Start with 10% carbamide peroxide in custom trays for 2-6 months depending on staining severity—first and second-degree cases respond well, while third-degree requires extended protocols. You’ll need bi-weekly assessments initially, then monthly progress documentation. If sensitivity becomes problematic, reduce wear time and apply desensitizing agents rather than abandoning treatment. For stubborn cases, consider KöR Deep Bleaching with refrigerated gels and sealed trays. Fourth-degree staining typically demands restorative solutions, and understanding the complete treatment hierarchy will help you achieve ideal results.
Key Takeaways
- Start with 10% carbamide peroxide in overnight custom trays for 2-6 months depending on staining severity and patient tolerance.
- Yellow-brown stains respond better than grey; realistic expectations include persistent cervical banding in severe cases requiring 6+ months treatment.
- Monitor progress bi-weekly initially, then monthly, emphasizing consistent daily wear to prevent rapid color regression from premature cessation.
- Manage sensitivity using lower concentrations, shorter wear times, desensitizing toothpaste, potassium nitrate gels, and fluoride applications throughout treatment.
- Consider advanced systems like KöR Deep Bleaching for stubborn cases; fourth-degree stains require porcelain-fused-to-zirconia crowns when bleaching fails.
Understanding Tetracycline Staining Severity and Treatment Options
When tetracycline antibiotics bind to calcium ions during tooth development, they create intrinsic discolorations that range from mild yellow-grey to severe blue-black staining with distinct banding patterns. You’ll classify cases into four degrees to establish treatment protocols.
First-degree presents mild, evenly distributed yellowish discoloration. Second-degree shows moderate yellow-brown uniformity. Third-degree exhibits severe blue-grey with significant banding. Fourth-degree remains intractable to bleaching.
Predictive staining factors include dosage duration, accumulative exposure exceeding three grams, and mineralization stage timing. Cyclic administration produces bands; extended use creates homogeneous staining.
For achieving consistent results, you’ll select home bleaching with 10% carbamide peroxide for first through third degrees. Yellow-brown cases respond better than grey. Direct restorations combined with bleaching offer minimally invasive solutions, while severe fourth-degree cases require porcelain-fused-to-zirconia crowns.
Choosing the Right Carbamide Peroxide Concentration
When selecting carbamide peroxide concentration for tetracycline stains, you’ll need to weigh faster results against patient comfort—10% produces less sensitivity while 15-20% accelerates whitening by several months.
You can start conservative patients with 10% concentration for 2-4 weeks to assess tolerance, then progress to 15% if sensitivity remains manageable and treatment timeline needs compression. This stepped approach maintains patient compliance while optimizing the whitening rate for these historically challenging cases.
Balancing Efficacy and Sensitivity
Selecting the appropriate carbamide peroxide concentration for tetracycline-stained teeth requires weighing speed of results against patient comfort during extended treatment. Your concentration selection directly impacts both treatment timeline and adverse effects profile.
Key factors for ideal concentration selection:
- 10% carbamide peroxide produces considerably less tooth sensitivity than 15% or 20% concentrations while maintaining comparable long-term efficacy
- Higher concentrations expedite initial whitening but require scalloped trays and increase discomfort during the 2-12 month treatment period
- More than 55% of maximum lightening occurs within the first month regardless of concentration, with 65% of results remaining after 5 years
Patient compliance factors favor lower concentrations for extended protocols. The 10% overnight tray approach delivers superior results with reduced sensitivity, optimizing adherence throughout your 3-4 month average treatment timeline.
Progressive Concentration Adjustment Strategy
Rather than committing to a single concentration throughout the entire treatment protocol, implement a strategic progression model that begins with lower concentrations and escalates based on patient tolerance and whitening velocity. Start with 10% carbamide peroxide for the first two weeks, establishing baseline tolerance while achieving measurable lightening.
If sensitivity remains minimal, advance to 15% for accelerated results during months two and three when most whitening occurs. Reserve 20% concentrations for resistant cases demonstrating inadequate response. This approach provides predictable safety controls while maintaining treatment momentum.
Suitable gel dispensing adjusts with concentration increases—lower percentages tolerate standard tray loading, while higher formulations require precise, minimal application. Monitor patient feedback biweekly during concentration changes, documenting sensitivity levels and photographic progress to validate adjustment decisions.
