whitening/
- https://bocaratoncosmeticdentist.com/blog/pain-after-teeth-whitening/
- https://www.suttonpda.com/sensitivity-safety-teeth-whitening/