Setting Realistic Treatment Timelines for Optimal Results
Understanding the extended commitment required for tetracycline stain reduction prevents patient disappointment and treatment abandonment. You’ll need to establish clear communication pacing from initial consultation through the 3-6 month treatment window, emphasizing that visible results emerge gradually rather than immediately.
Timeline Framework for Patient Follow-Up:
- Mild cases (light yellow/gray): 2-3 months minimum with bi-weekly assessments
- Moderate staining (darker bands): 4-6 months requiring monthly progress documentation
- Severe brown discoloration: 6+ months with realistic expectation that cervical banding may persist
Schedule patient follow-up at 6-8 week intervals to document incremental shade improvements and reinforce treatment compliance. Emphasize that premature cessation causes rapid color regression within days, making consistent daily wear non-negotiable for maintaining progress throughout the entire protocol.
Advanced Whitening Systems for Stubborn Stains
When tetracycline stains resist conventional whitening methods, you’ll need advanced systems engineered specifically for deep dentin penetration. The KöR Deep Bleaching System combines refrigerated gels, custom-sealed trays, and strategic conditioning protocols to achieve measurable results on severe discoloration over several months.
Professional in-office combination treatments like Opalescence Boost paired with high-concentration at-home protocols deliver the extended exposure time necessary to break down intrinsic pigments embedded in dentin layers.
KöR Deep Bleaching System
Tetracycline stains have long resisted conventional peroxide-based whitening treatments due to their intrinsic, deep-seated nature within tooth structure. The KöR Deep Bleaching System addresses this challenge through refrigerated technology that maintains gel potency and specialized delivery trays forming a 1-1.25mm cervical seal. This protocol restores your teeth’s oxygen absorption capability, enabling molecular-level stain breakdown.
Your treatment protocol involves three critical phases:
- Two weeks of at-home application using custom KöR-Seal trays during sleep with 16% carbamide peroxide
- One to two in-office sessions utilizing 34% hydrogen peroxide solution
- Periodic maintenance treatments to sustain permanent results
You’ll achieve 16+ shade improvements in severe cases, with diffuse tetracycline patterns responding maximally. The system targets gray, brown, and blue stains previously deemed untreatable, maintaining effectiveness without dietary restrictions post-treatment.
Professional In-Office Combination Treatments
How do professional in-office combination treatments outperform single-method approaches for tetracycline stains? You’ll achieve superior penetration by layering protocols—starting with high-concentration hydrogen peroxide gel application technique under curing light activation, followed by 14-night at-home carbamide peroxide trays.
Systems like Philips Zoom WhiteSpeed and Opalescence PF 10% deliver 2-8 shade improvements through controlled, deep enamel infiltration over two to six months. Your clinician protects soft tissue with liquid rubber dam before applying gel in 15-30 minute cycles, checking progress between applications. Laser-assisted activation accelerates agent breakdown for stubborn discoloration.
Patient comfort monitoring includes post-treatment desensitizer application. Total chair time runs approximately one hour initially, with gum isolation preventing irritation. Even severe tetracycline cases respond when you combine in-office intensity with extended at-home maintenance.
Managing Tooth Sensitivity During Extended Treatment
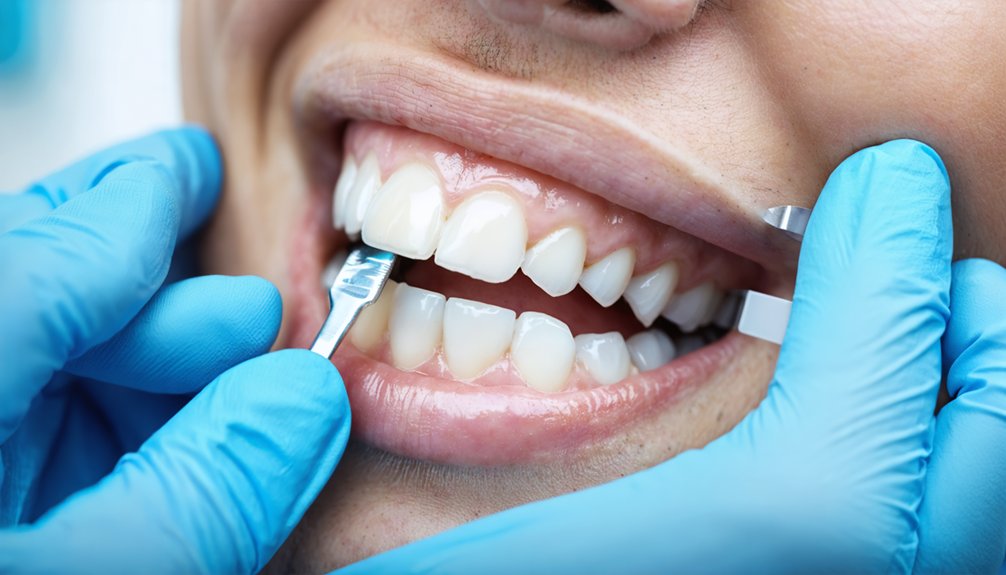
Tooth sensitivity represents the primary challenge in extended whitening protocols for tetracycline-stained teeth, affecting treatment compliance and outcome success. You’ll need systematic desensitizing agent applications to maintain progress through 6-8 week minimum treatment periods.
Three-Tiered Sensitivity Control Protocol:
- Prevention: Start with 10% carbamide peroxide containing potassium nitrate and fluoride (Opalescence PF 15%), then progress to higher concentrations only if sensitivity doesn’t develop.
- Active Management: Apply CPP-ACPF (GC Tooth Mousse Plus) in your bleaching tray for 30 minutes when hypersensitivity occurs, temporarily halting whitening until resolved.
- Home Sensitivity Management: Instruct patients to use desensitizing toothpaste (Sensodyne Repair and Protect) without rinsing, enabling self-directed symptom control between appointments.
Monitor monthly using Vita shade guides while adjusting protocols based on patient-reported discomfort levels.
When to Consider Veneers and Cosmetic Alternatives
When bleaching protocols fail to achieve acceptable shade improvement after 6-8 weeks of maximum-strength treatment, you’ll need to move toward restorative solutions that physically mask the underlying discoloration. Porcelain veneers deliver the most predictable outcomes for third and fourth degree tetracycline stains, with 99% demonstrating excellent marginal adaptation and survival rates exceeding 95% at five years.
Masking gingival staining presents the greatest technical challenge—discoloration extending to the gingival crest requires either increased ceramic thickness or strategic opaque cement selection. Minimally invasive veneer preparation can successfully address grade IV stains when you combine feldspathic ceramics or monolithic lithium disilicate with parallel stratification techniques. Material selection depends on balancing translucency against blockout requirements, with severely stained cases necessitating materials that sacrifice esthetics for complete opacity.
Frequently Asked Questions
Can Tetracycline-Stained Teeth Be Whitened if I Have Existing Dental Restorations?
Yes, you can whiten tetracycline-stained teeth with restorations, but they won’t lighten. You’ll need to replace them post-whitening for color matching. Dental bonding options or veneers as alternative solutions provide predictable results when whitening alone proves insufficient.
How Long Do Whitening Results Typically Last on Tetracycline-Stained Teeth?
Whitening duration extends 5+ years with 65% brightness retention when you maintain proper protocols. Stain reappearance progresses slowly; you’ll need accelerated maintenance touch-ups every 6-8 weeks post-treatment to sustain ideal results and prevent darkening in tetracycline cases.
Is Professional Whitening Covered by Dental Insurance for Tetracycline Staining?
Most dental insurance won’t cover professional whitening for tetracycline staining due to dental insurance limitations classifying it as cosmetic. You’ll likely pay full whitening treatment costs ($500-$1,000) unless you demonstrate medical necessity through documented enamel damage.
Can I Drink Coffee or Wine During Tetracycline Teeth Whitening Treatment?
You’ll need to avoid dark beverages like coffee and wine—yes, even your beloved morning ritual—to prevent staining interference. Maintain oral hygiene rigorously between sessions. Your commitment to dietary restrictions directly determines treatment success and ideal whitening results.
Are There Age Restrictions for Whitening Tetracycline-Stained Teeth?
You’ll need to wait until age 12—the minimum whitening age—when tooth development completes. Starting earlier risks potential dental risks like permanent enamel damage. Once you’ve reached this threshold, you can safely pursue treatment regardless of your current age.



